Motivation and emotion/Book/2018/Anxiety neurobiology
What are the neurobiological components and treatments of anxiety disorders?
Overview
[edit | edit source]
The statistics
[edit | edit source]Anxiety disorders are generally experienced as recurring intrusive thoughts or concerns. People experiencing anxiety disorders may avoid situations out of worry while also experiencing physical symptoms such as sweating, trembling, dizziness or rapid heartbeat (APA, 2018). Anxiety is the most common mental health condition in Australia. On average, 1 in 4 people, 1 in 3 women and 1 in 5 men will experience anxiety in their lifetime. Every year in Australia, approximately 14% of the population experiences an anxiety disorder of some type (Australian Bureau of Statistics, 2008).
Anxiety according to the DSM-5
[edit | edit source]For healthcare professionals to share common standard criteria for mental health disorders, the American Psychological Association publish the Diagnostic and Statistical Manual of Mental Disorders (DSM) currently in its fifth edition (as of May 2013). The DSM-5 categorises anxiety disorders as sharing excessive behavioural disturbances of fear and anxiety. Fear being the emotional response to a real or perceived immediate threat, while anxiety is the anticipation of a future threat. The autonomic arousal system of the ‘fight or flight’ response is triggered by fear. Anxiety is associated with muscle tension and avoidant behaviours, panic attacks also a prominent feature of anxiety related disorders. To be categorised as an anxiety disorder, rather than just fear or anxiety, the symptoms must be persistent for excessively long period, extending beyond what would be considered appropriate (typically lasting longer than 6 months). Each disorder has a range of diagnostic criteria that must be satisfied for the individual to receive a diagnosis. The DSM-5 also includes relevant information to the disorder such as associated features supporting diagnosis, prevalence, development and course, risk and prognostic features, culture-related diagnostic issues, gender-related diagnostic issues, suicide risk, functional consequences, differential diagnosis and comorbidity. This information can be helpful for practitioners to further inform and protect their patients.

The DSM-5 includes multiple anxiety related disorders, including:
- Separation Anxiety Disorder
- Selective Mutism
- Specific Phobia
- Social Anxiety Disorder
- Panic Disorder
- Panic Attack Specifier
- Agoraphobia
- Generalised Anxiety Disorder
- Substance/Medication-Induced Anxiety Disorder
- Anxiety Disorder Due to Another Medical Condition
- Other Specified Anxiety Disorder
- Unspecified Anxiety Disorder
While Post-Traumatic Stress Disorder (PTSD) and Obsessive-Compulsive Disorder (OCD) share many of the same related symptoms as anxiety related disorders, they are classified into independent chapters, ‘Trauma- and Stressor-Related Disorders” and “Obsessive-Compulsive and Related Disorders,” therefore, this chapter will not go into detail regarding these disorders.
The Goals
[edit | edit source]From the brain structures we will examine below, studies have shown that the early detection of neurological abnormalities may help identify individuals who are more at risk of developing anxiety related disorders (Cohodes & Gee, 2017). This is especially important to consider in relation to children and adolescents and how early identification may enable earlier diagnosis and treatment of anxiety related disorders.
Another goal of studying these brain structures and functions is to come to a greater understanding of the neurotransmitters involved in anxiety related disorders and how they can be manipulated through pharmacology to bring a patient to a normal level of functioning. Since pharmacological treatment has come so far in recent years, it is important to ask which medication is the most effective way to treat different anxiety related disorders.
Measuring activity in the brain
[edit | edit source]There are different ways of measuring the structure and the activity of a brain. The three most commonly used in psychology are the MRI, fMRI and EEG. The aim of measuring the structure and activity of the brain is to determine any abnormalities as compared with subjects from a suitable reference population (Brammer, 2009). As healthcare professionals, this should be done in the most accurate, timely and least intrusive way possible.
Magnetic Resonance Imaging (MRI)
[edit | edit source]Magnetic Resonance Imaging (MRI) is a medical imaging technique used to scan the brain using strong magnetic fields and radiofrequency pulses to generate signals from the brain. These signals are then detected by a radio antenna in the MRI machine and processed by computers to generate images of the brain (McIntyre & Goergen, 2017). One advantage of an MRI is that does not use x-rays or radiation such as that found in CT or PET scans which can be harmful to the body.
