Upper Limb Orthotics/Trigger Finger
Describe your case study
[edit | edit source]The patient is a 59-year-old female who complained of pain at the base of her fourth and fifth metacarpophalangeal (MCP) joint of the right hand. She spent most of her working years as a receptionist, however now retired she is a grandmother and uses her dominant right hand on a daily basis for cooking, sewing and gardening. She has trigger finger, which is an inflammatory condition of the flexor tendons in the digits, making the finger trigger or snap. To decrease some of the discomfort and pain, the patient is also taking anti-inflammatory medication. She would like to be able to return to her sewing and active lifestyle.
Written information
[edit | edit source]Evidence
[edit | edit source]Trigger finger, also known as stenosing synovistis a condition where flexor tendons; flexor digitorum superficialis and flexor digitorum profundus in the finger trigger or snap with movement due to the thickening of the A1 pulley sheath. It also affects the flexor tendons in the thumb, flexor pollicis longus and flexor pollicis brevis. Initial treatment for this condition is conservative, with a prescribed orthosis to immobilize the metacarpophalangeal (MCP) joint for approximately 6 weeks. If the condition is still present, injections of cortisone and surgery are also utilized to treat the condition with high success rates. If all else fails, surgery can alleviate the problem.
Patients with trigger finger often present with painless clicking, eventually developing into painful triggering radiating to the MCP joint and or proximal interphalangeal joint (Ryzewicz, M., & Wolf, J. M, 2006, p. 135). The mechanism to this injury thought to be the repeated forceful movement of flexing the phalanx. There is no official diagnostic test; most Trigger Finger conditions are diagnosed through the presence of symptoms being so particular. However, a simple injection of lidocaine into the sheath can relieve the pain associated, allowing for active and or passive movement of the digit (Makkouk, Oetgen, Swigart, & Dodds, 2008, p. 93).
The pathophysiology of Trigger Finger is the hypertrophy and inflammation of the retinacula sheath that restricts the movement for the flexor tendons (Makkouk, Oetgen, Swigart, & Dodds, 2008, p. 92). The A1 pulley due to its location is subjected to the highest amount of force especially during a power grip (Makkouk, Oetgen, Swigart, & Dodds, 2008, p. 92). Lundin, Eliasson, & Aspenberg (2012) believe that it stems from a malfunction or abnormality of the pulley, creating the triggering in the fingers (p. 235). Trigger finger originates from the proximal end of the metacarpal joint, in this instance the right first metacarpal joint, where a great degree of flexion occurs. Secondly, nodules are created through further irritation; the sheath is constricted and restricts the flexor tendons from sliding through efficiently. Hueston & Wilson (1972) believe that resultantly the tendon fibers commence spiraling, which consequently bunch together and become further restrained (p. 258).
The narrowing of the joint continuously with force is the main clinical problem that needs to be assessed. Majority of patients exhibiting trigger finger are middle-aged women who can be associated with other diseases including, rheumatoid arthritis, diabetes and changes to the integrity of the connective tissue (Colbourn, J., Heath, N., Manary, S., & Pacifico, D, 2008, p. 336). Comparatively, Ryzewicz and Wolf (2006) believe that the majority of trigger finger cases are idiopathic and mainly affect the first and fourth digits of the hand (p. 135).
Orthotic treatment options
[edit | edit source]
The first type of intervention prescribed is the conservative option of splinting the finger in extension. Whilst splinted the finger tension that was applied to the A1 sheath is null, allowing a significant amount of time for repair, approximately six weeks (Akhtar, Bradley, Quinton, & Burke, 2005, p. 32). Akhtar et al. (2005) stated that other diseases can compromise the healing time making the treatment using an orthosis less beneficial and or increasing treatment time (p. 23). Ultimately the goal of the orthotic intervention is to prevent friction caused by the tendon movement in the retinacula sheath. Designing an orthosis to treat Trigger Finger can be difficult for a number of biomechanical reasons; firstly the short length of the bones decrease the leaver arms and therefore the force applied by the thumb and secondly the thumb has a number of joints, taking into consideration their function (Bowker, Condie, Bader, & Pratt, 1993, p. 199). The above factors can decrease the client’s compliance rate as the orthosis can limit the functions of the thumb and or fingers if not designed effectively. Designing the orthosis is dependent on the location of the Trigger Finger, be it on a single finger, multiple fingers or thumb. For a single digit Trigger Finger located on a finger or thumb the same orthosis is advised upon. A static finger circumferential orthosis that immobilises the proximal interphalangeal joint but allows metacarpal phalangeal and distal interphalangeal joint movement (Valdes, 2012, p. 90). Valdes (2012) designed this orthosis with the understanding that the palm was left unhindered whilst the interphalangeal joint immobilization would restrict the flexor tendon movement and therefore alleviate reaction (p. 90-91). Similarly, if there is multiple digits affected a different orthosis is used, a modified boxer splint. The MCP joint in completely immobilised with roughly 10 to 15 degrees of flexion, this allows enhancing the hand function of opposition (Valdes, 2012, p. 91). Success rates of this treatment are conditional to the fit of the orthosis and compliance of the patient. In the literature there is a variety of statistics and their perception of success rates. Patel and Bassini (1992) found the success rate of orthoses in treating Trigger finger to be 70% (p. 112). Comparatively, there was an 85% success rate in a study of 40 patients by Valdes (2012, p. 93).
