Upper Limb Orthotics/Ulnar Nerve Lesion
Orthotic Management of an Ulnar Nerve Lesion
[edit | edit source]The patient is a 64-year-old male who suffered an ulnar nerve lesion stemming from a fracture to the olecron process in the elbow 2 months ago. He works as a carpenter where he fell off his ladder at work causing the fracture in the elbow. The injury to the olecron process has caused a high ulnar nerve lesion. This has caused clawing of the fourth and fifth digits and hyperextension of the metacarpophalangeal joint (MPJ). The patient has an inability to open his hand to grasp large objects and to abduct and adduct the fifth digit. The patient’s goals are to minimise the deformity thus allowing him to return to work.
Written information
[edit | edit source]Evidence
[edit | edit source]The ulnar nerve lesion is categorised as a high-level nerve lesion. They are more commonly caused from trauma to the elbow. High-level lesions are those lesions positioned proximal to the innervation of flexor carpi ulranis and flexor digitorum profundas (Pfaeffle, Waitayawinyu and Trumble, 2007, p.294).
High ulnar nerve lesions affect the function of the muscles it innervates. Colditz (1995), Scheker, Cheshar, Netscher, Julliard and O’Neill (1995) Paksima and Besh (2012) report that the ulnar nerve innervates the intrinsic muscles of the hand. The dorsal and volar interrosei muscles, which abduct and adduct the fourth and fifth digits at the MCPJ, are compromised. The hypothenar muscles in the hand such as abductor digiti minimi; flexor digiti minimi and opponens digiti minimi are all impaired. The movements of the hypothenar muscles create are abduction, flexion and lateral movement of the fifth digit. The loss of abduction, flexion and lateral movement therefore makes gripping objects difficult. Additionally, the lumbricals of the ring and little finger have an impaired function. The lumbricals flex the MCPJ and extend the philanges. Therefore, the combination of dorsal and volar interrosia, hypothenar muscles and the lumbricals being impaired means the intrinsic muscles of the hand that provide fine motor control movements are greatly compromised. The loss of intrinsic muscles in the hand, which assist in flexion of the MCPJ and extension of the interphalangeal joints (IPJ) are nonexistent. The absence of the intrinsic muscles means the extrinsic muscles are the only muscle opposing the tension of the long flexors. The extensors originate from the forearm and attach to the interossues and lumbricals to create the exstensor hood. The function of the extensors is to straighten out the digits (p.625 and p.86). The loss of the intrinsic muscles in the hand mean that the extrinsic muscles will dominate, as the balancing in the ring fingers is lost. This imbalance is known as intrinsic minus hand. This will create hyperextension of the MCPJ producing a claw position. Once in the claw position the only way the patient can flex the MCPJ is by fully flexing the IPJ (Scheker, Cheshar, Netscher, Julliard and O'Neill, 1995, p.590).
Damage to the ulnar nerve is more common at the elbow. The anatomical course of the ulnar nerve, especially at the elbow, significantly increases its vulnerability to irritations and lesions. The ulnar nerve originates from C8 and T1 roots and passes under the medial epicondyle through to the brachial plexus connecting onto the flexor carpi ulranis heads. It then proceeds underneath the aponeurosis between the ulnar and humeral heads. When the elbow performs movements such as flexion it changes shape from round to elliptical and the extaneural pressure increases by 45% (Shin and Ring, 2007, p.1110). The ulnar nerve can stretch, compress and slide. However, if these abilities are compromised an irritation can take place resulting in perinearal scarring (Seror, 1993, p.324).
Orthotic Treatment Requirements
[edit | edit source]Splinting claw hand involves opposing the claw hand deformity. Duncan (1989) and Parry, Harp, Fletcher, Dean, Knight and Robinson (1970) explain that the absence of the intrinsic muscles opposing the extrinsic muscles causes hyperextension of the MPJ. Therefore, a force is required to act on the MPJ to correct the claw deformity. The MPJ hyperextension block positions the splint in an intrinsic plus position. The hyperextension block therefore limits range of motion (ROM) in the MPJ so it does not exceed 0 degrees extention. At the same time it is important to allow flexion at the IPJ as the intrinsic muscles that are operating still need to be able to flex. Maximum flexion ROM is allowed. Free flexion means the splint is more functional for the patient (p.1108, p.33).