Functional Magnetic Resonance Imaging (fMRI)
[edit | edit source]
Functional Magnetic Resonance Imaging (fMRI) involves using the same scanning machine as an MRI and overlaying a functional scan on the image. This scan is used to detect the changes in blood oxygenation in response to neural activity, indicating more active regions of the brain. fMRI is used to create activation maps that show which parts of the brain are active during different mental processes (Delvin, 2016). These activation maps make fMRIs particularly useful for researchers investigating any neurological abnormalities associated with anxiety disorders.
Electroencephalography (EEG)
[edit | edit source]Electroencephalography (EEG) is a test used to measure the electrical activity of the brain. It uses electrodes placed along the scalp to record the brain’s electrical activity over a period of time. An EEG test cannot be used to diagnose mental illness, monitor psychotic conditions or neurologically map the brain structures. It is useful for diagnosing and monitoring conditions such as epilepsy, sleep disorders, brain injuries, head injuries, stroke and dementia (Health Direct, 2018). An EEG test is not a useful test for investigating anxiety related disorders; MRI and fMRI scans are much better equipped for investigating those disorders.
Brain structures involved
[edit | edit source]Several brain structures have been shown to be more active in those suffering from a variety of different psychological disorders (Iorfino, Hickie, Lee, Lagopoulos, & Hermens, 2016). The main brain structures identified as being affected by anxiety related disorders are the amygdala, the prefrontal cortex and the anterior cingulate cortex (ACC).
Amygdala
[edit | edit source]
The amygdala is an almond-shaped cell mass, located in the temporal cortex. It is made up of different groups of cells, called the lateral, basal and accessory basal nuclei – collectively called the basolateral amygdala. Structures surrounding the basolateral amygdala, including the central, medial and cortical nuclei are traditionally called the ‘amydaloid complex’, and together with the basolateral amygdala are collectively called ‘the amygdala’ (Davis & Whalen, 2000). The amygdala is associated with fear and emotional significance of a stimulus (Burton, Westen, Kowalski, & Westen, 2015). Stimulation of the amygdala is associated with autonomic reactions such as the ‘fight or flight’ response, increasing heart rate and blood pressure (Thomas, 2001). A study into lesions of the amygdaloid complex of monkeys in 1956 showed that the lesions on the amygdala diminished the monkey’s normal fear response (Weiskrantz, 1956). Studies indicate that increased amygdala volume may be correlated with increased amygdala reactivity (Cohodes & Gee, 2017). Studies have found that children and adolescents with anxiety related disorders show larger amygdala volumes (Milham & Banich, 2005), and another study in 2010 by Tottenham et al., found that increased amygdala volume predicted symptoms of anxiety in post-institutionalised children. Another study showed that children with anxiety disorders showed exaggerated amygdala responses to fearful faces compared to healthy children, suggesting that the amygdala function is affected by anxiety related disorders (Thomas, 2001).
Prefrontal cortex
[edit | edit source]
The prefrontal cortex (PFC) is responsible for complex cognitive behaviour, decision making and consciousness (Burton, Westen, Kowalski, & Westen, 2015). While there is still much debate as to what specific role the different areas of the PFC play in anxiety related disorders, a review conducted by Spalding in 2018, investigated the role that the medial prefrontal cortex (mPFC) has in relation to fear generalisation - conditioned fear generalising to related stimuli, (Spalding, 2018). The study found that in human subjects, the ventral mPFC plays an important role in inhibiting the fear generalisation, while dorsal mPFC is seen to activate fear generalisation. Studies indicate that "higher levels of anxiety have been associated with increased activity in the dorsal mPFC (Straube et al., 2009), but further research needs to be done to investigate this.