Other Treatment Options
[edit | edit source]Corticosteroid Injection
[edit | edit source]
The second conservative treatment option for Trigger Finger is injections of corticosteroid. The main function of this steroid is to decrease the inflammation of the A1 pulley, subsequently reducing friction and pain. This injection was introduced as a method of treatment in the 1950’s and should be tried before surgery, as it is very efficacious. Since then it has had continuously increasing high success rate, a study done by Vlades (2012) had a success rate of 87% and 38-90% by Akhtar et al. (2005) comparatively (p. 93; p. 32). However, there is evidence in the available literature as to where to administer the corticosteroid injection. Originally, insertion of the injection was directly into the effected sheath, yet Makkouk et al. (2008) believe that the best outcome came from the injection being injected from the subcutaneous tissue that surrounds the effected A1 pulley (p. 94). Additionally, Makkouk et al. (2008) also believe that if the patient has had the condition for more than 6 months the chances of the corticosteroid injection working is slim (p. 94). With any steroid injection come the risks, and possible side effects. Those included with the corticosteroid injection are dermal atrophy, skin hypopigmentation and fat necrosis. There are also risks associated with the third and final treatment option of Trigger Finger.
Surgery
[edit | edit source]
If both of the conservative treatment methods are found to be ineffective surgery is the final option for the patient. There are two variations of surgery that are both done under a local anesthetic. The open release surgery for Trigger Finger consists of an incision being made distal to the distal palmar crease or the xexor crease of the thumb at the MCP joint for Trigger Thumb (Lange-Riess, Schuh, Hönle, & Schuh, 2009, p. 1619). The A1 pulley is exposed and then dissected, however, great care needs to be taken during this procedure to not compromise the digital nerves that run distal to the incision cite, the thumb specifically. Żyluk, & Jagielski (2009) describe this surgery as being done in a ‘bloodless operative field’ where the blood flow is restricted just below the bracial plexus of the affected hand and the anaesthesia is administered into the nerve directly at the cite of incision (p. 276). This technique is more time consuming and expensive compared to the second technique.
Percutaneous release is a slightly less invasive technique, with the only piece of equipment used being a hypodermic needle to release the retinacula sheath (Żyluk & Jagielski, 2009, p. 268). Complication rates are slightly higher in this procedure in comparison to the open release technique as it is theoretically done blind, increasing the risk of flexion deformity, nerve transection and reoccurrence (Żyluk & Jagielski, 2009, p. 268; Makkouk et al., 2008, p. 95).
Success rates of both techniques are high in comparison to other treatment options. Lange-Riess, Schuh, Hönle, & Schuh (2009) found that 98% of their participants were successful in regain function of their affected finger or fingers (p. 1619). Similarly, Makkouk et al. (2008) reported success rates ranging from 90% to 100% (p. 95).
Overall, there are three treatment options for Trigger Finger, some more conservative than others. The conservative option of orthosis treatment is typically the first type of intervention where finger tension that was applied to the A1 sheath becomes null, allowing a significant amount of time for repair. Secondly, a corticosteroid injection can be administered to decrease the inflammation of the A1 pulley and subsequently reducing friction and pain. Lastly, surgery is the final treatment option, which can be done two ways, both with risks but high success rates in rectifying Trigger Finger.
