Motivation and emotion/Book/2014/Obesity treatment and needs
How do different health advice sectors treat obesity and how do these treatments interact with our needs?

Overview
[edit | edit source]Introduction: Obesity, treatments and motivation
[edit | edit source]
Obesity has overtaken smoking as the biggest threat to public health in Australia, with around 14 million Australians classified as obese or overweight. If the current trajectory continues, by 2025, close to 80% of all Australian adults will be overweight or obese (Modi, 2013). So what have we been doing about it? Currently obesity treatments can include medications with a composition similar to methamphetamine, controlled energy input and expenditure, surgery to reduce the size of the stomach, and behavioural therapy (Reeve, 2009). However, there has been a lack of success in decreasing obesity (National Preventative Health Taskforce, 2008) while this is due to many factors in this book chapter we will be looking through the lens of social, psychological and physical needs at some treatments for obesity from different types of organisations in our health sector. The Australian government's “How do you measure up?” Campaign. The for profit weight loss program by Michelle bridges. The non-profit organisation, Obesity Australia, and lastly the care given by health care professionals like Doctors, and nurses.
Why are we talking about obesity and not weight loss? Isn't weight loss the treatment for obesity? The answer is no. Obesity is a medical condition which has many factors leading to its causation, some of which are not purely physical (Astrup et al. 2004). While the “treatments” we may analyse focus on weight loss and healthy eating, this will be critical to assess where they may fall down or lack support for cognitive factors.

We may have some ideas or preconceptions of what an obese person may look like, but what does it mean to be obese and how do we measure it? The body mass index (BMI) is a current standardised measure of the spectrum of body mass used by health professionals (National Preventative Health Taskforce, 2008). However, it has some limitations, and more recently in popular culture has become unfavourableTemplate:Why?. This type of measure may surprise people with a label of being obese when they feel they lead healthy lives and like their appearance. This issue may have more to do with negative perceptions in society about person's with obesity rather than the scientific criticisms of the measure.
Another way to measure the obesity is to simply measure around the waist. Why? Through research we can see the morbidity of diseases associated with extra body mass goes up with every centimetre of waistline, a waistline over 90cm for men and 80 cm for women would increase the risk of obesity related disease (Janssen, et al. 2002).
Mental illness, obesity and cancer have a close relationship, it may be interesting to highlight that probably it is not being depressed about being obese that makes people depressed, but a shared set of risk factors for the conditions, for example structural and social determinants, from fast food advertising to child abuse (Dickerson, 2006).So we can see how our environment and our genetics have such a great influence on our behaviour, so when it comes to the treatment of obesity are we so concerned with the one physical aspect, weight loss? We are taught to think the main cause of obesity is an imbalance of energy intake and expenditure, but so far controlling these two factors has not led to a decrease in obesity in our population. So what could be the problem? One possible issue is that currently obesity is a seriously oversimplified condition, and probably a far more environmental and psychological one that we may think (McElroy, 2004).

So why are we talking about obesity and motivation? The theory of social, psychological and physical needs can give a useful scaffold into understanding human behaviour. We will use this scaffold to understand how motivational techniques may play a role in helping or hindering our efforts against obesity. It may be most useful for our purposes to look more specifically at how the treatments facilitate or conflict with our psychological, physiological and social needs.
What is a need?
[edit | edit source]Why is it useful to do things that support our needs?
A need is used to describe a condition that is essential for life, growth and well-being (Reeve, 2009). According to Clark Hull (1945) our needs will give rise to a drive, and a drive motivates and energises our behaviour, so that we may satiate our need. It may be obvious why we need to satisfy our hunger need, but what happens when we can’t or don’t satisfy our social or psychological needs? Some obesity treatments may affect our needs in unprecedented ways, making the treatment unsuccessful. Hunger is a physiological process over which is it hard to gain conscious control over (Reeve, 2009), for the sake of weight loss we may try to do some voluntary actions like self-regulation over our eating, mindfulness about our environment and being motivated to exercise. However these methods if done in such a way that is not conforming to other motivational theories, like flow and goal setting, then they may be quite ineffective, and cause people to use restraint release as they may have underestimated the biological urge, have conflicting / inappropriate or inconsistent standards, possibly not monitoring their behaviour, and becoming overwhelmed or distracted which can be detrimental to the weight loss efforts. So, in terms of “supporting” our hunger need, it is important to have small, attainable goals, which we can monitor.