Anterior cingulate cortex (ACC)
[edit | edit source]
The Anterior cingulate cortex (ACC) is not only responsible for autonomic functions such as heart rate and blood pressure, but also some higher brain functions such as cognition, decision-making and affect (Stevens, Hurley, & Taber, 2011) A meta-analysis of studies using neural imaging (fMRI), and cognitive Counting Stroop and Emotional Counting Stroop Tests included information relating to emotional processing in healthy volunteers and symptom provocation in volunteers with psychiatric disorders such as anxiety related disorders. The tests concluded that the separate areas of the ACC are involved in both emotion and cognition although further research into the question of the type of interaction between these emotional and cognitive processes is needed (Bush, Luu & Posner, 2000). Studies also show neuroimaging of the brain that links dysfunction of the ACC and psychiatric disorders such as bipolar disorder, schizophrenia, depression, obsessive-compulsive disorder, post-traumatic stress disorder and autism (Yücel et al., 2003). Further research should be conducted to investigate how this dysfunction can be identified earlier using neural imaging to help manage these disorders.
Pharmacological treatments for anxiety
[edit | edit source]There are currently two main classes of drugs that are used to treat the biological symptoms of anxiety, antidepressants and benzodiazepines. Antidepressants are a large class of medication with different types of antidepressants falling under this category.
Selective Serotonin Reuptake Inhibitors (SSRIs)
[edit | edit source]Selective serotonin reuptake inhibitor (SSRIs) are the most widely prescribed group of antidepressants throughout the United States and other countries (Preskorn, Ross, Stanga, 2004). SSRIs are considered first-line antidepressant drugs, which means they will generally be the first medication a doctor or psychiatrist will try prescribing for the treatment of anxiety (National Health Service, 2018). SSRIs are thought to work by increasing the levels of the neurotransmitter serotonin (5-HT) in the brain. It does this by inhibiting (blocking) reuptake, meaning more serotonin is available for the brain to carry signals between brain cells (National Health Service, 2017). Serotonin is linked to mood, emotion and sleep (Merens, Van der Does & Spinhoven 2007). The most commonly found SSRIs are fluoxetine, sertraline, fluvoxamine, paroxetine, citalopram and escitalopram. SSRIs are effective for both depressive and anxiety related disorders and the advantage of SSRIs is that they have good tolerability and do not cause some of the severe negative side effects seen in some other antidepressants (Preskorn, Ross, Stanga, 2004). Common for all antidepressants is that they are reported to produce some withdrawal effects if suddenly stopped. Withdrawal symptoms are reduced by gradually stopping the medication when the coming off it (The Australian National University, 2015).
Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs)
[edit | edit source]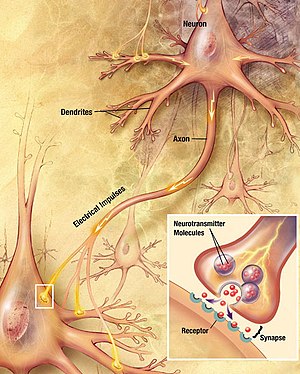
Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs) work by inhibiting the reuptake of serotonin (5-HT) as well as inhibiting the reuptake of noradrenaline (NA). Noradrenaline is a hormone and neurotransmitter responsible in the brain for increasing levels of arousal and alertness which is linked to fear and anxiety (Montoya, Bruins, Katzman, & Blier, 2016). SNRIs bind the serotonin transporters (5-HTT) and the noradrenaline transporters (NAT) like tricyclic antidepressants (TCAs) with the difference that SNRIs do not attract other receptors like TCAs do. It is shown that while SNRIs are ‘dual action’ between serotonin and noradrenaline, is also increases dopamine levels in the prefrontal cortex due to noradrenaline transporter inhibition (Komsuoglu, Mutlu, Ulak, 2012). In the brain, dopamine functions in motor control, arousal, reinforcement and reward and has been linked to controlling and regulating anxiety (Zarrindast & Khakpai, 2015). Common SNRIs include, desvenlafaxine, duloxetine, levomilnacipran and venlafaxine. Alongside SSRIs they are generally well tolerated and can be considered second-line antidepressant drugs (National Health Service, 2018), generally tried if SSRIs are not showing to be effective for the individual.
