Motivation and emotion/Book/2016/Sleep and motivation
What is effect of sleep on motivation?
Overview
[edit | edit source]|
Sleep, an essential biological process, serves to preserve and repair the body’s energy. However, when the human body fails to receive the required quantity and quality of sleep, biological and cognitive health aspects start to diminish. This book chapter will discuss the specific impact of sleep deprivation on motivation. |
What is sleep?
[edit | edit source]Sleep, according to Buysse (2014), is a cyclical state of detachment and unresponsiveness to the situational environment (Buysse, 2014). Characteristically, sleep in humans is conveyed through a resting position, motionlessness, and shut eyelids (Buysse, 2014).
Stages of sleep
[edit | edit source]Non Rapid Eye Movement (NREM), considered to be a lighter version of sleep; and Rapid Eye Movement (REM), outlined by it’s deeper form, are the two core categories that define sleep (Walker & van der Helm, 2009).

With the aid of an electroencephalogram (EEG), four sub-stages that encompass NREM can be measured and distinguished. Alpha (8-12 Hz) and Beta (13-30 Hz) activity are the two core patterns that occur when an individual is in a state of wakefulness. Thus, when Theta activity (3.5-7.5 Hz) presents itself in the brain, it is clear that NREM stage 1 has commenced, and the individual is shifting from being awake to falling asleep (Vassalli & Dijk, 2009).
Following the presentation of Theta activity in the brain, the addition of both sleep spindles and K complexes complete Stage 2 of NREM. Striking roughly every three minutes throughout all four stages of NREM, sleep spindles appear as short spurts of waves (12-14 Hz). K complexes, however, solely belong to the dimensions of NREM stage 2, and are described as impulsive short waveforms (Vassalli & Dijk, 2009).
Slow Wave Sleep (SWS) entails both stage three and four of NREM, and are based on the presence of high profusion waves that are slower than 3.5 Hz. These are known as delta activity. 20%-50% of delta activity is present in Stage three of NREM, with the rising of beyond 50% in stage four (Vassalli & Dijk, 2009).
According to Walker and van der Helm (2009), REM is a period of the deepest and intimate sleep. During REM, eye movement occurs at a back and forth pace, and active dreaming particularly is projected (Walker & van der Helm, 2009). Gamma activity, which occurs in conjunction with Theta activity, reaches a high 30-80 Hz (Vassalli & Dijk, 2009). A typical cycle combining the four stages of NREM and REM sleep resembles a 90-minute sleep pattern (See Figure 1) (Walker & van der Helm, 2009).
Test yourself
Optimal sleep
[edit | edit source]In order to preserve good health, sleeping seven to twelve hours per night – dependant on age and gender – and completing the full sleep cycle is essential (Burton, Westen, & Kowalski, 2012). According to Dahl (1999), there are two core components to sleep that one must consider. The first is that each individual needs a distinctive sleep requirement (Dahl, 1999). The second is that falling asleep and awakening states, on a physiological level, are attentively correlated facets of a larger scheme of arousal regulation (Dahl, 1999).
What is motivation?
[edit | edit source]According to Reeve (2015), motivation is defined as the influence that provides behaviour vitality and direction (Reeve, 2015). Furthermore, Ryan and Deci (2000), describe motivation as being ‘moved’ in any way, shape, thought, or form. An individual who lacks willingness to act is considered unmotivated, while in contrast, an individual who is empowered to meet a conclusion is considered motivated (Ryan, Deci, 2000). Individuals also vary in the quantity (level) and type (orientation) of motivation they maintain.
Sleep and motivation
[edit | edit source]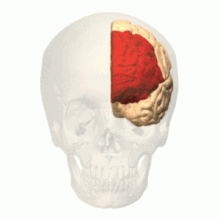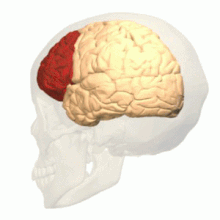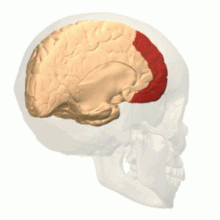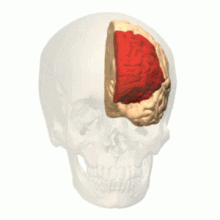
Sleep loss strongly affects the prefrontal cortex (See Figure 2), and points to deficiencies perceived in prefrontal cortex associated functions (Franzen, Siegle, & Buysse, 2008). In the brain, the prefrontal areas are crucially a part of regulating mood, predominantly by inhibiting brain structures such as the amygdala that are significant to the production and detection of affect (Franzen, Siegle, & Buysse, 2008). Hence, according to authors Franzen, Siegle and Buysse (2008), lack of sleep associated cognitive and affective deficiencies may share comparable pathophysiologic bases and could possibly be interconnected (Franzen, Siegle, & Buysse, 2008).
