Motivation and emotion/Book/2018/Social anxiety
What is social anxiety, what are its consequences, and how can it be managed?
Overview
[edit | edit source]
Have you ever experienced symptoms such as those discussed in the case study above? When faced with social situations does your heart begin to race? Do you begin to sweat? Does your breathing rate increase and your face begin to blush? Do you worry that people will judge and reject you? If so you may be one of the 8 per cent or 1.3 million Australian adults experiencing social anxiety disorder (SAD) (McEvoy, Grove, & Slade, 2011). Apart from specific phobias, social anxiety disorder is the second most common anxiety disorder worldwide and it has one of the earliest onsets, with 50% of sufferers reporting first onset prior to 12 years of age (McEvoy, & Abbott, 2017). SAD is more common in women than men, with 1.5 times as many women meeting the diagnostic criteria for social anxiety when compared to men (McEvoy, & Abbott, 2017).
SAD tends to have a chronic course, with a median duration of 25 years when not treated (DeWit, Ogborne, Offord, & MacDonald, 1999). In addition to its chronic course, SAD tends to have a high comorbidity with other anxiety disorders and other psychological disorders, such as major depressive disorder and substance use disorder (McEvoy, & Abbott, 2017). SAD and its co-morbid conditions can cause significant interference in an individual's academic, occupational and interpersonal functioning (McEvoy, & Abbott, 2017), because of this, it is highly important to understand the aetiology and management of SAD. Therefore, the following chapter will outline the aeitiology, symptoms and consequences of SAD and explore current treatment options
|
Focus questions
|
What is social anxiety?
[edit | edit source]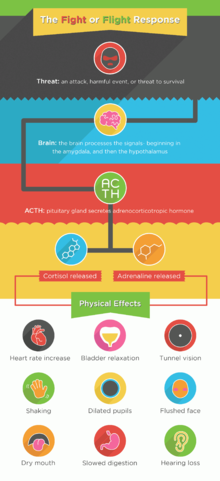
SAD is an anxiety disorder that is characterised by a marked fear or anxiety about one or more social situations in which the individual is exposed to possible scrutiny by others (American Psychiatric Association, 2013). The individual fears that he or she will behave in a way that will be negatively evaluated by others (i.e., will be humiliating or embarrassing). These social situations almost always provoke fear or anxiety and the fear or anxiety is out of proportion to the actual threat posed by the social situation (American Psychiatric Association, 2013). The fear, anxiety, or avoidance is persistent, typically lasting for six months or more and causes clinically significant distress or impairment in social, occupational, or other important areas of functioning (American Psychiatric Association, 2013).
Situations that may provoke social anxiety include having conversations, working in groups, being observed, eating, using public toilets or public speaking (McEvoy, & Abbott, 2017). As can be seen in figure 1, physical and psychological symptoms that are typically experienced by individuals with SAD include,excessive sweating, increased heart rate, blushing, trembling, difficulty breathing, nausea, diarrhoea, excessive worry, feelings of distress in social situations and avoidance of social situations (Beyond Blue, 2018).
As demonstrated in figure 2, these symptoms arise as a result of the flight or fight response, which is the physiological changes that occur in the body when the hormone adrenaline is released in response to a perceived threat (McEvoy, & Abbott, 2017). The fight or flight response is a natural response mechanism that prepares the body to respond to danger (McEvoy, & Abbott, 2017). However, in SAD, the fight or flight response is inappropriately activated in response to social situations, resulting in the physical and psychological symptoms mentioned above (McEvoy, & Abbott, 2017).
|
Video break
Want to learn more about social anxiety? Lets take a 5 minute video Break (van der Schrierf, 2015) for a quick lesson. |
Aetiology and theory of social anxiety disorder
[edit | edit source]No single cause seems to account for the development of SAD, however, several biological, psychological and social factors have been implicated in the development and maintenance of SAD (Rapee, & Spence, 2004). Evidence in the current body of research indicates that SAD may arise from a complex interaction between these biological and psycho-social factors (Rapee, & Spence, 2004).
Biological factors
[edit | edit source]Evidence suggests that genetic factors play a significant role in the development of SAD (Rapee, & Spence, 2004). Research has found that individuals who have a parent with a history of SAD have a two to three fold increase in relative risk of developing SAD (Tillfors, Furmark, Ekselius, & Fredrikson, 2001). It is unclear which specific genes play a role in the development of SAD (Rapee, & Spence, 2004). However, several genes have been implicated, including those involved in the dopamine and serotonin pathways (Rapee, & Spence, 2004).