TriCyclic Antidepressants (TCAs)
[edit | edit source]Tricyclic antidepressants (TCAs) are among the earliest antidepressants developed and while they are still in use, they have also been replaced by newer medication such as SNRIs that causes fewer side effects. Like SNRIs, TCAs work by inhibiting the reuptake of serotonin (5-HT) and noradrenaline (NA) by binding to the serotonin transporters (5-HTT) and noradrenaline transporters (NAT) (Komsuoglu, Mutlu, Ulak, 2012). However, in the process of doing this, the TCAs affect other chemical receptors, leading to a number of unwanted side effects, some of which have the potential to cause harm to themselves or others. The more common of these include; blurred vision, drowsiness (care needed when driving), confusion, low blood-pressure and urine retention (The Australian National University, 2015). TCAs also are very dangerous with overdose, as very large doses can cause coma and stop the heart. Alcohol and other medications such as painkillers also increase the drowsiness effect of TCAs. It is for these reasons that TCAs are less commonly used now and are viewed as a third-line antidepressant drugs (National Health Service, 2018), less likely to be prescribed for anxiety unless nothing else is working. The most common TCAs are amitriptyline, imipramine, dothiepin, nortriptyline, trimipramine, clomipramine and doxepin.
Monoamine Oxidase Inhibitors (MAOIs)
[edit | edit source]Monoamine Oxidase Inhibitors (MAOIs) were the first type of antidepressant developed. MAOIs work by inhibiting the activity of monoamine oxidase. Monoamine oxidase is an enzyme found throughout the body and the brain that breaks down a number of chemicals, including three major neurotransmitters, serotonin, noradrenaline and dopamine. By inhibiting monoamine oxidase, MAOIs increase the amount of serotonin, noradrenaline and dopamine in the brain (The Australian National University, 2015). Despite clinical benefits, MAOIs have had a reduction in their usage due to the discovery of serious and potentially dangerous interactions between MAOIs and some medication (relating to the sympathetic nervous system), and some foods high in tyramine (such as some cheeses and fish). MAOIs have a number of common side effects such as drowsiness, tremors, dizziness, lowered blood pressure causing fainting and dangerously high blood pressure when combined with the aforementioned medications and foods. Due to these reasons, MAOIs are also viewed as third-line antidepressant drugs and will generally not be prescribed for anxiety unless safer and more common medication options aren’t working (National Health Service, 2018). The most common MAOIs are tranylcypromine and phenelzine.
Reversible Inhibitors of MonoAmine oxidase (RIMAs)
[edit | edit source]Reversible Inhibitors of MonoAmine oxidase (RIMAs) work similar to MAOIs, in that they reduce the activity of monoamine oxidase which breaks down noradrenaline, serotonin and dopamine, increasing the amount of these chemicals in the brain. Moclobemide is the only RIMA drug available and it is not approved in the United States, but is approved in the United Kingdom and Australia. The difference between Moclobemide and the other MAOIs is that studies have shown that no significant changes in ECG or rises in cardiovascular pressure occurring when Moclobemide is combined with tyramine and some other medication, indicating should be considered a safe and well tolerated antidepressant, especially in the elderly (Roth, Mountjoy & Amrein, 1996). More research should be conducted into its effectiveness in treating anxiety related disorders.
Benzodiazepines
[edit | edit source]Benzodiazepines belong to a class of central nervous system psychoactive depressants called minor tranquilisers used to treat anxiety disorders. Benzodiazepines can be prescribed by doctors in Australia but while under the influence of them, it is illegal to operate a car or heavy machinery. Due to the high risk of dependence with benzodiazepines, they are usually prescribed for short-term use only. An increasing problem with benzodiazepines is their illegal recreational use in either powdered, pill or injected form (NSW State Library, 2017). Benzodiazepines work by increasing the efficiency of gamma-Aminobutyric acid (GABBA) in the brain. GABBA is a neurotransmitter that inhibits cell activity in the brain, so inhibiting its activity through benzodiazepines has an overall “slowing down” effect, relieving anxious symptoms (The Australian National University, 2017). However, while this is the effect that the user perceives, benzodiazepines do not actually increase the supply and levels of the neurotransmitters serotonin, noradrenaline and dopamine that various other antidepressants do. The most common types of benzodiazepines are diazepam (long-acting), alprazolam (short-acting), oxazepam (short-acting), nitrazepam (immediate-acting), and temazepam (short-acting) (Alcohol & Drug Foundation, 2018). The main disadvantage to consider before taking benzodiazepines is their serious addictive nature, especially when used over long periods of time, cause dependence and severe withdrawal symptoms when the medication is stopped. These withdrawal symptoms can include, drowsiness, dry mouth, dizziness, constipation, headache, nausea and blurred vision, among others (The Australian National University, 2017).
