Upper Limb Orthotics/Orthotic management of radial nerve palsy following humeral fracture
Describe your case study
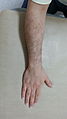
[edit | edit source]The patient is 45 years old male who had suffered a closed, incomplete fracture at mid to distal end of the humerus following a bicycle accident. Patient was not under any medication and his health signs are good. This accident resulted a radial nerve palsy which denied him to use his right hand to grasp properly. The patient is currently using a functional humeral brace for about 2 weeks and was able to flex his forearm and wrist. Although not at peak capacity, however, at this stage he is considering using a splint to regain some use of his right hand.
Written information
[edit | edit source]Background
[edit | edit source]The treatment process of radial nerve palsy due to fractures of the humeral shaft has been discussed in the literature. Two studies by Shao, Harwood, Grotz, Limb & Giannoudis (2005, p. 1651) and Liu, Zhang, & Wu (2012, p. 708) which have systematically reviewed the literature agreed that initial intervention either conservation or surgical means have high recovery rate. Shao et al. (2005, p. 1648) reported no significant difference in results between the two approach. However, Liu et al. (2012) as suggested from his conclusion that non-operative measures should be used first to avoid complications that may arise from surgical interventions. Furthermore, based on Shao et al. (2005, p. 1648) findings, about 70.7% of a group of patients that went with non-operative measures had recovered within three weeks. Therefore it is unnecessary to operate on a patient if there is an expectancy that the patient will recover in a timely fashion. Given the condition of our patient in this case study, it is best to treat our patient by using the non-operative method.
Anatomy of Radial nerve
[edit | edit source]Radial nerve continues from the posterior cord of the brachial plexus which has origins from C5, C6, C7, C8 and T1 spinal cord. As it travels towards the distal end of the humerus, it innervates triceps and anconeus muscle groups. It then twists around the mid humeral shaft or also known as "spiral groove" and channels through the intermuscular septum. At this point, more muscle groups are innervated by branches of the radial nerve and they are brachialis, brachioradialis and extensor carpi radialis longus. The radial nerve then continues to the lateral epicondyle of the humerus and splits into posterior interrosseous nerve and superficial branch of the radial nerve as it enters into the forearm. The posterior interosseous nerve innervates the supinator muscle first then superficial extensor muscle group (extensor carpi radialis brevis, extensor carpi ulnaris, extensor digitorum, extensor digiti minimi and extensor indicis) and finally the deep extensor muscle group (abductor pollicus longus, extensor pollicis longus and extensor pollicis brevis). (Wang & Weiss, 2013, p. 34).
Etiology
[edit | edit source]Wang & Weiss (2013, p. 36) reported that damages to radial nerve are commonly caused by traumatic accident. It is also due to fact that radial nerve runs closer to the dermis, especially near mid shaft and the lateral epicondyle of the humerus. Any compression, inflammation or deep laceration around these sites might damaged the radial nerve easily due to its anatomical position. McKee & Nguyen (2007, p. 73) further describe the etiology of the radial nerve caused by traction, internal entrapment, external forces exerting or impinging on the nerve, or bullet projectiles. Other pathologies such as diabetes, tumor, leprosy can contribute to radial nerve disruptions but only to a smaller extent.
Functional degradations
[edit | edit source]The main characteristic of radial nerve damaged is the "wrist drop" posture whereby the patient has no motor control to extend the wrist and digits. This will deny the patient to grasp objects simply due to the fact that the patient could not extend the palmar surface to envelope around it. The flexor muscle groups are not affected because they are innervated by either median and or ulnar nerves ( Colditz, 1984, p. 18 ).
Classification of nerve injury
[edit | edit source]Hosalkar, Matzon & Chang (2006) published nerve injuries classification based on Seddon (1943) and Sunderland (1951) published work. The main understanding is that there are three basic types of nerve injuries; neuropraxia, axonotmesis and neurotmesis. Sunderland (1951) added two variations of axonotmesis nerve injury.
Neuropaxia of the nerve is described being a loss of function but structural integrity of the nerve is intact. No degradation of the axon and the prognosis is positive and the nerve will be fully recovered. No surgical intervention is required. (Hosalkar, Matzon & Chang, 2006, p. 88)
Axonotmesis of the nerve meant the "Tinel" sign is occurring slowly and there is signs of axon regeneration. Sunderland's (1951) variations of the axonotmesis describes the level scarring of the axon that prevents it from repairing itself and if there is no signs of healing progress, surgical intervention will be required to repair the damage. (Hosalkar, Matzon & Chang, 2006, p. 88)
The final classification, neurotmesis indicates that the nerve is severed and no self repairing will occur. At this stage only surgical intervention could regain the nerve's function. (Hosalkar, Matzon & Chang, 2006, p. 88)
Another study conducted by Niver & Ilyas (2013) suggests that physical examination should be carried out to find the extent of the nerve injuries to the motor and or sensory neurons. Tests performed on wrist and fingers by means of extension and sensation testing by "light touch" or "pin prick". This method is useful for pinpointing the level of injury and the progress of the neural repairs if any. However, physical testing on patient's with radial nerve paralysis is not always the best choice because the interruption in the axon meant, the action potential of the nerves cannot travel down to the targetted muscle group.