The benefits of autonomy are many, as well as helping us fulfil the other psychological needs, specific benefits to an obesity treatment would increase, persistence, engagement, task performance, psychological well-being, vitality and positive emotions. To make engaging in competence beneficial means to find that optimal challenge and flow. Competence support would be specifically useful in exercise motivation and cognitively regulated eating, we can facilitate this by providing positive feedback and perception of progress, as well as a tolerance of failure(Reeve, 2009). The need for relatedness describes a need to social interaction difference from a need for intimacy it also considers the benefits of living in a society with a internalised set of values, it is important for this part of needs motivation to be used positively for example, convincing society that we should proscribe to a healthy lifestyle, but not saying that we should discriminate against those who don’t already (Choices, 2014).
Social need for achievement also specifically more beneficial if used with certain techniques to facilitate it. For example, use of a mastery goal over a performance goal would not only benefits a wide range of goals, but would also help facilitate successful obesity treatment, and avoid maladaptive coping behaviours in the face of failure. Different from relatedness, Affiliation and intimacy, are a social need driven from a deprivation in warm, close relationships, in an obesity treatment setting, it would be important to break down barriers from discrimination that might prevent these relationships, while also minimising rejection anxiety. If a participant is high in the need for power they may find it easier to engage (Reeve, 2009). If we can support our needs, we can increase our behavioural engagement, our emotional engagement, our cognitive engagement and voice.
In order to get a deeper insight into the role of needs and motivation in obesity treatment we will now look at where and what treatments are accessible for a member of the public. So where can we find health advice and treatment? Well it can come from a variety of sectors, Firstly we will look at an in depth case study of the governments “How do you measure up?” campaign. Health care sectors
Government : "How do you measure up ?" campaign
[edit | edit source]The Australian government has an ethical responsibility to consider the welfare of its peoples. The government recognises the economic burden of obesity and the growing number of obese persons in Australia (National Preventative Health Taskforce, 2008).
To combat these trends the government has initiated several health campaigns that use media to attempt to increase awareness about obesity and how it increases incidence of other diseases. The “How do you measure up” campaign aims to;
- Increase awareness of the link between chronic disease and poor nutrition, physical inactivity and unhealthy weight.
- To raise appreciation of why lifestyle change should be an urgent priority;
- To generate more positive attitudes towards achieving recommended changes in healthy eating, physical activity and healthy weight; and
- To generate confidence in achieving the desired changes and appreciation of the significant benefits of achieving these changes. (“How do you measure up?”, 2010)
The program aims to complete these goals by having the public measure themselves around the waist, calculate their BMI, and consider how they and what they eat and how much they exercise, and do all of these things measure up to what the government states is a healthy person. This program gives board guidelines on healthy living and targets them at Australian adults; there is also 2 quizzes where people can test their knowledge about healthy living. If someone is deemed unhealthy by the guidelines given they recommend conforming to the following;
- A waistline under 80cm for women and 90cm for men.
- A BMI between 18.5 to 24.9.
- Drink plenty of water.
- Two servings of fruit and five servings of vegetables every day.
- Manage portion sizes.
- Eat less processed food. Restrict alcohol intake and limit intake of “extra “foods.
- At least 30 minutes of moderate-intensity physical activity on most, preferably all, days(“Eat for Health”, 2014).
This program aims to treat obesity though a board educational approach that stirs personal responsibility, how does this affect our needs?