Antidepressants or benzodiazepines for anxiety disorders?
[edit | edit source]While both antidepressant drugs and benzodiazepines are currently used to treat anxiety disorders, the question remains as to which treatment is the most effective. In 2013, a systematic review and meta-analysis performed by Offidani and colleagues addressed the question regarding the ‘Efficacy and Tolerability of Benzodiazepines versus Antidepressants in Anxiety Disorders’, (Offidani, Guidi, Tomba & Fava, 2013). Using data collected from 22 studies gathered from six databases that met the criteria to be included in the analysis the researchers discovered that 18/22 studies involved tricyclic antidepressants (TCAs) and involved various anxiety related disorders. The researchers then selected the 10 studies comparing TCAs and benzodiazepines (BDZs) used to treat individuals suffering from panic disorder and used them to complete a meta-analysis. The remaining studies were examined individually. The researchers had recognised a shift in the recent years leading up to their study in healthcare professionals prescribing antidepressants (ADs) rather than BDZs to treat anxiety related disorders, so the aim of their study was to analyse whether the comparison between ADs and BDZs supported this shift. What the researchers found was that there was no consistent advantage to using TCAs over BDZs in treating generalised anxiety disorder (GAD), complex phobias, and anxiety-depressive disorders. However, unsurprisingly, TCAs showed far fewer treatment withdrawals and negative events than the ADs. The researchers also found that in panic disorder, BDZs showed to be more effective than the ADs in the reducing the number of panic attacks. Interestingly, the BDZs also showed to be better tolerated and cause less discontinuation and side effects than the TCAs. The individual studies examined by the researchers that contained newer ADs showed that BDZs showed similar or greater improvement or adverse effects in patients suffering from GAD or panic disorder. The researchers concluded by questioning the shift in the prescribing pattern from BDZs to ADs to treat anxiety disorders, stating that it “has occurred without supporting evidence,” (Offidani, Guidi, Tomba & Fava, 2013).
Due to the addicting nature of benzodiazepines when used over long periods of time, it is worth considering the long-term treatment plans for patients suffering from anxiety disorders and creating pharmacological treatment plans accordingly. This research suggests that while some anxiety related disorders such as specific phobias or panic attacks may benefit from the use of short-term use benzodiazepines, other disorders such as generalised anxiety disorder or social anxiety disorder may benefit from more long plan treatment, where the addictive nature of benzodiazepines may cause serious harm. In that case, the use of the first-line antidepressants such as SSRIs may prove to be the most beneficial to the patient.
Therapeutic treatments for anxiety
[edit | edit source]It is worth noting that studies have shown that pharmacological treatment is most effective when used in conjunction with therapeutic treatment such as cognitive behavioural therapy (Van Apeldoorn et al., 2008). To learn more about CBT please follow these links:
- Mindfulness and anxiety (Book chapter, 2015)
- Key principles of CBT
- Efficacy of CBT
Conclusion
[edit | edit source]
See also
[edit | edit source]- Anxiety (Wikipedia)
- Neuroscience (Wikipedia)
- Antidepressant (Wikipedia)
- Benzodiazepine (Wikipedia)
- Benzodiazapine Addiction
References
[edit | edit source]American Psychiatric Association. (2013). Anxiety disorders. In Diagnostic and statistical manual of mental disorders: DSM-5 (5th ed.). Arlington, VA: Author.
American Psychological Association. (2018). Anxiety. Retrieved from https://www.apa.org/topics/anxiety/index.aspx
Australian Bureau of Statistics. (2008). National survey of mental health and wellbeing: Summary of results, 2007 (4326.0). Retrieved from ABS website: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/4326.02007?OpenDocument
The Australian National University. (2015, March 11). SSRI (Selective Serotonin Reuptake Inhibitor) antidepressants. Retrieved from https://bluepages.anu.edu.au/index.php?id=ssri-selective-serotonin-reuptake-inhibitor-antidepressants
The Australian National University. (2015, March 12). Tricyclic antidepressants (TCAs). Retrieved from https://bluepages.anu.edu.au/index.php?id=tricyclic-antidepressants-tcas
The Australian National University. (2015, March 11). Reversible monoamine oxidase inhibitor (RIMA). Retrieved from https://bluepages.anu.edu.au/index.php?id=reversible-monoamine-oxidase-inhibitor-rima-antidepressants
The Australian National University. (2017, February 1). Benzodiazepines/Tranquilisers. Retrieved from https://bluepages.anu.edu.au/index.php?id=tranquilisers
Brammer, M. (2009). The role of neuroimaging in diagnosis and personalized medicine-current position and likely future directions. Dialogues in clinical neuroscience, 11(4), 389-96.