Appendix 1
[edit | edit source]Search Strategy
Databases used: Medline, Cochran, CINAHL, PubMed
Search Terms
Trigger finger, stenosing synovistis, trigger thumb
Aetiology, pathology, mechanism
Treatment, orthos*, splint*, extension splint*, immobili?ation
Corticosteroid injection, surgery, percutaneous release, open release
Functional Aims and Goals
[edit | edit source]Goals and functional aims of the orthosis are mainly situated around the immobilisation of the fourth and fifth metacarpophalageal joints. In treating trigger finger for the client the hand finger orthosis will prevent the friction that is caused by the tendons sliding through the retinacula sheath, decreasing inflammation and compensatory movements. The thickening of the A1 pully sheath narrows the joint continuously and is the main clinical problem that needs to be assessed.
In immobilising these two metacarpophalangeal joints and allowing for thumb opposition with the second and third phalanx it will still permit for then functional mobility of the hand. Whilst still having some functional ability of the hand the main function of this orthosis is to reduce pain by immobilising the said joints, by not forcing the tendon through the sheath.
The hand finger orthosis covers the majority of the volar aspect and approximately half of the dorsal aspect. However, this is purely for stability and to secure the device to the hand. On the fourth and fifth digits, the thermoplastic is slightly longer on the dorsal aspect in comparison to the volar to allow some mobility of those two digits.
Design
[edit | edit source]The orthosis required for Trigger Finger is a short-term device and is worn by the client for approximately six weeks. It is therefore an interim device and made out of Low Temperature Thermoplastic and supported using Velcor. Trimlines and straps are shown below in the force diagrams.
-
Anterior Force Diagram
-
Posterior Force Diagram
-
Sagital Force Diagram
Manufacturing process
[edit | edit source]Equipment
- Electric frypan
- Scissors
- Marker
- Velcro
- Low Temperature Thermoplastic
- Paper
- Heat Gun
1) In making the template of the orthosis, place the affected hand on a piece of paper with the thumb completely extended, the second and third digit together and the fourth and fifth digit together, leaving a V. Trace around the hand.
-
Tracing
2) Mark the following landmarks; distal palma crease, proximal interphalageal joints on digits 4 and 5, first metacapophalangeal joint and radiocarpal joint.
-
Stencil
3) To complete the drawing of the template draw the line across the hand of the distal palma crease. Draw two half oval between the lateral aspect of the distal palma crease and the inferior aspect of the metacarpophalageal joint, and the superior aspect of the metacarpophalageal and the lateral aspect of the radiocarpal joint. On the medial aspect of the hand the design is mirrored at the fourth and fifth proximal interphalageal joint. Then the design continues down to a 90 degree angle with the distal palma crease Then continues out medially for 2-3cm and then down again to be in line with the radiocarpal joint.
-
Stencil and HO outline
4) Cut out the paper template and make sure the template fits the client’s hand, however remember the thermoplastic will stretch and has 100% memory.
5) Trace the checked pattern onto the low temperature thermoplastic (LTT). Cut out the pattern roughly on the thermoplastic, then heat the plastic up in the electric frypan and cut out the pattern more easily and with more detail. Lastly before positioning on the client, roll the tabs, distal palma crease and arounf the radio carpal joint.
'6)' Position the clients had in the correct position, with the metacarpophalangeal joints on digits 2-5, flexed at 10-15 degrees and with the thumb opposed in a functional position.
-
Degree of flexion (10-15 degrees)
7) Reheat the thermoplastic and position it onto the clients hand, making sure that it isn’t too hot. Firstly position the LTT under the distal palma crease then wrap the excess around the fourth and fifth digit, making sure it comes up to the proximal interphalangeal joints. Lastly make sure the tabs come around and attach to the dorsal aspect of the hand. As the LTT hardens hold the clients hand in a bikers grip to hold the position.
8) Once it cools down and hardens, make markings on the device that need to be corrected for. Possibly high trimlines or restricting movement. In this case the trimlines around the radiocarpal joint need to be trimmed and remove some off the distal palma crease and tabs that wrap around the thumb.
-
Pre adjustments
9) Fit to the client for a second time, round sharp edges and take measurements for straps.
-
Fitting post adjustments
-
Fitting post adjustments
10) All straps are attached permanently on the palma surface by heating the LTT and loops of the Velco. The hooks of the velcro have an adhesive backing, however if it doesn't the same method used for the loops can be used.
