Upper Limb Orthotics/Intersection Syndrome
Describe your case study
[edit | edit source]- The patient, Sophie, is a female rower aged 25 years. She has been rowing for ten years and semi-professionally for six.
- The patient reported to the GP with pain on radial side of distal right forearm. Slight swelling in distal forearm was seen and pain was greater with flexion and extension of wrist. Slight pain with extension of fingers. Crepitus was noted with movement. NSAIDS were prescribed for inflammation as well as complete rest of the hand and wrist.
- However, the patient found it difficult to completely rest the arm and one week later the pain is persisting. She has a rowing competition in five weeks and needs full use of forearm/hand to compete.
- She works at the local petrol station as a cashier and would like to continue working.
Written information
[edit | edit source]Evidence
[edit | edit source]
Injuries to the forearm occur quite commonly due to overuse or repetition. These are usually associated with sports and sports injuries. Intersection syndrome, also called ‘Oarsman’s wrist’ however, is an uncommon injury of the distal forearm. The distal forearm muscles are divided up into six compartments. Of these compartments, one and two are involved in Intersection syndrome (Yonnet, 2013). Within the first compartment are the Extensor Pollicis Brevis (EPB) and Abductor Pollicis Longus (APL) (Yonnet, 2013), (Gruenberg, & Reagan, 1985, p.299), (De Maeseneer et al., 2009). The APL is responsible for abducting the thumb, as well has having some function in radially deviating the wrist (Jaworski, Krause, & Brown, 2010). The EPB is also associated with abduction of the thumb, however also extends the thumb at the metacarpophalangeal joint (Jaworski, Krause, & Brown, 2010). Within the second compartment are the Extensor Carpi Radialis Longus (ECRL) and the Extensor Carpi Radialis Brevis (ECRB) (Yonnet, 2013). These two muscles are involved with extension of the radiocarpal joint. Due to the anatomical layout of these four muscles and their tendons, it is logical to consider potential injury, especially where these muscles interact.
Intersection syndrome presents with localised pain and swelling around the area where the tendons cross over (De Maeseneer et al., 2009). However, there is individual variation within compartments and in relation to the compartment layout (De Maeseneer et al., 2009). Therefore crossover of these muscle tendons may occur at different locations depending on the individual. According to De Maeseneer et al. (2009) this intersection occurs 3.5-4.8cm proximal to the Lister tubercle. Where other authors suggest this distance may be closer to 4-6 cm (Rettig, 2004), (Shiraj et al., 2013), (Tagliafico, 2009). This crossover of compartment muscles presents an arrangement advantageous to intersection syndrome (Parellada et al., 2007) and this is commonly where swelling is seen. When diagnosing Intersection syndrome, palpation along the posterior radial surface of distal forearm results in tenderness, pain and there is visible swelling at the approximate compartment intersection (Forman, Forman, & Rose, 2005). There may also be crepitus present during wrist flexion and extension and palpation (Rettig, 2004).
The specific pathophysiology of intersection syndrome is not known, however there are theories as to why it occurs. Kaneko, and Takasaki, (2011) suggest two theories as to why this condition occurs. One relies on the idea that friction between the tendons of the two muscle groups results in pain and swelling in the muscle bellies (Kaneko, & Takasaki, 2011). Another theory relies on the idea that the swelling of the muscle compartments causes stenosis, in turn causing pain (Kaneko, & Takasaki, 2011). Yonnet, (2013), suggests that Intersection Syndrome is a peritenosynovitis involving inflammation of the tendon sheaths.
Intersection syndrome is common in those working in the industry or athletes who use their hands repetitively. Intersection syndrome usually occurs a as a results of repeated resistive wrist flexion and/or extension (Yonnet, 2013) as well as radial deviation (Shiraj et al., 2013).
Orthotic treatment options
[edit | edit source]
Generally treatment of Intersection syndrome is conservative. That is with NSAIDS, rest and immobilisation (Shiraj et al., 2013), (Yonnet, 2013). However, sometimes due to a variety of reasons, conservative treatment is not successful. If this is the case, then steroid injection into site of swelling may improve pain (Shiraj et al., 2013).