Burton, L. J., Westen, D., Kowalski, R. M., & Westen, D. (2015). Psychology (4th ed.). Milton, Australia: Wiley.
Bush, G., Luu, P., & Posner, M. I. (2000). Cognitive and emotional influences in anterior cingulate cortex. Trends in Cognitive Sciences, 4(6), 215-222. doi:10.1016/s1364-6613(00)01483-2
Cohodes, E. M., & Gee, D. G. (2017). Developmental neurobiology of anxiety and related disorders. Oxford Research Encyclopedia of Neuroscience. doi:10.1093/acrefore/9780190264086.013.129
Davis, M., & Whalen, P. J. (2000). The amygdala: vigilance and emotion. Molecular Psychiatry, 6(1), 13-34. doi:10.1038/sj.mp.4000812
Delvin, H. (2016). What is functional magnetic resonance imaging (fMRI)? – Psych central. Retrieved October 27, 2018, from https://psychcentral.com/lib/what-is-functional-magnetic-resonance-imaging-fmri/
Etkin, A. (2012). Neurobiology of anxiety: From neural circuits to novel solutions? Depression and Anxiety, 29(5), 355-358. doi:10.1002/da.21957
Health Direct. (2018, April 10). Electroencephalogram. Retrieved from https://www.healthdirect.gov.au/electroencephalogram-eeg
Ionescu, D. F., Niciu, M. J., Mathews, D. C., Richards, E. M., & Zarate, C. A. (2013). Neurobiology of anxious depression: A review. Depression and Anxiety, 30(4), 374-385. doi:10.1002/da.22095
Iorfino, F., Hickie, I. B., Lee, R. S., Lagopoulos, J., & Hermens, D. F. (2016). The underlying neurobiology of key functional domains in young people with mood and anxiety disorders: a systematic review. BMC Psychiatry, 16(1). doi:10.1186/s12888-016-0852-3
Komsuoglu, I., Mutlu, O., & Ulak, G. (2012). Serotonin noradrenaline reuptake inhibitors (SNRIs). Effects of Antidepressants. doi:10.5772/37999
Livingstone, M. G., & Livingstone, H. M. (1996). Monoamine Oxidase Inhibitors. Drug Safety, 14(4), 219-227. Retrieved from https://link.springer.com/article/10.2165/00002018-199614040-00002
Martin, E. I., Ressler, K. J., Binder, E., & Nemeroff, C. B. (2010). The neurobiology of anxiety disorders: Brain imaging, genetics, and psychoneuroendocrinology. Clinics in Laboratory Medicine, 30(4), 865-891. doi:10.1016/j.cll.2010.07.006
McIntyre, R., & Goergen, S. (2017, July 26). Magnetic Resonance Imaging. Retrieved from https://www.insideradiology.com.au/mri/
Merens, W., Willem Van der Does, A., & Spinhoven, P. (2007). The effects of serotonin manipulations on emotional information processing and mood. Journal of Affective Disorders, 103(1-3), 43-62. doi:10.1016/j.jad.2007.01.032
Milham, M. P., & Banich, M. T. (2005). Anterior cingulate cortex: An fMRI analysis of conflict specificity and functional differentiation. Human Brain Mapping, 25(3), 328-335. doi:10.1002/hbm.20110
Montoya, A., Bruins, R., Katzman, M., & Blier, P. (2016). The noradrenergic paradox: implications in the management of depression and anxiety. Neuropsychiatric Disease and Treatment, 541. doi:10.2147/ndt.s91311
Nahtional Health Service. (2017, October 23). Selective serotonin reuptake inhibitors (SSRIs). Retrieved October 26, 2018, from https://www.nhs.uk/conditions/ssri-antidepressants/
National Health Service. (2018). Guidelines on choice and selection of antidepressants for the management of depression. Retrieved from http://www.hpft.nhs.uk/media/1584/guidelines-on-choice-and-selection-of-antidepressants-for-the-management-of-depression-final-oct-2016.pdf