-
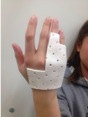
Finished Device (Pamla Surface)
-
Finished Device (Dorsal Surface)
Critique of fit
[edit | edit source]The patient is a 59-year-old female who complained of pain at the base of her fourth and fifth metacarpophalgeal joints on her right hand. The client has had this triggering before when she used to work as a receptionist and has only now become painful. She presented to the clinic with slightly inflamed fourth and fifth MCP joints and subsequent pain. This becomes more sever after doing a lot of sewing and gardening during the day, resulting in the finger becoming stuck during movements through flexion and extension There is no official diagnostic test; most Trigger Finger conditions are diagnosed through the presence of symptoms being so particular. However, a simple injection of lidocaine into the sheath can relieve the pain associated, allowing for active and or passive movement of the digit. The client would really like to be able to get back to her lifestyle of using the dexterity of her hands as soon as possible and decrease the amount of pain she experiences. The referring doctor requested that she be placed in an orthosis for six weeks to immobilise the two MCP joints. With multiple digits affected a different orthosis is used compared to a single effected Trigger Finger. The fourth and fifth MCP joints are completely immobilised with roughly 10 to 15 degrees of flexion, this allows enhancing the hand function of opposition. The orthosis would be made out of a low temperature thermoplastic, as the duration of splinting is not long enough to make a definitive device mad out of something more durable.
The custom made device was modelled off a boxer’s splint, as its main purpose is to immobilise the fourth and fifth MCP joints, which is our main objective. It would be more beneficial for the client to have the two phalanxes in full extension, however they were put in slight flexion to maintain functionality of the hand in performing everyday tasks and opposition with other digits. If this device was to be made again, alterations could be adapted to make it a more functional and comfortable hand orthosis.
-
Hand Orthosis-Final (Dorsal Surface)
-
Hand Orthosis-Final (Palma Surface)
-
Hand Orthosis-Fit before straps (Palma Surface)
-
Hand Orthosis-Fit before straps (Dorsal Surface)
- The orange circle shows that the distal palma crease comes up too high and this section of the hand orthosis is not rolled. Can cause rubbing and discomfort for the client.
- The pink circle shows some of the marks left on the devise from marking out the orthosis on the low temperature thermoplastic and the alterations that were made to the orthosis once the thermoplastic had cooled.
- The blue circles show the straps being placed in the correct positions. The client has a relatively small hand and therefore I used smaller straps. They also have tapered edges to prevent scratching.
- The red circle shows the anterior trim-lines, more specifiacally the dorsal surface of the fourth and fifth MCP joints. This dorsal surface could have been longer; currently it is the same length as the palma surface and doesn’t cover the dorsal surface of the proximal interphanlageal joints.
- The purple circles shows the stretching of the low temperature thermoplastic at the medial aspect of the distal palma crease as wells as on the dorsal aspect.
Overall the device will suffice in immoblising the fourth and fifth MCP joints on the client right hand. It will decrease the amount of pain she experiences daily and will act as a reminder. The outcome measure from the Disability of the Arm, Shoulder and Hand Score was tested prior to wearing the device. She obtained a score of 35.8. She will also be tested after wearing the device for 2 weeks.
Outcome measures
[edit | edit source]Three outcome measures were tested on the client; they included a Disabilities of the Arm, Shoulder and Hand Questionnaire (DASH), ROM testing and Muscle grading.
Pre Hand Orthosis
With the Dash Assessment the client scored a 35.8 out of 100, where 100 is a great disabling impact on daily life (Institute for Work & Health, 2013). The DASH outcome measure is comprised of 30 questions scored from 1 to 5, based on the severity of disability and symptoms. There is a second section of an additional 4 questions based on high performance in relation to sport, music or work. In scoring a 35.8 it shows that the client has had a mild interference with daily living due to her Trigger Finger. (Hudak, Amadio, & Bombardier, 1996).
A ROM assessment was tested on the client’s effected fourth and fifth digits. Flexing the fingers at the MCP joint caused some pain, however in attempting to fully extend the fingers they became stuck and finally released after an audible click, this was due to the nodule sliding under the first pulley.
An Isometric Muscle Grading Assessment was also conducted on the client. The scale ranges from 0-5, with the client receiving a 4. This is against gravity as well as additional resistance. A muscle grading of 5 was not achieved as that would imply resistance against maximal force, however if too much resistance was applied this cause the client pain.
There are a number of outcome measures that can be done for the client, however considering the age and activity level of the client the DASH, ROM and Isometric Grading are suitable. There is some improvement that can be obtained for all three tests even though she scored relatively well on all.
The outcome measures would be performed again in 6 weeks time, after the client has had their hand immobilised in the Hand Orthosis.