Commonly orthotic treatment is prescribed involving a wrist/forearm splint involving the thumb. The splint maintains a wrist position of extension with inclusion of a thumb spike (Hanlon, & Luellen, 1999). Specifically, the wrist should splinted in 20 degrees extension (Hanlon, & Luellen, 1999), with this position maintained by the splint for 2-3 weeks. Alternatively, Pantukosit, Petchkrua, and Stiens (2001) suggest 15 degrees of wrist extension. Therefore a comfortable range in the approximate position of 15-20 degrees wrist extension should be appropriate.
Another possible conservative treatment for intersection syndrome is strapping or taping. Kaneko, and Takasaki, (2011) suggest taping of the distal forearm decreases the crepitus/pain. However the authors stated that this result was only seen when the taping was forcefully applied in a direction towards the ulna.
With patients who do not comply with first treatment, it is common to use steroids for the management while surgical treatment is usually only an option for severe cases (Yonnet, 2013).
Surgical treatment is only resorted to where conservative and steroid treatment has failed. Surgical methods are generally used to alleviate muscles within the first or second compartment. Decompressing the muscles of the first compartment may be an option (Williams, 1977). The same technique can be used on the second compartment muscles the ECRL and ECRB (Pantukosit, Petchkrua, & Stiens, 2001).
Comparison of orthotic and other treatment options
[edit | edit source]
As Intersection syndrome is a condition that affects the muscles of wrist extension, complete cease of wrist extension/flexion along with anti-inflammatories would be considered to be best intervention. A prospective study by Pantukosit, Petchkrua, and Stiens, (2001) found that of 30 patients with intersection syndrome, 28 were effectively treated with non-splinting conservative treatment. This treatment included resting of forearm and wrist, as well as modification of everyday tasks to eliminate excessive extension of wrist. However, as the patient compliance to general forearm and wrist rest is poor, physical immobilisation of the wrist would be used to primarily prevent wrist extension.
As the muscles involved in intersection syndrome are involved with thumb abduction, wrist extension, wrist radial deviation and thumb metacarpalphalangeal joint extension, it would be hypothesised that immobilising the joints in these specific positions would alleviate symptoms. Cooper, (2007), suggests a wrist and thumb splint that includes the interphalangeal joint. However, including the interphalangeal joint of the thumb may not be necessary.
Many individual case studies have found that an immobilising orthoses such as a wrist splint effectively alleviates symptoms of Intersection syndrome. In a previous case study on a 35 year old male patient with intersection syndrome, a splint with a dorsal angulation of 20 degrees was prescribed (Yonnet, 2013). The author found that after a prescription of 2 weeks symptoms had been relieved. However, this splint intervention was in conjunction with a change in implementation of everyday activities. This is also supported by similar singular patient case studies and literature (Shiraj et al., 2013), (Pantukosit, Petchkrua, & Stiens, 2001), (Rettig, 2004). These studies also found that a wrist and thumb splint effectively reduces symptoms. As well as this, immobilisation has been found to be effective in a relatively short period of time. Yonnet, (2013) suggests that approximately 12 days is adequate for healing using a well-immobilising wrist splint. The author also suggests that a poorly immobilised wrist would take 32 more days to heal. However, according to previous studies, the average time prescription for an immobilisation splint is 2-3 weeks (Jaworksi, Krause, & Brown, 2010),(Kaneko, & Takasaki, 2011), (Shiraj et al., 2013). Yonnet, (2013) concludes that a wrist orthosis that includes thumb immobilisation would be of most benefit as it immobilizes all four muscles of the first two dorsal forearm compartments, allowing adequate healing.
Other conservative methods of immobilisative treatment include strapping of the wrist. Kaneko, and Takasaki, (2011) describe a study which shows that forceful strapping of the wrist in an ulna direction from the radius is effective in relieving symptoms of intersection syndrome. However, as the patient is non-compliant with simple resting, it is unlikely that strapping would be effective as more thorough immobilisation is needed.
In severe cases of Intersection syndrome where conservative treatment is ineffective, a more radical surgical approach is needed. Effective surgical treatments have been shown in literature (Pantukosit, Petchkrua, & Stiens, 2001), (William 1977). However, this is not needed in the client’s case as physical immobilisation of the wrist is likely to be the most effective option.
Conclusion
[edit | edit source]
Intersection syndrome involves the muscles of the distal, posterior wrist and is caused by repetitive overuse. Pain and swelling occurs where the muscles of the first two compartments cross, aggravated with extension of wrist. Common treatment includes anti-inflammatories and immobilisation, with surgical treatment reserved for extreme cases. Due to the non-compliance to rest, the client’s best option would be to physically immobilise the wrist and thumb in common orthotic splint.