Additionally, sleep deprivation has been associated with cognitive and mood instability. Authors Franzen, Siegle and Buysse (2008) have suggested that chronic sleep constraint and acute sleep deficiency leads to larger cognitive and motor mood effects, and the lack of sleep related effects on mood are comparable to other mood disorders such as depression and anxiety (Franzen, Siegle, & Buysse, 2008).
Does sleep have an effect on motivation?
[edit | edit source]Like a connected sequence, sleep effects motivation, which directly correlates with emotion, which devises sleep behaviour – and thus the cycle begins again.
Yoo, Gujar, Hu, Jolesz and Walker (2007) completed a study that addressed the emotional affect of the brain without sleep. Using function Magnetic Resonance Imaging, a magnetic resonance imaging technique that processes blood flow in brain activity, the authors examined the variance between two groups (Yoo et al., 2007). The first group consisted of individuals who had endured a sleep-deprived night. The second group, slept. Results indicated that in the control group – the individuals who slept – a greater connection was present between the medial prefrontal cortex and the amygdala (Yoo et al., 2007). As the medial prefrontal cortex plays a vital part in memory, decision-making, and self-reward, participants in the control group were able to make more suitable decisions the day after their night's rest (Yoo et al., 2007).
Results also identified an amplified correlation between the amygdala and brainstem – the central stalk of the brain that conjoins to the spine – in the sleep-deprived group (Yoo et al., 2007). Authors suggest that this correction is a hyper consequence by the amygdala to negative emotional stimuli under circumstances of lack of sleep (Yoo et al., 2007). Conclusively, said data suggests that sleep retunes the accurate brain reactivity to next-day emotional challenges, thus implementing a more calm and tranquil view of events. These emotional components related to adequate sleep support the foundations of healthy thoughts.
Furthermore, in a study conducted by authors Mikulincer, Babkoff, Caspy and Sing (1989), the outcome of a total loss of seventy-two hours of sleep were examined on the psychological variables of sleepiness, affect, motivation, cognitive difficulties, and waking dreams (Mikulincer, Babkoff, Caspy, & Sing, 1989). Results indicated that sleepiness, affect, motivation, cognitive difficulties, and waking dreams are significantly affected by the extent of sleep deprivation, with the variables said to be getting worse as time prolonged (Mikulincer, Babkoff, Caspy, & Sing, 1989). Conclusively, it was specified that the profusion of the circadian component of the psychological figures increased over the extent of sleep loss and deprivation (Mikulincer, Babkoff, Caspy, & Sing, 1989).
In addition to the two examined studies, Franzen, Siegle and Buysse (2008) assessed the correlation between the consequences of sleep deprivation on subjective and objective measures of tiredness and affect, as well as psychomotor vigilance performance. In their study, individuals were unsystematically allocated to either a night of sleep, or night of sleep deprivation (Franzen, Siegle, & Buysse, 2008). The following day, statistics were measured by both subjective self-report and the objective Multiple Sleep Latency Test and the Pupil Sleepiness Test. Results indicated that sleep deprivation had a momentous impact on motivation, affect, sleepiness, vigilance, and executive function (Franzen, Siegle, & Buysse, 2008).
Sleep and motivation in children
[edit | edit source]A research study conducted by Meijer and van den Wittenboer (2004) examined the joint contribution of sleep, intelligence and motivation to daytime educational performance on 153 children with a mean age of eleven years and seven months.

The test used an organized equation model that measured the effect of sleep length and sleep quality on academic performance. Intelligence, attainment motivation, and examination anxiety were all used as control variables (Meijer & van den Wittenboer, 2004). Said variables were modeled more exclusively by the following two variables: ‘chronic sleep reduction’ and ‘eagerness.’ Chronic sleep reduction, based on the weight of sleep length, assessed: school day bedtime, weekend bedtime, and child authority to determine own bedtime. Eagerness, based on sleep quality, related to conscious and subconscious test anxiety (Meijer & van den Wittenboer, 2004).