-
Making Breakfast with Hand Orthosis
-
Writing with Hand Orthosis
Post Hand Orthosis
After wearing the Hand Orthosis the client has experienced less pain and no triggering of the affected digits. Their score on the DASH questionnaire decreased significanty from 35.8 to an 8.3. The only issues she had were related to strength, she also therefore still obtained a 4 on the Isometric Muscle Grade. This can be overcome with the assistance of a physiotherapist. Lastly her ROM has been fully restored and can now flex and extend her fourth and fifth digit.
Referral Letter
[edit | edit source]Dear Rebecca Jones
I am referring to you a 59 y.o female client who presented to the clinic with pain and swelling at the proximal ends of her fourth and fifth digits on her right hand. She is a retired receptionist and grandmother that spends the majority of her time cooking, sewing, gardening and looking after her grandchildren. General Practitioner, Dr. Pete Hart, assessed the patient at the Wantirna South Medical Centre and referred her to our clinic. Dr. Hart came to the conclusion that she was suffering from Trigger Finger in her fourth and fifth digits and prescribed an immobilisation orthosis to be per worn for 6/52.
The patient presented to our clinic and her affected fingers were inflamed at the MCP joints. Nodules were also palpable proximal to the A1 pulley as they became stuck in a flexed position, and releasing after an audible click. ROM was also therefore impinged and an isometric muscle grade of 4.
In having to wear the orthosis for 6/52, it was a collective decision to make a custom-made low temperature thermoplastic orthosis. The device design was to immobilise the MCP joint, whilst still maintain dexterity of the hand. A modified boxer splint was used, with the fourth and fifth digit in 10-15 degrees of flexion to allow for greater functionality.
The patient wishes to be able to return to her active lifestyle that entails looking after her grandchildren and leisure activities such as sewing. If her dexterity cannot be established she will need to be referred back to Dr. Hart for cortisone injections or surgery.
If you have any questions or queries regarding this patient or her current orthotic management, please don’t hesitate to contact me. Yours Sincerely
Shannon Patton
References
[edit | edit source]- Akhtar, S., Bradley, M. J., Quinton, D. N., & Burke, F. D. (2005). Management and referral for trigger finger/thumb. BMJ: British Medical Journal, 331(7507), 30. doi:10.1136/bmj.331.7507.30
- Bowker,P., Condie, D. N., Bader, D. L., & Pratt D. J. (1993). Biomachanical Basis of Orthotic Management. Oxford, England: Butterworth-Heinemann
- Colbourn, J., Heath, N., Manary, S., & Pacifico, D. (2008). Effectiveness of splinting for the treatment of trigger finger. Journal of hand therapy, 21(4), 336-343. doi:10.1197/j.jht.2008.05.001
- Hueston, J. T., & Wilson, W. F. (1972). The aetiology of trigger finger: Explained on the basis of intratendinous architecture. The Hand, 4(3), 257-260. doi:10.1016/S0072-968X(72)80010-X
- Institute for Work & Health. (2013). The DASH outcome measure - Disabilities of the Arm, Shoulder and Hand. Retrieved from http://www.dash.iwh.on.ca
- Lange-Riess, D., Schuh, R., Hönle, W., & Schuh, A. (2009). Long-term results of surgical release of trigger finger and trigger thumb in adults. Archives of Orthopaedic and Trauma Surgery, 129(12), 1617–9. doi:10.1007/s00402-008-0802-8
- Lundin, A. C., Eliasson, P., & Aspenberg, P. (2012). Trigger finger and tendinosis. Journal of Hand Surgery (European Volume), 37(3), 233-236. doi:10.1177/1753193411421853
- Makkouk, A. H., Oetgen, M. E., Swigart, C. R., & Dodds, S. D. (2008). Trigger finger: etiology, evaluation, and treatment. Current reviews in musculoskeletal medicine, 1(2), 92-96. doi:10.1007/s12178-007-9012-1
- Ryzewicz, M., & Wolf, J. M. (2006). Trigger digits: principles, management, and complications. The Journal of hand surgery, 31(1), 135-146. doi:10.1016/j.jhsa.2005.10.013
- Valdes, K. (2012). A retrospective review to determine the long-term efficacy of orthotic devices for trigger finger. Journal of Hand Therapy, 25(1), 89-96. doi:10.1016/j.jht.2011.09.005
- Żyluk, A., & Jagielski, G. (2009). Results of the Treatment of Trigger Finger - A Review. Polish Journal of Surgery, 81(5), 265–271. doi:10.2478/v10035-009-0041-x