Colditz (1995) outlines that factors important in splinting in ulnar nerve palsy hand are to reduce the surface area of the splint to increase the functionality of the splint. Additionally, reducing surface area of the splint is important when the median nerve remains unaffected, as the sensibility is still high due to the active median nerve. In most cases this means the splint should only cover one-third of the palmer surface. Paternostro-Sluga, Keilani, Posch & Fialka-Moser (2003) imply that the function and fitting of the correct splint are important, as this correlates with the patient wearing the splint for longer, meaning a more successful treatment (p.87). Furthermore, rolling out the splint edges can reduce pressure from the splint. Also, where there are bony prominences, such as the MPJ, it is recommended to place padding, to prevent any pressure areas (Foss-Campbell, 1998, p.202).
Comparison of Treatment Options
[edit | edit source]Treatment of ulnar nerve lesions varies. DeSouza and Choi (2012) and Robertson and Saratsiotis (2005) report that conservative treatment involves an ulnar nerve palsy static splint or a dynamic dorsal knuckle bender splint in combination with physiotherapy. The other more invasive option is surgery. This can be used to release the tension on the nerve to allow healing (DeSouza and Choi, 2012; Saratsiotis, 2005).
Static Orthoses Treatment
[edit | edit source]Static splints are designed to limit movement and to support the joint. Duncan (1989) and Hong, Long, Kanakamedala, Chang and Yates (1996) outline that static splints maintain correct alignment and minimises deformities. A passive ROM can be achieved non-surgically by using a static splint. It can manipulate one joint to assist in the function of another joint, as shown by incorporating a hyperextension block to assist in flexion of the fourth and fifth digits (p.1107). An example of a static splint is an ulnar nerve palsy splint. Colditz (1995) and Scheker et al. (1995) explain that the splint limits the MPJ from hyperextending. This is achieved by positioning a force acting on the dorsum of the proximal phalanx. The dorsum block is molded, so that it equalizes pressure over the dorsum of the phalanx. Distally, the dorsum stop should end at the axis of the IPJ. The splint limits any intrinsic-minus deformity by allowing any unaffected intrinsic muscles to contract and any impaired intrinsic muscles to be maintained in flexion. Therefore, functional flexion is allowed. The impaired intrinsic muscles may have limited function, however, they still play a role in the balancing effect of the flexor and extensor mechanisms (p.625) and (p. 589).
Dynamic Orthoses Treatment
[edit | edit source]Dynamic splinting aims are to provide a passive ROM. Dynamic splints increase stretching of stiff joints. A dynamic splint used to manage ulnar nerve palsy is the dorsal knuckle bender splint (Duncan, 1989; Hong et al., 1996). The splint provides dynamic MPJ flexion. The splint provides resistance against the MPJ hyperextension by placing rubber band acting against that movement. It has a padded component over the dorsum of the metacarpal shafts and proximal phalanges. The objective is to insert pressure to the palm of the hand, proximal to the MP joint (Dell and Sforzo, 2005).
Surgical Treatment
[edit | edit source]A more invasive treatment option for ulnar nerve lesion is to surgically release the tension on the nerve. The aim of surgical intervention is to reduce the tension for repair. Generally for high-level lesions subcutaneous transposition is performed to lower the tension. The laceration is increased longitudinally and the ligament of Osborne and the flexor carpi ulranis heads are released (Pfaeffle, Waitayawinyu and Trumble, 2007).
Evaluation of Treatment Options
[edit | edit source]The difference between a static and dynamic splint is how the splint blocks the hyperextension of the MPJ. Basically, by having the trim lines on the dorsum of the proximal phalanx, the static splint blocks the hyperextension of the MPJ. There is no way the MPJ can hyperextend against the block. Alternatively, the dynamic splint provides resistance against the hyperextension by using rubber bands. Therefore, the patient would have to hyperextend against the bands. Alternatively, surgery in comparison to orthotic treatment is a lot more invasive. Surgery healing time generally takes longer. Surgery success and healing time hinders upon factors such as age and time period between injury and surgery. There is also significant data showing that improvements of the nerve after surgery can continue for 5 years (Ruijs, Jaquet, Kalmijn, Giele and Hovius, 2005, p.490).
In this case study, surgical intervention can be ruled out due to the patients age and goals. As the patient is 64 years old, surgery may not be as beneficial compared to someone who is younger. The patient also wants to return to work as soon as possible, and as surgery healing time can take up to 5 years this is not suitable. In terms of orthotic treatment, the static ulnar nerve palsy splint is more appropriate. The static splint is more suitable for the patient as it has less components to it, making it a more sturdy and durable option for returning to work.