Static and dynamic orthotic treatment
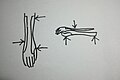
[edit | edit source]Non-operative treatment is currently in place for our patient. The first orthotic option is based on Duncan's (1989) research, a static splint is commonly used to hold, immobilise or support the hand. The three point force system is applied to the forearm (distal to the hand), at the wrist (stabiliser) and hand (volar aspect of the palm, below the crease line of the metacarpal heads - to allow flexion and provide a resistant force to keep the palm up).
The splint holds the "drop wrist" in a power grip position to allow flexion. The hand position about the wrist must be slightly extended to about 25 degrees and slightly ulnar deviated 5-10 degrees. This "cock-up wrist" splint statically position the hand in a power grip position, however, it does not help to extend the digits out. It retains a "claw" like posture at rest. Furthermore, Duncan (1989, p. 1104) explained that the latch at the forearm acts as a lever and it required enough length to hold the weight of the hand.
Second orthotic options, Crochetiere, Goldstein, Granger & Ireland (1975) discussed using a dynamic orthotic design named "Granger" to allow full flexion of the hand by utilising gravity. This is done by having a fixed horizontal bar over the proximal phalanx from the forearm cuff. This allow finger stirrups attached to the horizontal bar. When the hand is relaxed, the weight of the hand itself drops down due to gravity and the digits placed in the stirrups extend out.
After the "Granger" design were introduced, a few variations of dynamic orthosis have taken shape. One such splint was designed having "tenodesis" like function to extend the digits. (Hannah & Hudak, 2001, p. 196)
Comparison of static and dynamic orthotic treatment
[edit | edit source]Both static and dynamic orthoses are designed to ascend the position of the "drop wrist". Both achieved the design goal but when compared in terms of functionality the dynamic orthosis allow better range of motion when flexing and a better grip and release of the object(s). According to a study conducted by Hannah & Hudak (2001, p 199), dynamic orthoses such as "dorsal wrist cock-up with dynamic finger extension splint" and "dynamic tenodesis suspension splint" used by a patient were able to complete all "TEMPA" tasks. The tasks allocated were activites that one might do in their daily live, for example, "pick up and move a jar", "handle coins" and "pick up and move small objects". (Hannah & Hudak, 2001, p. 197). This study found to have sampling and selection bias because it had only one patient. However, the patient preferred the static splint in the end because it was easier to don and doff and less noticeable on her hand compared to the other two dynamic splints.
Conclusion
[edit | edit source]Conservative or early surgical intervention of the radial nerve palsy following humeral fracture have shown high success rate of recovery. Conservative treatment is still favoured due to less complication post surgery and high spontaneous recovery rate. Therefore the initiative to create a model which all clinician can use as a guideline to include time expectancy for "spontaneous recovery" of radial paralysis and time frame for surgical intervention when "spontaneous recovery" has lapsed is warranted. (Shao et al., 2005).
Our patient which is in the early stage of recovery, it is best to fit an orthosis to enable him to increase hand functions in the mean time. The choice to use a static volar cock-up orthosis is within the scope of this project.