The association between all stated variables indicated that less chronic sleep reduction, in combination with higher eagerness, achievement motivation, and intelligence all contribute to greater daytime educational performance (Meijer & van den Wittenboer, 2004).
Furthermore, Meijer (2008) conducted a study on prolonged sleep decline, school performance and academic motivational achievement in preadolescents. A survey titled: Chronic Sleep Reduction was established to investigate consequences of lack of sleep. For example, tiredness, sleepiness, loss of energy and motivation, as well as emotional instability (Meijer, 2008). Participants included 436 children with a mean age of eleven years and five months.
Conclusively, the author found that chronic sleep reduction affected school achievement directly. Results also indicated that lack of sleep indirectly affects functioning at school through motivation and emotion levels, with poorer academic marks as a result (Meijer, 2008).
Health and sleep deprivation
[edit | edit source]As research has suggested, sleep affects emotion and motivation. However, it is important to understand that sleep significantly affects health, which directly affects motivational levels. Thus, the suggested cycle and correlation between sleep, motivation and emotion, continues with the addition of health into play.
Research conducted through the International Classification of Sleep Disorders states that sleep deprivation caused over eighty diverse health disorders (Hossain & Shapiro, 2002). To gain further insight, authors Soderstrom, Jeding, Ekstedt, Perski, and Akerstedt (2012) studied threatening illnesses that were linked to sleep deficiency. Their research indicated that high blood pressure, disease of the heart, and diabetes were all lifelong medical conditions that arose, in part, from lack of sleep (Soderstrom at al., 2012). As well as this, the authors found that disorders such as obesity, mood disorders, and weak immune functioning, are all linked to sleep deprivation, and thus, a reduced life expectation (Soderstrom at al., 2012).
Furthermore, laboratory analyses suggest that lack of sleep increases the occurrence of either or both diabetes and obesity (Knutson, Spiegel, Penev, & Van Cauter, 2007). According to current data, changes in glucose metabolism, variation in appetite, and a reduction in energy disbursement are directed effects of the relationship between sleep deprivation, diabetes and obesity (Knutson, Spiegel, Penev, & Van Cauter, 2007).
Sleep deprivation also affects daytime performance. Motor dysfunction, fatigue, depression, lack of energy, impaired cognition, and irritability, as suggested by authors Mendelson, Garnett, Gillin, and Weingartner (1984), are shared consequences in sleep deficiency (Mendelson, Garnett, Gillin & Weingartner, 1984). Furthermore, daytime symptoms such as fatigue, irritability, decreased alertness and concentration have been reported by individuals suffering with insomnia (Riedel & Lichstein, 2000).
Obstructive sleep apnea
[edit | edit source]
Obstructive sleep apnea (OSA), as defined by Beebe and Gozal (2002), is disorder that is related with upper airway impediment during the sleep cycle (See Figure 4). Research evidence has suggested that major daytime cognitive and behavioral insufficiencies arise from OSA that go past simple sleepiness (Beebe & Gozal, 2002). A model created to assist the understanding of the psychological effects of individuals who suffer from OSA was created for the present study.
The model begins by highlighting that individuals with OSA experience a degree of sleep disruption and exhibit intermittent hypoxemia and hypercarbia (Beebe & Gozal, 2002). The natural restorative course that occurs during sleep is agitated, and in its place a range of cellular and biochemical tensions that lead to the disruption of functional homeostasis and changed neuronal and glial viability inside particular brain regions is stimulated (Beebe & Gozal, 2002). The dysfunction of prefrontal regions of the brain cortex, titled ‘executive dysfunction’ by neuropsychologists, is the prime indicator of the hostile cellular and biochemical proceedings activated by OSA (Beebe & Gozal, 2002). These include, as stated by Beebe and Gozal (2002), interactive reserve, set shifting, self instruction of affect and stimulation, functioning and contextual memory, as well as examination (Beebe & Gozal, 2002). Conclusively, the aftereffects of these result in daytime cognitive consequences such as a poor execution of plans, reduced judgment, rigid thinking, a lack in motivation and emotional immovability, as well as problems in mentally manipulating information (Beebe & Gozal, 2002).