Search Strategy
[edit | edit source]A search strategy was used to find information on ulnar nerve lesions. The databases I used included Medline, Cochrane and CINAHL. Google Scholar and the La Trobe University library search were extremely helpful in collaboration with the other databases. The search terms I used to find information included ulnar nerve palsy splints, claw hand splints, ulnar nerve lesions, treatment of ulnar nerve lesions, orthotic treatment and surgical treatment for ulnar nerve lesion.
Reference List
[edit | edit source]Colditz, J. (1995). Splinting the Hand with a Peripheral- Nerve Injury. Rehabilitation of the Hand: Surgery and Therapy, 4, 622-626. Retrieved fromhttp://www.handlab.com/ckfinder/userfiles/File/Rehab_Hand_2002_p_622-634_Nerve_Splinting(1).pdf
Dell, P, C., & Sforzo, C, R. (2005). Ulnar Intrinsic Anatomy and Dysfunction. Journey of Hand Therapy, 18(2), 198-207. Retrieved from http://0-search.proquest.com.alpha2.latrobe.edu.au/docview/222227197/fulltextPDF?accountid=12001
DeSouza, R, M., & Choi, D. (2012). Peripheral Nerve Lesions. Neurosurgery, 30(3), 149-154. Retrieved from http://ac.els-cdn.com
Duncan, R. (1989). Basic Principles of Splinting the Hand. Journal of the American Physical Therapy Association, 69, 1104-1116. Retrieved from http://ptjournal.apta.org/content/69/12/1104.full.pdf+html
Foss-Campbell, B. (1998). Principles of Splinting the Hand. Plastic Surgical Nursing, 18(3), 199-203. Retrieved from http://0-search.proquest.com.alpha2.latrobe.edu.au/docview/203326263/fulltextPDF?accountid=12001
Hong, C, Z., Long, H, A., Kanakamedala, R, V., Chang, Y, M., & Yates, L. (1996). Splinting and Local Steroid Injection for the Treatment of Ulnar Neuropathy at the Elbow: Clinical and Electrophysiologial Evaluation, American Academy of Physical Medicine and Rehabiliation, 77, 573-577. Retrieved from http://ac.els-cdn.com
Paksima, N., Besh, B, R. (2012). Intrinsic Contractures of the Hand. Hand Clinics, 28(1), 81-86. Retrieved from http://ac.els-cdn.com/S0749071211001053
Parry, C, B, W., Harper, D., Fletcher, I., Dean, A, E., Knight, P, N., & Robinson, A, R. (1970). New Types of Lively Splints for Peripheral Nerve Lesions Affecting the Hand. The Hand, 2(1), 31-38 http://ac.els-cdn.com/0072968X7090032X/1-s2.0-0072968X7090032X-main.pdf
Paternostro-Sluga, T., Keilani, M., Posch, M., & Fialka-Moser, V. (2003). Factors that Influence the Duration of Splint Wear in Peripheral Nerve Lesions. American Journal of Physical Medicine and Rehabilitation, 82, 86-95. Retrieved from http://0-ovidsp.tx.ovid.com.alpha2.latrobe.edu.au/sp-3.11.0a/ovidweb.cgi
Pfaeffle, H, J., Waitayawinyu, T., & Trumble, T, E. (2007). Ulnar Nerve Laceration and Repair, Hand and Microvascular Surgery, Department of Orthopaedics and Sports Medicine, 23, 291-299. Retrieved from http://ac.els-cdn.com
Robertson, C., Saratsiotis, J. (2005). A Review of Compressive Ulnar Neuropathy at the Elbow. Journal of Manipulative and Physiological Therapeutics, 28(5), 1-17. Retrieved from http://ac.els-cdn.com/S0161475405001053/1-s2.0-S0161475405001053-main.pdf
Ruijs, A, C, J., Jaquet, J, B., Kalmijn, S., Giele, H., & Hovius, S, E, R. (2005). Median and Ulnar Nerve Injuries: A Meta-Analysis of Predictors of Motor and Sensory Recovery after Modern Microsurgical Nerve Repair. Plastic and Reconstructive Surgery, 116, 484-494. Retrieved from http://0-ovidsp.tx.ovid.com.alpha2.latrobe.edu.au/sp-3.11.0a/ovidweb
Scheker, L, R., Chesher, S, P., Netscher D, T., Julliard, K, N., & O’Neill, W, L. (1995). Functional Results of Dynamic Splinting after Transmetacarpal, Wrist, and Distal Forearm Replantation. Journal of Hand Surgery, 20, 584-590. Retrieved from http://0-jhs.sagepub.com.alpha2.latrobe.edu.au/content/20/5/584.full.pdf+html
Seror, P. (1993). Treatment of ulnar nerve palsy at the elbow with a night splint. Journal of Bone & Joint Surgery, British Volume, 75(2), 322-327. Retrieved from http://www.bjj.boneandjoint.org.uk/content/75-B/2/322.short
Shin, R., & Ring, D. (2007). The Ulnar Nerve in Elbow Trauma. The Journal of Bone and Joint Surgery, 89(5), 1108-1116. Doi: 10.2106/JBJS.F.00594
Functional Aims and Goals
[edit | edit source]The functional aims and goals of splinting ulnar nerve lesion are based on opposing the claw deformity and to enhance the function of the device to enable the patient to return to work. To achieve a successful outcome the splint needs to incorporate:
- A hyperextension block to prevent hyperextension of the MPJ evident in intrinsic minus hand or claw hand. Immobilising the MPJ in flexion corrects the deformity and promotes healing of the ulnar nerve.