References
[edit | edit source]Seddon, H. J. (1943). Three types of nerve injury. 'Brain, 66(4), 237-288. doi:10.1093/brain/66.4.237
Sunderland, S. (1951). A classification of peripheral nerve injuries producing loss of function. Brain, 74(4), 491-516. doi:10.1093/brain/74.4.491
Colditz, J. C. (1987). Splinting for radial nerve palsy. Journal of Hand Therapy, 1(1), 18-23. Retrieved from http://dx.doi.org/10.1016/S0894-1130(87)80007-8
Hosalkar, H. S., Matzon, J. L., & Chang, B. (2006). Nerve palsies related to pediatric upper extremity fractures. Hand clinics, 22(1), 87-98. doi:10.1016/j.hcl.2005.12.2004
McKee, P., & Nguyen, C. (2007). Customized dynamic splinting: orthoses that promote optimal function and recovery after radial nerve injury: a case report. Journal of Hand Therapy, 20(1), 73-88. doi:10.1197/j.jht.2006.11.013
Wang, L. H., & Weiss, M. D. (2013). Anatomical, clinical, and electrodiagnostic features of radial neuropathies. Physical medicine and rehabilitation clinics of North America, 24(1), 33-47. Retrieved from http://dx.doi.org/10.1016/j.pmr.2012.08.018
Duncan, R. M. (1989). Basic principles of splinting the hand. Physical therapy, 69(12), 1104-1116. Retrieved from http://physicaltherapyjournal.com/content/69/12/1104.short
Niver, G. E., & Ilyas, A. M. (2013). Management of radial nerve palsy following fractures of the humerus. Orthopedic Clinics of North America, 44(3), 419-424. Retrieved from http://dx.doi.org/10.1016/j.ocl.2013.03.012
Shao, Y. C., Harwood, P., Grotz, M. R. W., & Giannoudis, P. V. (2005). Radial nerve palsy associated with fractures of the shaft of the humerus A SYSTEMATIC REVIEW. Journal of Bone & Joint Surgery, British Volume, 87(12), 1647-1652. doi:10.1302/0301-620X.87B12.16132
Liu, G. Y., Zhang, C. Y., & Wu, H. W. (2012). Comparison of initial nonoperative and operative management of radial nerve palsy associated with acute humeral shaft fractures. Orthopedics, 35(8), 702-708. doi:10.3928/01477447-20120725-10
Crochetiere, W., Goldstein, S., Granger C. V. & Ireland, J. (1975). The Granger orthosis for radial nerve palsy. Orthot Prosthet, 29(4), 27-31. Retrieved from http://www.oandplibrary.org/op/pdf/1975_04_027.pdf
Hannah, S. D., & Hudak, P. L. (2001). Splinting and radial nerve palsy: A single-subject experiment. Journal of Hand Therapy, 14(3), 195-201. Retrieved from http://dx.doi.org/10.1016/S0894-1130(01)80053-3
Appendix 1
[edit | edit source]Search Strategy Search engines such as Google Scholar, Cinhanl, Embase, Medline, Proquest and Latrobe Library were used to find journal articles which were required to write this assignment. Keywords such as splint, radial nerve palsy, orthosis, orthotics, orthos*, "radial nerve paralysis" and "orthotic management" were used to locate these journals.
Most relevant searches were located when using keywords such as radial nerve and splint especially on Google Scholar.
Functional Aims and Goals
[edit | edit source]The active insufficiency of the flexor muscle groups due to wrist drop, the patient is unable to flex or grip properly. The inability to innervate the extensor muscle groups also create problems such as releasing a grip or supinating the forearm.
The main objective of the static orthosis is to provide support and extend the hand about the wrist. Furthermore, by extending the hand, elongated flexor muscle groups has enough sufficiency to flex better. However, the static orthosis will not be able to aid the patient for any movements exerted by the extensor muscle groups. Action such as releasing a grip can only be done during the eccentric action of the flexor muscle groups. The orthosis must not interfere with the fingers and thumb during flex. Therefore distal part of the orthosis must be folded away from the palmer crease line and the thumb hole is made large enough. This should allow better range of motion at the metacarpal, proximal interphalangeal and distal interphalangeal joints.
The length of the orthosis is used as a leverage in the three point force system. Therefore straps are placed at the proximal end of the orthosis, at the wrist and the distal end of the orthosis (dorsal aspect of the hand).
Either the low temperature thermoplastic (LTT) or the plaster of paris (POP) cast can be use to meet the main objective as discussed above. Both are mouldable on the hand and forearm to achieve the desired outcome. Both materials have their pros and cons. POP cannot be remoulded unlike LTT. But it is cheaper to use in terms of cost.
Design
[edit | edit source]Outline the design of your orthosis, this should include but is not limited to: technical drawings, force system diagrams (3 planes), materials of choice, attachment methods, trimlines and manufacturing procedure. Within this section, if you would choose to make your device from something other than LTT explain why and how this may affect the function of the device you manufacture.
-
Force diagram
Figure 1 shows forces acting on both the frontal (left) and sagittal plane (right).
A low temperature thermoplastic (LTT) product will be use to produce this orthosis. It is relatively easy to mould and cleaner to use than plaster of paris. The LTT is rigid enough for making this orthosis. It makes a good interim and definitive orthosis.
-
Original template
This original template obtained from our LMS resource will be use to create an orthosis.
Alternate Design
[edit | edit source]An different design is to use an outrigger attachment over LTT orthosis. The design would change if I were to pursue this. The outrigger attachment is a piece of metal screwed onto the base (LTT). An off the shelf outrigger such as Phoenix Extended Outrigger Kit (2004) can be bought from the website. The LTT will only be used to create a splint 'base' that stays on the forearm. The outrigger kit is then attached to the splint 'base'. It is made up of metal that sits above the dorsum aspect of the forearm and the hand. The metal part of the outrigger extends beyond metacarpal joints where the hooking point sits and operates the digits.
This design has more functional benefit than the volar static splint because it further increase the palmar surface enabling better surface grip.