Autonomy
[edit | edit source]This program in comparison to some other obesity treatments does not have an overly controlling style, it may seem that this campaign is doing okay so far. However we might say that is program doesn’t use an autonomy supportive motivational style, Reeve (2009) states to support autonomy we may try nurturing inner motivational resources, relying on flexible language, providing explanatory rationales, acknowledging and accepting the others expressions of negative affect. The program may use flexible language to reach a wide audience, but does not provide enough support services or information to facilitate the other factors.

Competence
[edit | edit source]Supporting competence is connected to providing feedback which should come from one or more of the following sources. The task itself; participants can use measures like the BMI or waist measurement to see their progress. Comparisons to past performance; only if a participant keeps a record of their progress will they have something to compare to, the program does provide a link to a meal planner which participants could use. Comparisons to the performance of others; the campaign doesn’t allow for interaction with other participants, and so unfortunately people may compare themselves to any sort of other person which may support incorrect or negative feedback.
Relatedness
[edit | edit source]This campaign relies heavily on the premise that by presenting the benefits of a healthy lifestyle that it will facilitate a social change or framework to promote internalisation of the healthy lifestyle because it will stir a persons need for relatedness to their society. The campaign may provide rationale that supports conforming to the healthy lifestyle is beneficial but it cannot account for the adversity an obese person may encounter that will create barriers to participating in communal relationships in order to provide that relatedness satisfaction. While we need to create a social and cultural change that supports healthy lifestyles, we also need to allow people that don’t yet conform to these values and regulations to be able to be accepted and connected to society.
Achievement
[edit | edit source]This campaign talks about how we need to achieve healthy eating, physical activity and healthy weight. The campaign aims to create dissonance between the present state of Australians and what they deem to be a healthy state; they do this through the education of the benefits of achieving a healthy lifestyle, hoping that this dissonance will energise the behaviour to accomplish a healthier lifestyle. The campaign in comparison with other treatments gives relatively vague structures in order to accomplish this; it may support a mastery goal type, which is more beneficial than in this circumstance than a performance goal (Reeve, 2009). However there is no system to tailor the vague structures into optimal goals for the individual, and so it may allow for an increase in failure avoidance, if the participant feels the goals are already an extreme change from their normal lifestyle.
Affiliation/intimacy
[edit | edit source]Like the psychological need for relatedness we might consider how this campaign may affect the capacity for participants to affiliate and create warm personal relationships. This program tires to insight a personal responsibility in the participant rather than giving strict controls, this program by trying to make a healthy lifestyle socially normal, may move obese persons in a society where they may have felt normal/accepted into a position where they feel rejection by society therefore increasing a deprivation in the affiliation/intimacy need (McClelland, 1985). How the program doesn’t provide any support to deal with feelings of rejection or loneliness, and obese person may seek the support of other obese persons in order to satiate this need rather than change to conform (Stürmer, et al. 2003). In order to really use affiliation and intimacy to benefit participants it would be better to assess how the participant may respond to a social need deprivation to correctly mitigate and counsel feelings of rejection and facilitate a healthy need to belong. (Reeve, 2009).
Power
[edit | edit source]This program allows participants to have a larger degree of control in comparison to some obesity treatments, however it does not account for the differences in the need for power and control in individuals, and therefore may not support those who may have a low need for power to engage them in the pursuit of the goal to treat their obesity.
Hunger
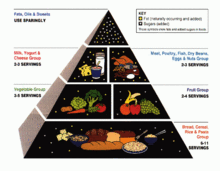
[edit | edit source]We know that cognitively regulated eating has not been a successful method(National Preventative Health Taskforce, 2008). This program does provide links to information about how to eat to the good pyramid system (“Eat for health”, 2014) which doesn’t notsuggest calorie control, but moderation of food types and amount. However does this method still set up Australians for self-regulation failure? If we are required to control our portion sizes according to the food pyramid then this may be a drastic change from the usual amount a person may be eating, then this may lead to a strong biological urge to eat more. There is no function of the eating plan that also the adaption of the eating standards to a persons before state, which may give rise to inappropriate standards(Reeve, 2009). It does offer a meal planner/recorder template however this is very hard to find, but may help people monitor their behaviour.