NSW State Library. (2017, October 20). Benzodiazepines. Retrieved from https://druginfo.sl.nsw.gov.au/drugs-z-drugs/benzodiazepines
Offidani, E., Guidi, J., Tomba, E., & Fava, G. A. (2013). Efficacy and tolerability of benzodiazepines versus antidepressants in anxiety disorders: A systematic review and meta-analysis. Psychotherapy and Psychosomatics, 82(6), 355-362. doi:10.1159/000353198
Preskorn, S. H., Ross, R., & Stanga, C. Y. (2004). Selective serotonin reuptake inhibitors. Antidepressants: Past, Present and Future, 241-262. doi:10.1007/978-3-642-18500-7_9
Roth, M., Mountjoy, C. Q., & Amrein, R. (1996). Moclobemide in elderly patients with cognitive decline and depression: An international double-blind, placebo-controlled trial. British Journal of Psychiatry, 168(02), 149-157. doi:10.1192/bjp.168.2.149
Spalding, K. N. (2018). The role of the medial prefrontal cortex in the generalization of conditioned fear. Neuropsychology, 32(1), 1-17. doi:10.1037/neu0000384
Stevens, F. L., Hurley, R. A., & Taber, K. H. (2011). Anterior cingulate cortex: Unique role in cognition and emotion. Journal of Neuropsychiatry, 23(2), 121-125. doi:10.1176/appi.neuropsych.23.2.121
Straube, T., Schmidt, S., Weiss, T., Mentzel, H., & Miltner, W. H. (2009). Dynamic activation of the anterior cingulate cortex during anticipatory anxiety. NeuroImage, 44(3), 975-981. doi:10.1016/j.neuroimage.2008.10.022
Strawn, J. R., Dominick, K. C., Patino, L. R., Doyle, C. D., Picard, L. S., & Phan, K. L. (2014). Neurobiology of pediatric anxiety disorders. Current Behavioral Neuroscience Reports, 1(3), 154-160. doi:10.1007/s40473-014-0014-1
Thomas, K. M. (2001). Amygdala response to fearful faces in anxious and depressed children. Archives of General Psychiatry, 58(11), 1057-1063. doi:10.1001/archpsyc.58.11.1057
Tottenham, N., Hare, T. A., Quinn, B. T., McCarry, T. W., Nurse, M., Gilhooly, T., … Casey, B. (2010). Prolonged institutional rearing is associated with atypically large amygdala volume and difficulties in emotion regulation. Developmental Science, 13(1), 46-61. doi:10.1111/j.1467-7687.2009.00852.x
Van Apeldoorn, F. J., Van Hout, W. J., Mersch, P. P., Huisman, M. , Slaap, . B., Hale, W. W., Visser, S. , Van Dyck, R. and Den Boer, J. A. (2008), Is a combined therapy more effective than either CBT or SSRI alone? Results of a multicenter trial on panic disorder with or without agoraphobia. Acta Psychiatrica Scandinavica, 117: 260-270. doi:10.1111/j.1600-0447.2008.01157.x
Weiskrantz, L. (1956). Behavioral changes associated with ablation of the amygdaloid complex in monkeys. Journal of Comparative and Physiological Psychology, 49(4), 381-391. doi:10.1037/h0088009
Yücel, M., Fornito, A., Wood, S., Pantelis, C., Riffkin, J., & Velakoulis, D. (2003). Anterior cingulate dysfunction: Implications for psychiatric disorders? Journal of psychiatry & neuroscience, 28(5), 350-354.
Zarrindast, M. R., & Khakpai, F. (2015). The modulatory role of dopamine on anxiety behavior. Arch Iran Med, 18(9), 591-603. Retrieved from https://pdfs.semanticscholar.org/1191/e6ba1e43141a0efd41754b6c8bf49a589a62.pdf?_ga=2.102480833.1139804520.1540785623-747116929.1540456435
External links
[edit | edit source]- Beyond Blue (Support Service)
- CBT and Anxiety (Video)
- Neuroscience of anxiety (Video)
