Motivation and emotion/Book/2020/Hypomania and emotion
What are the emotional characteristics of hypomania?
Overview
[edit | edit source]This chapter focuses on hypomania and emotion and dives more deeply into the emotional characteristics of hypomania. Emotions play an important role in how we think and behave and there are many contrasting theories of emotion however, the major theories discussed are the cognitive and biological approach. Hypomania is episodes of increased mood which are often associated with bipolar disorders and are considered less severe than a manic episode. This chapter will discuss what psychological theory says about hypomania. Lastly, for an interesting extra, this chapter will discuss a study that investigated how marijuana use in young people effects their likelihood of developing hypomania later in life.
Feel free to test what you have learnt from this chapter with the quiz at the end.
|
Focus questions:
|
What are emotions?
[edit | edit source]Defining emotion can be a difficult task. Theorists have come up with different perspectives and there are many contrasting views on the topic. Some theories of emotions are similar but simply occur in different orders. It is commonly agreed emotions are immediate, specific, positive or negative response to internal thoughts or external events. You may feel an emotional response which can affect your mood (Moors, 2009). The components of emotion are: physiological (e.g. racing heart), biological (overt expressions), cognitive (conscious experience) (Moors, 2009). Simply defined, emotions are responses to stimulus that occurs in the environment. The cognitive perspective of emotion states, humans appraise stimulus from the environment, this appraisal (good or bad, scary or boring) elicits an emotional response (Moors, 2009). In contrast, the biological perspective states humans do not need the initial appraisal as emotions are considered an innate physiological response to stimulus (Moors, 2009).
What is hypomania?
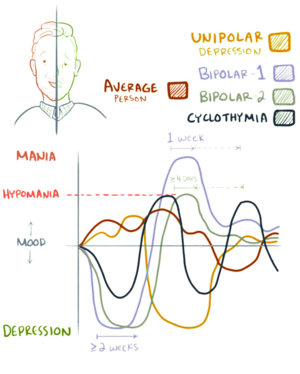
[edit | edit source]Hypomania is a mental disorder characterised by distinct period of elevated mood however, in some circumstances hypomania can present as an extreme irritable mood (Black Dog Institute, 2020). Hypomania is considered as a change from an individuals baseline mood with no psychotic symptoms. Hypomania episodes are considered less severe than a manic episode and are often associated with bipolar disorders and can be referred to as being on the 'bipolar spectrum,' (Goldberg, 2010). The three bipolar disorders (see figure 3) firstly, cyclothymia which involves brief periods of hypomania then brief periods of depression, usually shorter cycles than bipolar. Secondly, bipolar I is classified as having extreme and long mania episodes as well as long depressive episodes. Lastly, bipolar II is characterised by hypomanic episodes which usually do not last as long as the manic depressive episodes. Furthermore, some patients with bipolar may experience psychotic symptoms whereas, patients with cyclothymia will not (Goldberg, 2010).
"People with bipolar II disorder have an increased risk of suicide. About 32% of people with the condition attempt suicide at least once in their life," (Hull, 2020). "Approximately 1.3% of Australians live with a form of bipolar disorder. One in 50 adult Australians experience bipolar disorder each year," (Better Health Victoria, 2020). "More than 66% of people with bipolar disorder have at least one family member with the condition," (Hull, 2020). |
Emotional characteristics of hypomania
[edit | edit source]There are a broad range of emotional characteristics a person may experience whilst in a hypomanic episode and the strength and length of these symptoms differs from person to person. The most common symptoms which are used for diagnosis in the DSM-5 are: fidgetiness and pacing, restlessness (also known as psychomotor agitation), flight of ideas, racing thoughts, grandiose thinking (unrealistic thinking about your powers, talents, or abilities) and a reduced need for sleep without feeling tired (Angst, 1998). During a hypomanic episode an individual can be at risk of making abnormal and engaging in risk taking behaviour, such as, unprotected sex (Black Dog Institute, 2020). Following a hypomanic episode a person may experience depressive symptoms along with guilt and shame of their hypomanic behaviour. These large fluctuations in emotions and mood swings can take a large toll on the person experiencing them and their family and friends.