Conclusion
[edit | edit source]Being “healthy” is subjective and sometimes hard to define concept. A criticism of this campaign could be that, besides a waistline recommendation, there are not well defined concepts of good health instead they take on the approach that good health is the absence of chronic disease. It also does not
For profit : Michelle Bridges 12 week body transformation program
[edit | edit source]
The Michelle bridges 12 week Body transformation MOVE program, is an online resource that provides, energy input and expenditure guidelines, thought the means of meal plans, and exercise routines. It also has informational video and online forums which aim to build a community and provide support. This particular program has been developed for people with a BMI of 30+(“Move program”, 2014)
Autonomy
[edit | edit source]This program has little support for autonomy, and aims to targets a prescribed outcome, there are weekly instructional videos on how to shop, eat, exercise and even think! With videos aimed at changing mindsets surrounding weight loss and lifestyle. This program doesn’t aim to nurture inner motivational resources, but does provide a strong, well explained structure using easy to understand language and does provide education and rationale of the program. However it does not provide room acknowledging and accepting the others expressions of negative affect, instead chooses to focus on short term performance.
Competence
[edit | edit source]The feedback for this program can come from online forums from persons hired as moderators or though live chat sessions. It is unclear whether or not they use positive feedback. Another form of feedback is received though the weighing and measuring of the body, this type of feedback facilitates a performance orientated goal, which may not be as useful in the long term as a mastery type goal. While this website has many different programs it also may not be able to provide optimal challenge as it isn’t personalised, it also may not be able to provide any failure tolerance, as this may be dependent on the forum community or moderators. However the website and program does have a clear and helpful structure.


Relatedness
[edit | edit source]This program aims to provide the means to participants of engaging in a new way of life, by taking on Michelle bridges teaching and making it their own though internalisation (Reeve, 2009). On this premise they would hope that the program may continue long term. More research needs to be conducted in this area, the internalisation of values of the person teaching or conducting and the long term success.
Achievement
[edit | edit source]This program uses performance based goal setting for the 12 weeks, it also allows for some comparison if the participants choose to share the information on the forums. However the system is self-reported and it may be harder to ascertain whether or not people are reporting their real progress (Rowland, 1990).
Affiliation/intimacy
[edit | edit source]This program aims to provide an online community in which people may be able to make connections and develop relationships with others. Moderators monitor the forums and would remove any heinous remarks, but it is unclear whether or not people may suffer discrimination in the online forum or not.
Power
[edit | edit source]This program may help or hinder those with high power needs, taking away some of the control that otherwise would have come intrinsically may be detrimental, while they may flourish by providing support to their peers though the forums. Through having an impact (Reeve, 2009)
Hunger
[edit | edit source]This program uses calorie restriction to reduce energy intake, this program has a slightly higher calorie intake than other programs, in order to help slow weight loss. However research has shown that whether fast or slow, the rate at which weight is put back on is the same in the long term (Jeffery, et al. 2000).
Conclusion
[edit | edit source]In conclusion, this program has reported success, however it does not last for the long term. Could it be that an overly controlling method is not the way ?
Other Sectors
[edit | edit source]Non profit
[edit | edit source]Obesity Australia is a not for profit organisation that aims to help treat obesity and minimise the impact of obesity on Australian society by;
- Providing leadership and independent advice to inform sound policy
- Building recognition of the personal, social and economic effects of obesity
- Changing entrenched attitudes
- Independently evaluating what works and what doesn't work in the Australian context
- Showcasing the best science on how and why obesity occurs so it provides a base for effective community response and government funding ("Obesity Australia, 2014)
This is an interesting organisation that should be used to supplement the education on obesity.