Search Summary
[edit | edit source]
The search strategy involved searching databases PubMed and Google Scholar. Key terms used in search were: intersection syndrome, pathology of intersection syndrome, treatment AND intersection syndrome, wrist extension injuries, extensor carpi radialis injuries, ‘oarsman’s wrist’, thumb spica splint.
Functional Aims and Goals
[edit | edit source]
The functional aims of this orthotic device are to immobilise the wrist, carpometacarpal and metacarpophalangeal joints in a functional, extended position. While the wrist is immobilised, the interphalangeal joint of the thumb needs full range of motion as well as the metacarpophalangeal and interphalangeal joints of digits 2-5. This is to allow the client to remain at work and undertake activities of daily living.
The functional aims of the plaster of paris device are to maintain the same position as the orthotic device. However, as the device needs to be worn for a long period of time, the plaster device is not applicable as it is not durable.
The use of low temperature thermoplastic allows for a lightweight orthotic device that is strong enough to maintain wrist extension. As the device is to be worn for more than a week (Jaworski, Krause, & Brown, 2010, Kaneko, & Takasaki, 2011, Shiraz et al., 2013), it needs to be durable. The device should encompass half the circumference of the forearm to allow for adequate immobilisation of the wrist.
The orthosis should be positioned with the wrist immobilised in a functional position of 15-20 degrees extension/dorsiflexion (Hanlon, & Luellen, 1999, Pantukosit, Petchrua, & Stiens, 2001). The thumb is immobilised in extension at the carpometacarpal and metatarsophalangeal joint. This is to allow the muscles of the first and second forearm compartment to rest and adequately heal.
Design
[edit | edit source]Trimlines


The trim lines extend from 1/3 of the forearm distal to elbow to the distal palmer crease. The device covers approximately half the circumference of the forearm on the volar surface, with the proximal trim line flared for client comfort. The device includes the thumb, covering the MCP joint with the thumb trim line ending just proximal to the IP joint. Figures 1 and 2 show approximate trim lines in both sagittal and coronal planes.
Straps
3 straps are included on the dorsal surface of the device to apply a 3 point force system to maintain position. The straps are attached at the proximal end, over the wrist and at the distal end of device. The proximal and distal straps are placed as far as possible proximally and distally respectively. This allows for a longer lever arm, decreasing the necessary force to keep forearm/hand in required position. Figure 1 and 2 illustrate the positioning of the straps.
Materials
Orthotics device is made out of low temperature thermoplastic as this is easy to mold and is durable for short term use. As the orthosis is worn for approximately 2-3 weeks (Rettig, 2004; Pantukosit, Petchkrua, & Stiens, 2001; Shiraj et al., 2013; Yonnet, 2013;) this material is appropriate. Hook and loop material is used for straps, with the hook being adhesive to attach to the device.
Position
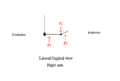
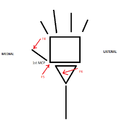
The wrist is positioned in 15-20 degrees of wrist extension (Hanlon, & Luellen, 1999; Pantukosit, Petchkrua, & Stiens, 2001). The inclusion of the thumb in the device allows for maintained extension at the MCP joint (Hanlon, & Luellen, 1999). Figures 3 and 4 shows this position, as well as the forces needed to maintain this position. The forces act to increase wrist extension (Figure 3) and increase thumb extension at MCP joint (Figure 4).
-
Figure 3 Sagittal view of 3 point force system acting to maintain wrist extension
-
Figure 4 Coronal, dorsal view of 3 point force system acting to maintain thumb extension at MCPJ
Manufacturing process
[edit | edit source]1. Trace onto cloth around hand and arm, approximately 2/3 length of forearm to make template. Place thumbhole at the level of the MCP joint and the midline of the first digit. Mark the level of the wrist joint and extend proximally 2/3 of forearm. Add a tab approximately 30 mm distally between 1st and 2nd digit. The distal end should sit at the distal palmer crease. Trim lines extend approximately 20mm medially and laterally from edge of forearm.
2. Place template on hand to ensure the template is correctly positioned and the trim lines are in the correct place. Make and adjustments if needed.