Causes of hypomania
[edit | edit source]The aetiology of hypomania is complicated and debated and often comes down to the long standing debate of nature versus nurture. The most commonly reported symptoms are as follows:
- alcohol or drug use (Goldberg, 2010)
- changes in sleep patterns (Kusumakar, 2009)
- depression (Goldberg, 2010)
- high levels of stress (Goldberg, 2010)
- side effect of medications (Goldberg, 2010)
- genetic component (Hull, 2020)
Diagnosis
[edit | edit source]Often the diagnosis of hypomania can be missed or misdiagnosed (Singh and Rajuput, 2006). People may not seek medical treatment as their symptoms are not as severe as someone who has bipolar (Black Dog Institute, 2020). Additionally, a person may not seek medical help as symptoms of hypomania, such as, elevated mood, increased sex drive can be pleasurable and therefore people do not deem them necessary to be treated (Colom & Vieta, 2007). The Diagnostic and statistical manual of mental disorders (American Psychiatric Association, 2013) categorises hypomania elevated mood plus three of the following symptoms OR irritable mood plus four of the following symptoms:
- pressured speech
- inflated self-esteem or grandiosity
- decreased need for sleep
- flight of ideas or the subjective experience that thoughts are racing
- easily distracted
- increase in goal-directed activity, or psychomotor agitation
- involvement in pleasurable activities that may have a high potential for negative psycho-social or physical consequences
Additional symptoms include:
- increased sex drive
- risk taking behaviour
- elevated mood
(American Psychiatric Association, 2013)
Alice is a 21 year old university student working part-time as a waitress to pay her rent. Currently, Alice lives in an apartment with her long-term boyfriend, Jason. Recently, Jason has noticed changes in Alice's behaviour, he reports she is staying out late and drinking excessively. Jason has also noticed Alice hasn't been sleeping much lately and is constantly firing out ideas to Jason about new creative tasks. Jason also admits he has noticed Alice has had an increased sex drive and is worried she may cheat on him. Although Jason is not concerned that Alice in immediate danger, he is confused by the seemingly sudden change in behaviour. Jason asks Alice if anything is wrong, however Alice says she is feeling better than she's ever felt. With help from Alice's mum, they manage to persuade Alice to see a doctor for a check-up. The doctor diagnoses Alice with Cyclothymia and states she is experiencing hypomanic symptoms. He prescribes her medication and recommends a psychologist Alice can keep in regular contact with. Several months later Alice's mood stabilises although throughout the next few years she struggles with medication compliance as she complains the prescribes drugs make her feel "numb and flat." |
Hypomania: theoretical basis
[edit | edit source]Many theories have been developed to help aid our understanding of bipolar disorders, however there are only a few that independently investigate hypomania. Psychological theory is essential as it is often the basis of therapies, treatments for patients and education purposes. The cognitive and behavioural approach system are imperative to understanding the psychopathology behind the bipolar spectrum and more specifically hypomania. These theoretical frameworks can aid in diagnosing, categorising and treating the symptoms of hypomania to ensure emotions are stabilised and a patient can enjoy a relatively normal life.
Cognitive approach
[edit | edit source]Colom and Vieta (2007) attempted to translate hypomania into a cognitive model. Hypomania are "positive cognitions that do not correspond to reality," (Colom & Vieta, 2007). These extreme positive cognitions are said to cause unrealistic, self-serving goals and self schemas. Additionally, Colom and Vieta (2007) suggest that a person experiencing a hypomanic undergoes a change in information processing style in which a person experiences extreme "self-overvaluation, positive interpretation of reality and unjustified, excessive optimism," (Colom & Vieta, 2007) which contributes to the severity of symptoms and subsequent behaviours.
Furthermore, in a study by Lex et al 2011 explicit and implicit information processing styles in hypomania were examined. Hypomanic episodes have evidence for depression-related information processing styles. Hypomanic patients have more dysfunctional attitudes than those who are not hypomanic and show a learning deficit for depression related words. This learning deficit is described as potentially being an avoiding or coping strategy. Furthermore, cognitive behavioural therapy is a widely used psychological therapy to treat internal thought processes and can be used for hypomania, (Goldberg, 2020). An individuals, internal thoughts and feelings affects their behaviour and works on changing an individuals negative thinking to improve their behaviours for a positive outcome.
Behavioural approach system (BAS)
[edit | edit source]The behavioural approach system is a system that "integrates approach motivation, personality traits, and behavioural tendencies involved in goal-seeking and reward responsiveness," (Alloy & Abramson, 2010). The BAS regulates an individuals motivation and behaviours to obtain rewards. In people with bipolar disorders it is hypothesised the behaviour approach system easily becomes deregulated. This causes a person to become vulnerable "to extreme fluctuations in activation and deactivation," (Alloy & Abramson, 2010) which subsequently causes a person to experience hypomanic (due to activation) and depressive symptoms (due to deactivation). Behavioural approach system activation occurs in some instances when positive goal-striving emotions are created. A person can become vulnerable to a bipolar disorder when their behavioural approach system is overly sensitive or hyperactive which causes the hypomanic symptoms, (Alloy & Abramson, 2010).