Sleep disorders
[edit | edit source]There are many types of sleep disorders including insomnia which is the inability to sleep, restless legs syndrome which is the uncontrollable urge to move the legs constantly while sleeping due to leg discomfort and Bruxism which is the involuntary habitual grinding of the teeth typically during sleep (Mansfield, 2013).
Treatment for sleep disorders
[edit | edit source]Stepanski, Rybarczyk, Lopez, and Stevens (2003) examined several techniques and therapies for managing sleep difficulties. These comprise of the use of dopaminergic, hypnotic and tranquilizing medicine, as well as Cognitive Behaviour Therapy – which works to identify and substitute the actions and thoughts that are leading individuals to apprehension (Stepanski, Rybarczyk, Lopez & Stevens, 2003). As well as this, the authors recommend the use of nasal continuous positive airway pressure, which is a device that provides air to the lungs through the nose. Furthermore, restricting the quantity a person occupies in bed to the authentic time they spend sleeping, also known as Sleep Restriction Therapy, is another favorable method of insomnia treatment (Stepanski, Rybarczyk, Lopez & Stevens, 2003).
Sleep support
[edit | edit source]
Events in Australia
[edit | edit source]World Sleep Day
Funded by the World Association of Sleep Medicine, Australia celebrates World Sleep Day as a yearly occasion. World Sleep Day promotes knowledge and understanding of sleep loss and highlights the toll it takes on the lives of individuals ("World Sleep Day", 2016). In 2016, World Sleep Day occurred on Friday, March 18th, 2016
Sleep Awareness Week
Sleep Awareness Week, which was held from 4-10 July 2016 , raises awareness of common sleep disorders and the benefits of treatment ("Sleep Awareness Week", 2016). The week bases its foundation on the prior years sleep survey and uses that research to promote awareness.
Sleep tips
[edit | edit source]- A sleep pattern - Try sticking to a routine by waking up and going to sleep at the same time every day. Thus, your body will develop a healthy cycle.
- Food and drinks - Some foods, like caffeine and alcohol, contain stimulants that tend to keep us awake. It is best to try and avoid these for at least two hours before going to sleep.
- Relax - Lower the lights and remove all technology from your room to create a peaceful environment suitable for comfort.
A helping hand
[edit | edit source]
If you or someone you know is dealing with lack of sleep and it’s subsequent effects, there are a number of national helplines and websites you can reach out to. The following organizations offer information, advice, and a helping hand.
- Headspace - Self-contained telephone and online therapy services that are free of cost (See Figure 5). 1800 650 890 https://headspace.org.au
- SANE Australia - Reliable and relevant information about mental illness and disorders, as well as treatments and resources. 1800 18 7263 https://www.sane.org
- Furthermore, the national Sleep Health Foundation offers fact sheets, tool kits, and action plans to help understand and tackle sleep deprivation. http://www.sleephealthfoundation.org.au
Conclusion
[edit | edit source]Lack of sleep affects life quality and health. Consequences in health involve a undermined immunity, depression, diabetes, and stroke. Dahl (1996) summarizes the relationship between sleep and motivation in three points. Firstly, sleep and motivation signify adversary progressions in a superior system of stimulation regulation (Dahl, 1996). Secondly, involved contact among the controlling systems of sleep and motivation are integrated in sections of the prefrontal cortex (Dahl, 1996). And thirdly, the result of sleep deprivation is due to variations at the level of prefrontal cortex integration across regulatory systems . However, beyond this biological standpoint, the changes in these levels result in cognitive alterations in attention, emotions and motivation (Dahl, 1996).
See also
[edit | edit source]References
[edit | edit source]Burton, L., Westen, D., & Kowalski, R. (2012). Psychology (3rd Ed). Milton, QLD: John Wiley & Sons Australia Ltd.
Buysse, D. (2014). Sleep Health: Can We Define It? Does It Matter?. SLEEP. http://dx.doi.org/10.5665/sleep.3298
Dahl, R. (1996). The regulation of sleep and arousal: Development and psychopathology. Development And Psychopathology, 8(01), 3. http://dx.doi.org/10.1017/s0954579400006945
Dahl, R. (1999). The consequences of insufficient sleep for adolescents: Links between sleep and emotional regulation. Phi Delta Kappan, 80(5), 354-359.