Reference:
[edit | edit source]Phoenix Extended Outrigger Kit (2014). North Coast Medical & Rehabilitation Products. Retrived from https://www.ncmedical.com/item_695.html
Manufacturing process
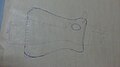
[edit | edit source]1. Outlining patient's hand on a big piece of paper as shown below.
-
Figure 1. Outline patient's hand.
2. Once the outline has been drawn, continue to mark all the required landmarks such as palmar crease line using metacarpal joints on either side of the palm, metacarpal joint of the fifth digits, both styloid processes and the proximal trimline. The keyhole for the thumb is where the vertical line of the 4th digit crosses the horizontal line of the 5th digit.
-
Figure 2. Landmarks.
-
Figure 3. Template over hand
4. Cut the template out and outline it over a sheet of low temperature plastic (LTT).
-
Figure 4. Place template over the LTT
5. Cut out the LTT template and place it into a pan of warm water.
-
Figure 5.
-
Figure 6.
6. Take care when you mold and fit over your client's hand as it might still be hot. You can make it cooler by wiping off excess waterr from the template before fitting.
-
Figure 7. Fitting and molding over the hand
-
Figure 8. LTT will stretch so place the stretched tab over the body and it still maintains the form.
7. The following procedures can only be done when it is still warm. You must rolled the trimline of the distal end of the orthosis below the palmar crease line. This allows the metacarpal 1st, 2nd, 3rd and 4th joints to flex over it. The trimline for the thumb is rolled back down to its carpometaparpal joint (figure 9). This allows flexion movement of the 5th digit. The proximal trimline is flared out like so in figure 10.
-
Figure 9.
-
Figure 10.
8. Because the LTT does get stretched out during molding stage, excess trimlines can be removed by using a strong pair of scissors. Trimlines can be smoothen out further by using a woolly buffer.
-
Figure 11.
-
Figure 12.
9. Small cut out of a plastozote was buffed and velcro straps were heated and stuck onto the body of the orthosis.
-
Figure 13.
-
Figure 14.
10. Finish product of the orthosis. Fit it again on patient's hand and if required, make necessary adjustments.
Critique of fit
[edit | edit source]-
Critique of fit
| Description |
Critique of fit - Marcus.oggtheora.ogv | ||
|---|---|---|---|
| Source |
own work | ||
| Date |
14 May 2014 | ||
| Author | |||
| Permission (Reusing this file) |
|
Outcome measures
[edit | edit source]Disabilities of the Arm, Shoulder and Hand (DASH) has been chosen as a measuring tool for orthotic management of the radial nerve palsy. In order to use DASH, please refer to their website http://www.dash.iwh.on.ca. The online version of the DASH can be obtain from this website http://www.orthopaedicscore.com/scorepages/disabilities_of_arm_shoulder_hand_score_dash.html. DASH is one of the tools approved by Traffic Accident Comission (TAC) and therefore by using standardised tool such as this, the functional outcome measures are more transparent to all bodies involve. DASH questionaires are easy to obtain, written in simple plain english and the questions are relevant to patient's daily activities. Which means it is in compliance with insurance company and clinicians, patients would receive compensation and treatment without being penalised.
DASH tool is used to understand what improvements has been made to patient's daily activities when prescribed an orthosis. The score from the second test is compared to the first test. If there is a significant reduction of points, it means that the patient is getting more functional benefits from the orthosis.
-
DASH survey answered without using an orthosis
-
DASH questionaire used as a measurement for functional outcomes after using an Orthosis.
DASH tool has high retest reliability. Clinician can continue to use the same DASH tool to evaluate the improvements of the patients. It is easy to score and it does not require any statistical means to provide meaningful information. The higher the score obtained, the higher disability level is present. If you use the online DASH survey, it even calculate the score for you. Currently it is free to use. No subscription fee was required and therefore reduces the overhead costs.
The limitation of using this DASH tool is how sensitive each score means. For example, subsequent tests after an orthosis had been prescribed, the patient only scored 2 points less than the previous one. Does that mean he is ready to go back to work, or his daily activities are still hampered from the disability? This is where the situation might be difficult to comprehend. If this situation is not handled right, it could mean that the patient could be forced to work knowing that he is not fully recovered yet. In order extend the outcome measures, the patient can fill in the "work module" survey.
References:
Orthopeadic Scores (2014). The Disabilities of the Arm, Shoulder and Hand (DASH) Score. Retrieved from http://www.orthopaedicscore.com/scorepages/disabilities_of_arm_shoulder_hand_score_dash.html
Transport Accident Commission (2014). Standard Outcome Measures. Retrieved from http://www.tac.vic.gov.au/providers/clinical-resources/outcome-measures#upper
The DASH Outcome Measure (2014). Disabilities of the Arm, Shoulder and Hand. Retrieved from http://www.dash.iwh.on.ca