3. Trace template onto low temperature thermoplastic and cut out using shears.
-
STEP 1
-
STEP 2
-
STEP 2
4. Heat up LTT in a water bath at approximately 60° and cut out template.
5. Replace LTT back into water bath to soften again. Whilst the LTT is in the water bath, position client’s arm and hand into required position. This position should be between 15-20 degrees wrist extension with extension of the thumb at the MCP joint. Make sure angles are correct. Ask client to maintain this hand position.
-
STEP 4
-
STEP 4
-
STEP 5
6. When soft enough, gently place on forearm and position correctly. Once positioned, secure around thumb. Mold LTT to contours of arm/hand, continuously making sure correct angles are maintained. Mark trim lines at approximately half the circumference of the forearm.
7. While still warm, remove excess material at the trim lines.
8. Roll back the outside edge of LTT at the distal palmer crease and at the IP joint of the thumb. Then flare the proximal edge of the device.
-
STEP 6
-
STEP 6
-
STEP 7
-
STEP 8
9. Cut out loop tape to correct size and permanently affix to the volar surface between the 1st and 2nd digit. Heat up both the LLT and the hook tape to attach. Attach other end via adhesive hook tape positioned distally at the level of the 5th MCP joint.
10. Attach two more straps positioned over the wrist and at the proximal end of device. Loop tape is attached via adhesive hook tape on the volar side of device. Straps 1 and 2 are attached as far as possible distally and proximally respectively.
11. Check fit of device on client. Check the angles of the writs and MCP joint. Make sure there is no points of excess pressure and trimlines and straps don’t cut into skin.
-
STEP 9
-
STEP 10
-
STEP 11
Critique of fit
[edit | edit source]
The client is a female rower aged 25. She has been rowing for a couple of years and recently reported with pain present on the radial portion of the distal forearm following a training session. When presentation to the clinician, slight swelling was noted at 6cm proximal to wrist with pain present at palpation. Crepitus with pain was seen with any movement of the wrist. Grip strength was noted to be lowered at 20.4 Kg due to pain. A diagnosis of intersection syndrome was given with the prescription of anti-inflammatory medication and complete rest of wrist. However, as the client is active and was not able to rest arm adequately and pain is still present the clinician prescribed a wrist immobilisation splint for 14 days.
The device is designed to hold the wrist in 15-20 degrees of extension as stated be previous literature (Hanlon & Luellen, 1999; Pantukosit, Petchkrua, & Stiens. 2001; Rettig, 2004; Shiraj et al., 2013). As also suggested by literature, it holds the thumb in extension at the carpo-metacarpal joint (Cooper, 2007; Hanlon & Luellen, 1999). The aim of this position is to immobilise the wrist to alleviate pain, whilst maintaining a position that aids healing. While this may impact of the functional ability of the hand, it will aid healing. The straps, positioned over the wrist, proximal forearm and on the distal edge of the device are designed to provide the appropriate force system to maintain this required wrist extension angle. The distal and proximal joints are positioned as far away from the wrist joint as possible to maximise the lever arm and minimise the force required to maintain the extended position. The device is made out of low temperature thermoplastic as this is durable for short term use and is easy mouldable for good fit.
Overall the device fits the client’s arm well. The trim lines encompass approximately half the forearm on the volar surface (figures 2-4). The straps are positioned well (Figure 1) allowing for comfort and applying the appropriate 3-point force system. However, the device is slightly too short and could be lengthened proximally to increase the lever arm of force 1 (Figure 1). The angle of the device does not achieve an adequate position of wrist extension (figure 5). This angle does not pertain to the prescription as indicated by literature. The angle of wrist extension could have been increased by 10 degrees.
-
Figure 2: Position of medial trim line
-
Figure 3: Device coverage of volar surface of fore arm showing distal and proximal trim lines
-
Figure 4: Position of lateral trim line
-
Figure 5: Angle of wrist extension
The orthosis holds the thumb in good extension, though this compromises hand function as this reduces thumb abduction. Whilst this device is a static orthosis, the thumb has complete range of motion at the IP joint. (figure 2 & 3). Whilst the wrist is fixed in extension, the thumb and fingers should have full range of motion from the MCP joints however, there is not sufficient opposition of thumb and fingers. Overall the fit and function is good, however if done again I would make sure the angle of wrist extension is greater. Whilst the thumb was maintained in an extended position to aid healing, this decreases functionality. If done again, I would position the thumb in a more functional abducted position.