Franzen, P., Siegle, G., & Buysse, D. (2008). Relationships between affect, vigilance, and sleepiness following sleep deprivation. Journal Of Sleep Research, 17(1), 34-41. http://dx.doi.org/10.1111/j.1365-2869.2008.00635.x
Hossain, J., & Shapiro, C. (2002). The prevalence, cost implications, and management of sleep disorders: an overview. Sleep And Breathing, 6(2), 85--102. doi:10.1007/s11325-002-0085-1
Knutson, K., Spiegel, K., Penev, P., & Van Cauter, E. (2007). The metabolic consequences of sleep deprivation. Sleep Medicine Reviews, 11(3), 163-178. http://dx.doi.org/10.1016/j.smrv.2007.01.002
Meijer, A. (2008). Chronic sleep reduction, functioning at school and school achievement in preadolescents. Journal Of Sleep Research, 17(4), 395-405. http://dx.doi.org/10.1111/j.1365-2869.2008.00677.x
Meijer, A. & van den Wittenboer, G. (2004). The joint contribution of sleep, intelligence and motivation to school performance. Personality And Individual Differences, 37(1), 95-106. http://dx.doi.org/10.1016/j.paid.2003.08.002
Mendelson, W., Garnett, D., Gillin, J., & Weingartner, H. (1984). The experience of insomnia and daytime and nightime functioning. Psychiatry Research, 12(3), 235--250. doi:DOI: 10.1016/0165-1781(84)90029-5
Mikulincer, M., Babkoff, H., Caspy, T., & Sing, H. (1989). The effects of 72 hours of sleep loss on psychological variables. British Journal Of Psychology, 80(2), 145-162. http://dx.doi.org/10.1111/j.2044-8295.1989.tb02309.x
Reeve, J. (2015). Understanding motivation and emotion. New York: Wiley.
Riedel, B., & Lichstein, K. (2000). Insomnia and daytime functioning. Sleep Medicine Reviews, 4(3), 277--298. doi:DOI: 10.1053/smrv.1999.0074
Ryan, R. M., & Deci, E. L. (2000). Intrinsic and extrinsic motivations: Classic definitions and new directions. Contemporary Educational Psychology, 25(1), 54-67. doi:10.1006/ceps.1999.1020
Sleep Awareness Week. (2016). Sleephealthfoundation.org.au. Retrieved 21 October 2016, from http://www.sleephealthfoundation.org.au/public-information/key-events/about-sleep-awareness-week.html
Soderstrom, M., Jeding, K., Ekstedt, M., Perski, A., & Akerstedt, T. (2012). Insufficient sleep predicts clinical burnout. Journal Of Occupational Health Psychology, 17(2), 175. doi: 10.1037/a0027518
Stepanski, E., Rybarczyk, B., Lopez, M., & Stevens, S. (2003). Assessment and treatment of sleep disorders in older adults: A review for rehabilitation psychologists. Rehabilitation Psychology, 48(1), 23. doi:0.1037/0090-5550.48.1.23
Vassalli, A. & Dijk, D. (2009). Sleep function: current questions and new approaches. European Journal Of Neuroscience, 29(9), 1830-1841. http://dx.doi.org/10.1111/j.1460-9568.2009.06767.x
Walker, M. & van der Helm, E. (2009). Overnight therapy? The role of sleep in emotional brain processing. Psychological Bulletin, 135(5), 731-748. http://dx.doi.org/10.1037/a0016570
World Sleep Day. (2016). Sleephealthfoundation.org.au. Retrieved 21 October 2016, from http://www.sleephealthfoundation.org.au/public-information/key-events/world-sleep-day.html
Yoo, S. S., Gujar, N., Hu, P., Jolesz, F. A., & Walker, M. P. (2007). The human emotional brain without sleep—A prefrontal amygdala disconnect. Current Biology, 17, R877–R878. Retrieved from: http://walkerlab.berkeley.edu/reprints/Yoo-Walker_CurrBiol_2007.pdf
External links
[edit | edit source]- Resources needing clarification
- Resources needing facts checked
- Resources needing examples
- Resources needing clarification by what
- Resources needing clarification by where
- Motivation and emotion/Book/2016
- Motivation and emotion/Book/Motivation
- Motivation and emotion/Book/Neuroscience
- Motivation and emotion/Book/Sleep