- Equalise the pressure of the hyperextension block to ensure pressure is equally distributed on the dorsal proximal phalanges and to prevent any pressure areas.
- Free flexion ROM is required in the 4th and 5th digit to allow the unimpaired intrinsic muscles to perform their movements and to enhance the function.
- Allow thumb opposition to enhance the function of the splint.
- Reduce the surface area of the splint to reduce any material from impeding on the sensory areas of the median nerve and to produce enhanced function for the individual.
- Strap is positioned so that the loose section is placed on the dorsal section of the hand to minimise it getting caught on things and getting in the way.
The functional aims and goals for the plaster of paris (POP) cast and low temperature thermoplastic (LTT) ulnar nerve palsy splint are identical. The POP cast may be used initially for the first week if there was any swelling evident. However, long-term splinting would be achieved by using the LTT as it is more durable, lightweight, aesthetically pleasing and comfortable. Ultimately, the LTT would be better in a tough work environment compared to the POP and would enable the patient to return to work.
Design
[edit | edit source]Positioning
[edit | edit source]The positioning of the static splint is designed to oppose the deformity that exists in claw hand. To oppose the claw deformity the following positioning is required:
- MPJ hyperextension block.
- Free flexion of the 4th and 5th digits.
- Opposition of thumb is required for functional purposes.
Trimlines
[edit | edit source]To achieve correct positioning, appropriate trimlines are required:
- MPJ hyperextension block positioned on the dorsum of the proximalphalanx of the 4th and 5th digit. This should be molded equally to ensure correct distribution of pressure.
- Distally, the hyperextension block should finish at the axis of the proximal IPJ. This allows functional flexion.
- Ensure that the surface area of the thermoplastic is as small as possible. This is important, so it does not impede on the uninjured median nerve.
Patterns
[edit | edit source]To achieve the appropriate trimlines the orthotic device requires a hand component and a loop component. This is achieved by a pattern:
- Trace around the hand.
- The hand component distal trimlines are the distal palmer crease. The proximal trimlines is two fingers width below the distal trimline. The width is double the size of the hand, as it wraps around the entire circumference of the hand (fg.1).
- The loop component involves positioning tabs that overlap the hand component. The width of the loop is about 2.5cm wide the whole way around (varying patient to patient). The proximal trimlines should finish at the proximal IPJ of the ring fingers (fg.2).
-
Figure 1. Hand Component.
-
Figure 2. Loop Component.
Attachment Methods
[edit | edit source]Attachment methods for the thermoplastic and straps are identical. This is achieved by using a heat gun. It is important to heat up both surfaces and materials that you are attaching to ensure the join is of high integrity.
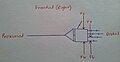
Force System Diagrams
[edit | edit source]-
F1, F2 and F3 are creating the flexion moment at the MPJ. This is resisting any extent on the MPJ. Although, at the same time allowing free flexion of the IPJ.
-
F4 and F5 are resisting any abduction and adduction forces of the MPJ. F6 and F7 are controlling digits 4 and 5 by preventing any extension, abduction and adduction forces.
Design Drawings
[edit | edit source]Manufacturing process
[edit | edit source]- Create template of the hand and loop components and cut out.
- Turn the fry pan on to initiate boiling process.
- Position patient in correct position: the patient should be sitting at a height where the hand is easily accessible. The wrist should be in a neutral position with the MCPJ in flexion (fg.1).
- Place the hand piece in the fry pan first; leave untill the thermoplastic is moldable.
- Apply thermoplastic hand piece to hand; mold it smoothly onto hand. Ensure there are no creases.