Psychological factors
[edit | edit source]
Approach/avoidance motivation
[edit | edit source]Approach vs avoidance motivation refers to an innate motivational tendency to approach success and avoid failure (Reeve, 2014). Research has shown that when faced with the possibility of interacting with familiar and unfamiliar peers, children generally follow a standard pattern of initial inhibition and waiting behaviour followed by parallel play and group interaction (Neal, & Edelmann, 2003). The initial inhibition and waiting stage involves a conflict between approach and avoidance motivations, in which children must balance their desire to approach a desired social interaction with their fear of social failure and rejection (Neal, & Edelmann, 2003). This conflict is resolved when the child begins to interact with their peers (Neal, & Edelmann, 2003). However, socially avoidant children (those with a high avoidance tendency) tend to remain in the inhibited waiting stage and tend to engage in solitary play (Neal, & Edelmann, 2003). These innate motivational patterns of avoidance can be further strengthened or weakened through social interaction with peers (Neal, & Edelmann, 2003). Children who encounter neglect or rejection from peers during the initiation of social contact may experience a deep sense of social failure and embarrassment and this exacerbates the existing tendency toward social avoidance (Neal, & Edelmann, 2003). This avoidance motivation combines with an individuals increasing concerns about social evaluation to eventually present as SAD (Neal, & Edelmann, 2003).
Behavioural inhibition
[edit | edit source]Behavioural inhibition refers to a temperament style which is characterised by a consistent pattern of behavioural and emotional responses that an individual displays in response to unfamiliar/novel people, places, situations or objects (Rapee, & Spence, 2004). Individuals with this temperament style generally respond to these novel stimuli with restraint, caution, apprehension and withdrawal and when faced with unfamiliar people, these individuals are usually shy, timid and withdrawn,(Rapee, & Spence, 2004). SAD is significantly more likely to be diagnosed in individuals who at age 2-6 were identified as being high in behavioural inhibition (17%), compared to those who were low in behavioural inhibition (5%) (Rapee, & Spence, 2004).
Cognitive distortions
[edit | edit source]cognitive bias and distortion in social information processing have been found in both socially anxious adults and children (Rapee, & Spence, 2004). When confronted with social situations, these individuals tend to anticipate negative outcomes, negatively evaluate their own performance and experience high levels of negative cognition (Rapee, & Spence, 2004). This tendency to perceive social situations in a threatening way generates anxious emotions and impairs social performance (Rapee, & Spence, 2004). This results in further negative emotions and subsequent social avoidance and adverse social outcomes , which further perpetuates the persons assumption that social events will lead to negative outcomes (Rapee, & Spence, 2004).
Emotional regulation difficulties
[edit | edit source]Empirical evidence has found that individuals with SAD demonstrate dysfunctions in emotional regulation and reduced reward responses when faced with social situations (Helbig-Lang, Rush, & Lincoln, 2015). People with SAD tend to evaluate the experience and expression of intense emotion as a potential threat (Helbig-Lang et al., 2015). In addition to this, individuals with SAD focus their attention on internal emotional states and the suppression of emotional responses during social situations and this results in heightened attention to negative emotions and symptoms of arousal and reduced observation of other people's behaviour and responses (Helbig-Lang et al., 2015). Together, these problems in emotional regulation reduce the cognitive resources that are available for social performance and for interpreting social cues and therefore results in less successful social interactions and maintains negative social expectations and anticipatory anxiety (Helbig-Lang et al., 2015). One recent study found that students who experienced SAD reported higher intensity negative emotions and less effective emotional management strategies than students who did not experience SAD (Helbig-Lang et al., 2015).
Social factors
[edit | edit source]
Adverse life events
[edit | edit source]Adverse life events such as divorce, death, illness, academic failure, family violence, bullying and social humiliation have been implicated in the development of SAD through the processes of classical and operant conditioning (Helbig-Lang et al., 2015). Fear is learned when social interaction is paired with an adverse stimuli, such as particularly embarrassing or humiliating life events (Tillfors, 2004). This classically conditioned fear is then maintained by operant conditioning, when the individual learns that avoiding social situations (the phobic stimulus) can reduce fear and anxiety (Tillfors, 2004).
Parenting traits
[edit | edit source]Parenting traits such as over control, lack of warmth, rejection, over protection, anxiety and over concern with the opinions of others, are known to be associated with the development of SAD (Brook, & Schmidt, 2008). These parenting traits contribute to the development of SAD through both the modelling of dysfunctional and avoidant behaviours and by reducing and restricting opportunities that are available for the child to explore and learn new social skills independently (Brook, & Schmidt, 2008). Retrospective questionnaires of adults with SAD have revealed that individuals with SAD tend to perceive their parents to have been overprotective, rejecting and lacking in warmth (Brook, & Schmidt, 2008).
|
Quiz
|
What are the consequences of social anxiety?