Cannabis use as a risk factor for hypomania
[edit | edit source]
Cannabis is a commonly and widely used drug, approximately one in seven Australians use cannabis everyday (NADK, 2020). Cannabinoids bind to different receptors in the brain and hence, a range of different experiences and symptoms can occur, (Marwaha, 2017). Although cannabis can be used medicinally and legalisation is becoming more common, it is still stigmatised and is commonly believed to be linked to mental health problems. In a 2017 study by Steven Marwaha (et al) was conducted, investigating cannabis use and hypomania in young people. Cannabis use is particularly common among young people whilst their brains are still developing and hence, is a significant area of interest. The study hypothesis was that adolescent cannabis use is associated with hypomania in early adulthood via several potential etiological pathways. Marwaha studies 3,370 participants who used cannabis approximately 2-3 times per week. The study was first conducted in the early 1990s whereby mothers who were pregnant agreed to have their children be a part of the study. When the child was 17 years of age, they were questioned about their cannabis use. Questions such as: if they had ever used cannabis and if so, how frequently? Following this, at age 18, participants psychotic symptoms were assessed (hallucinations, delusions, and experiences of thought interference). Furthermore, depression symptoms of participants were also assessed between the age of 17-18 years old. Finally, when the participant was aged 22-23 they were asked to complete a self-report questionnaire about their experience of manic symptoms, (Marwaha et al, 2017).
Key findings
[edit | edit source]Results of the study showed adolescent cannabis use is independently associated with hypomania in early adulthood; and men were more likely to experience problematic cannabis use and hence, more likely to experience hypomania symptoms. Finally, the study showed childhood physical or sexual abuse is indirectly associated with hypomania, through an increased likelihood of cannabis use. In other words, a person who has been physically or sexually abused was more likely to use cannabis and subsequently more likely to experience hypomanic related symptoms (Marwaha et al, 2017).
Quiz
[edit | edit source]Choose the correct answer and click "Submit"
Conclusion
[edit | edit source]Hypomanic episodes are milder versions of manic episodes and are classed under bipolar disorders. These episodes are disruptive to an individuals life and can cause significant stress on family and friends. There are several risk factors including age, gender, family history and drug use. There are many different emotional characteristics of hypomania such as the fidgeting, pacing, reduced need for sleep. Whilst hypomanic episodes can seem pleasant to the individual experiencing them, they put and individual at risk of making decisions they would not normally make. Additionally, following a hypomanic episode individuals will often experience a depressive mood. These fluctuation of emotional states can take an enormous toll on a person. Due to this, it is important a person seeks professional medical help. This can include, medication and psychotherapy. This area of study is extremely important as people with bipolar are more likely to attempt and complete suicide. Hence, making people aware of the signs and symptoms may increase their likelihood of seeking help. With correct diagnosis and appropriate treatment, patients are likely to make significant improvement and recovery, (Hull, 2020). Lastly, this area of study has important implications for future research, diagnosis and education purposes.
See also
[edit | edit source]- Hypomania and motivation (Book chapter, 2020)
- How to manage your emotional well-being
- Lifeline
References
[edit | edit source]American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). Arlington, VA: Author
Angst, J. (1998). The emerging epidemiology of hypomania and bipolar II disorder. Journal of Affective Disorders Volume 50, Issues 2–3, p143-151. DOI: https://doi.org/10.1016/S0165-0327(98)00142-6
Better Health Chanel. (2020). Bipolar Disorder. Victorian State Government. DOI: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/bipolar-disorder
Colom, F., & Vieta, E. (2007). Sudden glory revisited: Cognitive contents of hypomania. Psychotherapy and Psychosomatics, 76(5), 278-88. Retrieved from https://doi.org/10.1016/j.jpsychires.2007.10.01
Goldberg, G. S. (2010). Hypomania: hype or mania? Bipolar Disorders, 12(8), 758-763.
Hull, M. (2020). Hypomania Statistics. The Recovery Village. Retrieved from: https://www.therecoveryvillage.com/mental-health/hypomania/related/hypomania-statistics/
Kusumakar, D., Yatham, L. (2009). Bipolar disorder: A clinician's guide to treatment management. Taylor & Francis, p. 1-17.
Lex, C., Hautzinger,M., Meyer, T. (2011). Cognitive styles in hypomanic episodes of bipolar I disorder. Bipolar disorders. 13. 355-64. 10.1111/j.1399-5618.2011.00937.x.
Marwaha, S., Winsper, C., Bebbington, P., Smith, D. (2017). Cannabis Use and Hypomania in Young People: A Prospective Analysis. Schizophrenia Bulletin, Volume 44, Issue 6, p1267–1274.
MD, J. T. (2015). Caffeine‐induced mania in a patient with caffeine use disorder: A case report. The American Journal of Addictions, 24(4), 289-291
Moors, A. (2009) Theories of emotion causation: A review, Cognition and Emotion, 23:4, 625-662, DOI: 10.1080/02699930802645739
External links
[edit | edit source]- Black Dog Institute. (2020). Bipolar Disorder. Retrieved from: https://www.blackdoginstitute.org.au/resources-support/bipolar-disorder/
- Psychiatry - Mania/Hypomania By Kate Huntington (YouTube)
- Mani, Hypomania, and Cyclothymia - The Mental Breakdown (YouTube)
- National Alcohol and Drug Knowledge, (2020). How often do Australians use cannabis? Retreieved from https://nadk.flinders.edu.au/kb/cannabis/use-patterns/how-often-do-australians-use-cannabis/