- Any alterations required at the hand piece are recommended at this stage.
- Take off hand piece and proceed to place loop piece into fry pan (fg.2).
- Once the thermoplastic loop piece becomes moldable, place it on patient ensuring they’re in the appropriate position.
- Once you ensure that the loop is performing its desired outcomes, ensure trimlines are neat and correct. Any alterations are recommended at this stage.
- Apply both pieces to the patient; mark out the attachment points for the loop and hand piece.
- Heat up both attachment points with the heat gun. Then attach both components together.
- Then, with the straps, cut them down to their appropriate length. Place the velcro strap on the thumb side of the hand piece and the velcro hook on the dorsum of the hand.
- To connect the velcro strap and hook, use a heat gun on the thermoplastic and velcro strap and hook.
- At this stage, you have your ulnar nerve palsy splint. However, there is time to ensure that there are no sharp edges and trimlines are correct. To alter any sharp edges or edit trimlines, heating the thermoplastic up in the fry pan can make it easier to work with. You can cut or shape the edges accordingly (fg.3).
- To ensure there is no pen marking, you can use acetone.
-
Figure 1.
-
Figure 2.
-
Figure 3.
Critique of fit
[edit | edit source]-
Critique
Outcome measures
[edit | edit source]Outcome measures are used to determine whether the orthotic device has been successful. The outcome measures chosen for the ulnar nerve palsy are representative of measuring his overall disability and personal goals. In order to measure the desired outcomes, the Disability of the Arm Shoulder and Hand (DASH) outcome measures was used.
To access the extent of the disability of the hand, the DASH outcome measures were used. Based on the 30 questions involved in the DASH, a number is calculated depending upon the response; 100 represents high disability and 0 represents no disability. At 0 weeks, the patient reported a total score of 82. Then at 8 weeks, the patient repeated the test and scored 62. The difference of 20 indicates that the ulnar nerve palsy splint reduced the disability of the hand.
The patient’s personal goals included minimising the deformity to be able to return to work as soon as possible. In order to obtain whether the splint enabled the patient to return to work the DASH Work Module component was used. The maximum score of 100 results in the impossibility to undertake work, and the minimum means work is normal once again. The patients first measurement was 75 meaning working was severely difficult and prevented him from working. However, after 8 weeks, the patient recorded a score of 38. Therefore, it can be concluded that the splint enabled the patient to work, albeit with mild-moderate difficulty.
Therefore, the splint was successful in minimising the disability and allowed the patient to return to work.
Referral Letter
[edit | edit source]Mr. David Davis West Bundoora Physiotherapy Centre
Date: 29 May 2014
Dear Mr Davis,
Thankyou for seeing Mr Toffolo, regarding his ulnar nerve palsy condition.
Mr Toffolo is a fit 64-year-old male, who works for himself as a carpenter. His ulnar nerve lesion has resulted in an intrinsic minus hand. The hand has clawing of the fourth and fifth digits and hyperextension of the metacarpophalangeal joint. The ulnar nerve lesion sustained obstructs the hypothenar and lumbricals muscles. This results in the patient possessing an inability to open his hand to grasp large objects and to abduct and adduct the fifth digit. Mr Toffolo’s goals are to minimise the deformity thus allowing him to return to work.
Treatment thus far has consisted of Mr Toffolo using a low temperature thermoplastic ulnar nerve palsy splint. The splint consists of a hyperextension block, to prevent hyperextension of the MPJ in the 4th and 5th digit. Free flexion, of the 4th and 5th digit is allowed so that the unimpaired intrinsic muscles can perform movements to enhance function. Thus far, treatment has reduced claw hand significantly, however, flexion is still inhibited to a maximum of 10 degrees in the 4th and 5th digits.
Patient has completed the Disability of the Arm, Shoulder and Hand Questionairre (DASH) and has shown improvements from 8 weeks of using the splint. The DASH outlines the patient has improved their overall disability in the hand. Additionally, the patient’s ability at work has improved and has enabled him to return to work albeit with mild-moderate difficulty. However, I believe physiotherapy will enhance Mr Toffolo’s improvement already made.
Please kindly assist Mr Toffolo to minimise the deformity and to increase flexion ROM in the metacarpophalangeal joints of the 4th and 5th digits. Additionally, please assist the patient to increase their ability to grasp large object and abduct and adduct the 5th digit. Thankyou in advance for accessing the patient, if you have any queries please feel free to contact me on 0438 299 750.
Yours sincerely, Luke McNeil Bundoora Orthotics