[edit | edit source]SAD is characterised by an early onset, chronic course and high rates of comorbidity (Canton et al., 2012) and can significantly interfere with an individual's social and occupational functioning (Canton et al., 2012). Individuals who suffer from SAD are more likely to access and utilise medical services, receive lower incomes and are less likely to earn university degrees or be employed in professional occupations, when compared to individuals who do not have SAD (Canton et al., 2012). Individuals with SAD are also less likely to develop effective relationships with family, friends and romantic partners and these individuals are at greater risk of suicide (Canton et al., 2012).
How can social anxiety be managed?
[edit | edit source]Social anxiety can be managed through a variety of methods, including both through pharmacological and psychological interventions. Given the complex nature of social anxiety and its treatment it can be understood that all of these methods of management work in tandem to provide adequate management options.
Pharmacological interventions
[edit | edit source]Pharmacological interventions include the use of a range of medications such as selective serotonin re-uptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors (MAOIs) and benzodiazepines (Blanco et al., 2013). Current research has largely found that SSRI'S, such as Paroxetine, sertraline, fluvoxamine and venlafaxine are the most effective medications for reducing the clinical symptoms of SAD (Blanco et al., 2013). SSRIs are therefore recommended for the pharmacological treatment for social anxiety disorder (Blanco et al., 2013).
Psychological interventions
[edit | edit source]Cognitive behavioural therapy (CBT) is currently the most well researched psychological treatment for SAD (Rodebaugh, Holaway, & Heimberg, 2014). CBT includes a range of techniques, such as exposure therapy, mindfulness and progressive muscle relaxation, social skills training and cognitive restructuring(Rodebaugh et al., 2004).
Exposure therapy
[edit | edit source]Exposure therapy aims to expose the individual to the feared social situation and to support them to stay in this situation despite feelings of anxiety(Rodebaugh et al., 2004). With the support of the therapist, the individual will develop a list of feared situations and rank these situations based on the degree of anxiety they provoke(Rodebaugh et al., 2004). The individual is then first exposed to the lowest ranked situation and gradually progresses up the hierarchy to more highly feared situations(Rodebaugh et al., 2004). Exposure to the feared situation can be in vivo or through role play or imagery(Rodebaugh et al., 2004).
Mindfulness and progressive muscle relaxation
[edit | edit source]Mindfulness and progressive muscle relaxation (PMR) are relaxation techniques used to manage physiological arousal symptoms, such as difficulty breathing and increased heart rate, that typically accompany anxiety(Rodebaugh et al., 2004). The individual with SAD is instructed in mindfulness and PMR and asked to practice these techniques during their usual daily activities(Rodebaugh et al., 2004). After these skills have been mastered, the individual with SAD can utilise these techniques during feared social situations(Rodebaugh et al., 2004). Therapy will often utilise mindfulness and PMR during exposure therapy (Rodebaugh et al., 2004).
Social skills training
[edit | edit source]Social skills training aims to teach the individual with SAD practical social skills through a combination of modelling, rehearsal, corrective feedback and positive reinforcement(Rodebaugh et al., 2004). Social skills training is typically used in conjunction with other CBT techniques in order to improve self efficacy and success during social interaction(Rodebaugh et al., 2004).
Cognitive restructuring
[edit | edit source]Cognitive restructuring aims to identify cognitive distortions that are perpetuating the SAD(Rodebaugh et al., 2004). During therapy, the client is supported by the therapist to identify and challenge negative distortions and beliefs, through rational disputation, psychoeducation and monitoring, in order to develop new balanced thoughts(Rodebaugh et al., 2004). The client may also be given homework tasks, which involve monitoring and challenging these thoughts during real life situations (Rodebaugh et al., 2004).
Effectiveness of pharmacological and psychological interventions
[edit | edit source]Meta -analytic studies have found both CBT and pharmacological interventions to be effective treatments for SAD, with moderate to large effect sizes for treatment effectiveness when compared to control groups (Rodebaugh et al., 2004). However, individuals who are receiving pharmacological treatment on its own have been shown to experience higher rates of relapse, when compared with individuals who are receiving a CBT intervention or a combination of both (Blanco et al., 2013). Therefore, it is recommended that individuals receive a combination of both pharmacological and psychological treatment in order to achieve both short term and long term reductions in social anxiety symptoms (Canton et al., 2012).
Conclusion
[edit | edit source]In conclusion, SAD is characterised by a marked fear or anxiety about one or more social situations in which the individual is exposed to possible scrutiny by others and this fear results in physiological and psychological symptoms, such as excessive sweating, increased heart rate, blushing, trembling, difficulty breathing, nausea, diarrhoea, excessive worry, feelings of distress in social situations and avoidance of social situations. These symptoms can severely reduce a persons social and occupational functioning. The exact cause of SAD is not clear. However, the current body of research suggest that SAD may result from a complex interaction between biological, psychological and social factors. SAD can be effectively treated through a combination of pharmacological interventions, such as SSRIs, and psychological interventions, particularly CBT.