Health care professionals
[edit | edit source]Health care professionals have played a role in monitoring and assessing obesity however, there is nationally enforced treatment plan that general practitioners may follow. The most current document in Australia that is developing more of a national plan, is the " Australia :Healthiest country by 2020". However, it still does not really recommend psychological intervention unless an eating disorder is prevalent.
Conclusion
[edit | edit source]
Research suggests we currently have not developed a treatment for obesity that works in the long term. It also may be possible that weight loss may not reverse the detrimental effects of obesity (National Preventative Health Taskforce, 2008).
Based on a motivational analysis from the needs point of view in order to create an effective treatment for obesity, it would be crucial to define obesity as a disease, and a disease that needs a highly personalized treatment plan and steady stream of feedback from both psychological and medical professionals. However, it should also be recognised that Australians are not simply “stupid people making poor choices” and that our environment influences our way of life, for example, the way our cities are built, the way in which for profit companies market food to us, and the placement of fast food establishments (Obesity Australia, 2014). It may be relevant to add that to beat obesity we may need to withdraw from the society in which we live in order to adapt a healthier lifestyle, for example using farmers markets instead of a supermarket or having a part time job instead of a full time job in order to devote more time to the self. Of course these aren’t options for everyone, and so we still need to provide support for obese persons as they may be segregated from and discriminated against in society (Choices, 2014).
See also
[edit | edit source]- Weight loss motivation in overweight children
- Veganism motivation
- Resisting the temptation of unhealthy food
- Comfort eating and negative emotions
- Chocolate and mood
- Dehydration and mood
- Exercise and mood
References
[edit | edit source]Choices, N. H. S. (2014). Weight discrimination study fuels debate-Health News-NHS Choices.
Dickerson, F. B. (2006). Obesity among individuals with serious mental illness. Acta Psychiatrica Scandinavica, 113(4), 306-313.
"How do you measure up?" (2010, October 8). Retrieved October 20, 2014, from http://webarchive.nla.gov.au/gov/20110601173703/http://www.measureup.gov.au/ internet/abhi/publishing.nsf/Content/copyright
Janssen, I., Katzmarzyk, P. T., & Ross, R. (2002). Body mass index, waist circumference, and health risk: evidence in support of current National Institutes of Health guidelines. Archives of internal medicine, 162(18), 2074-2079.
Jeffery, R. W., Epstein, L. H., Wilson, G. T., Drewnowski, A., Stunkard, A. J., & Wing, R. R. (2000). Long-term maintenance of weight loss: current status.Health psychology, 19(1S), 5. McClelland, D. C. (1985). How motives, skills, and values determine what people do. American Psychologist, 40(7), 812.
McElroy, S. L., Kotwal, R., Malhotra, S., Nelson, E. B., Keck, P. E., & Nemeroff, C. B. (2004). Are mood disorders and obesity related? A review for the mental health professional. J Clin Psychiatry, 65(5), 634-651.
Modi : Monash Obesity and Diabetes Insitute. (2013, August 6). Retrieved October 20, 2014, from http://www.modi.monash.edu.au/
“Move Program”(2014) Retrieved October 20, 2014 from https://www.12wbt.com/fitness/weight-loss
National Preventative Health Taskforce, Australia: the healthiest country by 2020. 2008, Preventative Health Taskforce: Commonwealth of Australia: Canberra. Available from: http://www.preventativehealth.org.au/internet/preventativehealth/publishing.nsf/Content/discussion-healthiest].
“Obesity Australia : Understanding Action” (2014) retrieved October 20, 2014 from http://www.obesityaustralia.org/
Reeve, J. (2009). Understanding motivation and emotion (5th ed.). Hoboken, NJ.
Rowland, M. L. (1990). Self-reported weight and height. The American journal of clinical nutrition, 52(6), 1125-1133.
Stürmer, S., Simon, B., Loewy, M., & Jörger, H. (2003). The dual-pathway model of social movement participation: The case of the fat acceptance movement. Social Psychology Quarterly, 71-82.