See also
[edit | edit source]- Social anxiety (Wikipedia)
- Social anxiety disorder (Wikipedia)
- Specific phobia (Wikipedia)
- Anxiety and gender (Book chapter, 2017)
- Social inhibition (Wikipedia)
- Mindfulness and flow (Book chapter, 2018)
References
[edit | edit source]Beyond Blue. (2018). Social phobia. Retrieved from https://www.beyondblue.org.au/the-facts/anxiety/types-of-anxiety/social-phobia
Blanco, C., Bragdon, L.B., Schneier, F.R., & Liebowitz, M.R. (2013). The evidence-based pharmacotherapy of social anxiety disorder. International journal of neuropsychopharmacology, 16, 235—249. https://doi.org/10.1017/S1461145712000119
Canton, J., Scott, K.M., & Glue, P. (2012). Optimal treatment of social phobia: Systematic review and meta-analysis. Neuropsychiatric disease and treatment, 8, 203—215.https://doi.org/10.2147/NDT.S23317.
DeWit, D.J., Ogborne, A., Offord, D.R., & MacDonald, K. (1999). Antecedents of the risk of recovery from DSM-III-R social phobia. Psychological medicine,29, 569—582. https://doi.org/10.1017/S0033291799008399
Halldorsson, B., & Creswell, C. (2017). Social anxiety in pre-adolescent children: What do we know about maintenance? School of psychology and clinical language sciences, 99, 19—36.https://doi.org/10.1016/j.brat.2017.08.013
Helbig-Lang, S., Rush, S., & Lincoln, T.M. (2015). Emotion regulation difficulties in social anxiety disorder and their specific contributions to anxious responding. Journal of clinical psychology, 71, 241—249. https://doi.org/10.1002/jclp.22135
McEvoy, P., & Abbott, M. (2017). Anxiety disorders. In Reiger, E.(Ed.), Abnormal Psychology(4th ed., pp.41—70). Sydney.: McGraw-Hill Education.
McEvoy, P.M., Grove, R., & Slade, T.(2011). Epidemiology of anxiety disorders in the Australian general population: findings of the 2007 Australian national survey of mental health and wellbeing. Australian and New Zealand journal of psychiatry,45,,957—967. https://doi.org/10.3109/00048674.2011.624083
McEvoy, P.M., Moulds, M.L., Grisham, J.R., Holmes, E.A., Moscovitch, D.A., Hendrie, D., Saulsman, L.M., Lipp, O.V., Kane, R.T., Rapee, R.M., Hyett, M.P., Erceg-Hurn., D.M. (2017). Assessing the efficacy of imagery-enhanced cognitive behavioral group therapy for social anxiety disorder: Study protocol for a randomized controlled trial. Contemporary clinical trials,60,34—41. https://doi.org/10.1016/j.cct.2017.06.010
Neal, J.A., & Edelmann, R.J. (2003). The eitiology of social phobia: Toward a developmental profile. Clinical psychology review, 23, 761—786. https://doi.org/10.1016/S0272-7358(03)00076-X
Rapee, R.M., & Spence, S.H. (2004). The etiology of social phobia: Empirical evidence and on initial model. Clinical psychology review, 24, 737—767. https://doi.org/10.1016/j.cpr.2004.06.004
Reeve, J. (2014). Understanding motivation and emotion(6th ed.).New Jersey:John Wiley & Sons
Rodebaugh, T.L., Holaway, R.M., Heimberg, R.G. (2004). The treatment of social anxiety disorder. Clinical psychology review, 24, 883—908. https://doi.org/10.1016/j.cpr.2004.07.007
Scani, S., Belotti, R., Ogliari, A., & Baltaglia, M. (2016). A comprehensive meta-analysis of cognitive-behavioral interventions for social anxiety disorder in children and adolescents. Journal of anxiety disorders,42, 105—112.https://doi.org/10.1016/j.janxdis.2016.05.008
Tillfors, M. (2004). Why do some individuals develop social phobia? A review with emphasis on the neurobiological influences. Nordic journal of psychiatry, 58, 267—276. https://doi,org/10.1080/08039480410005774
Tillfors, M., Furmark, T., Ekselius, L., & Fredrikson, M. (2001). Social phobia and avoidant personality disorder as related to parental history of social anxiety: A general population study. Behaviour research and therapy, 39, 289—298. https://doi.org/10.1016/S0005-7967(00)00003-6
van der Schrier, S. (2015). You will never see social anxiety the same after watching this [video file]. Retrieved from https://youtu.be/dBZyFMd6La4
External links
[edit | edit source]- Social phobia (Beyond blue)
- Social anxiety disorder (Reach out Australia)
- Social anxiety self help (Centre for clinical interventions)