Outcome measures are difficult to measure whilst the device is being worn. However, the upper limb extremity functional index (Transport Accident Commission, 2014) is a useful way of measuring functionality whilst the splint is being worn as the client requires to be able to continue working. After ceasing wearing the device, the clients grip strength may be measured to identify any improvement.
Outcome measures
[edit | edit source]The purpose of the device is to immobilise the wrist in an extended position. This is to aid healing and to prevent movement of extension and flexion of the arm. Therefore an outcome measure is hard to choose and hard to measure whilst wearing the device. However, as the client needs to be able to continue working while wearing the orthosis, the Upper Extremity Functional Index (UEFI) (Transport Accident Commission, 2014)is an appropriate measure. This measure was chosen as it is 20 questions focused on the ability to undertake a range of everyday tasks. These tasks would be similar to the tasks undertaken in the client’s work. This measure is used before and after treatment, however, for this client a measure will also be taken whilst wearing the brace to assess functional ability. A more specific outcome measure, the patient-specific functional scale (PSFS) (Transport Accident Commission, 2014) was also used. This measures the ability of the client to undertake a task of their choice. This allows the function of the wrist to be assessed before and after splinting in regards to what is most important to the client. The client chose rowing as the task to be assessed using this measure. This will also be measure before, during and after splinting. Both these measures are easily implemented as they are both simple questionnaires. The UEFI has previously been shown to be reliable and repeatable in a clinical setting (Gabel, Michener, Burkett & Neller, 2006)
The Upper Extremity Functional Index (UEFI)


The UEFI measures function of tasks out of 90. The client’s results of the UEFI were the following;
- Pre-treatment: 39/90
- During treatment: 36/90
- Post-treatment: 68/90
While there is a vast improvement seen between pre- and post-treatment, there is a decrease in scoring between pre- and during treatment. This may be due to total immobilisation at the wrist and the position of the immobilisation. Therefore this measure may not be a good measure during treatment.
Patient-Specific Functional Scale (PSFS)
This scale is a rating scale from 0 to 10 where 0 is unable to perform task and 10 is able to perform task at the same level as before injury. The client chose the ability to row as this functional assessment. Pre-test the client’s rating was 0 as she couldn’t do this task at all. Post-treatment the rating was a 7 indicating healing and improvement in wrist extension. During treatment, the client rated rowing functionality as a 1 as it was very difficult with the wrist immobilised in extension.
Though these measures are a good measure of functionality, they are not specifically tailored to the client’s need. Whilst they may measure how functional the hand is for work purposes, they may not be applicable to the client’s desire to get back into rowing. Therefore, measuring grip strength may be a better indicator of improvement. Grip strength pre-treatment was measured at 20.4kg and increased to 28.2Kg post-treatment which is closer to the reference values in the standard female population (Bohannon et al., 2006).
Referral
[edit | edit source]Due to ongoing weakness in the client's right hand after healing and cease of orthosis wear, the client will be referred to a physiotherapist for ongoing strengthening. The following is the referral letter sent to the referred physiotherapist.
-
Referral Letter
Direct Link to ULO Main Page
[edit | edit source]References
[edit | edit source]Bohannon, R. W., Peolsson, A., Massy-Westropp, N., Desrosiers, J., & Bear-Lehman, J. (2006). Reference values for adult grip strength measured with a Jamar dynamometer: a descriptive meta-analysis. Physiotherapy, 92(1), 11-15. doi 10.1016/j.physio.2005.05.003
Cooper, C. (2007). Fundamentals of Hand Therapy. Elsevier Health Sciences. Retrieved from http://books.google.com.au/books?id=F3nR9eQWJR8C&printsec=frontcover&source=gbs_ge_summary_r&cad=0#v=onepage&q&f=false
De Maeseneer, M., Marcelis, S., Jager, T., Girard, C., Gest, T., & Jamadar, D. (2009). Spectrum of normal and pathological findings in the region of the first extensor compartment of the wrist. Journal of Ultrasound in Medicine, 28(6), 779-786. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/19470818
Forman, A. T., Forman, S. K., & Rose, N. E. (2005). A clinical approach to diagnosing writs pain. American Family Physician, 72(9), pp. 1753-1758. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/16300037
Gabel, C. P., Michener, L. A., Burkett, B., & Neller, A. (2006). The upper limb functional index: development and determination of reliability validity and responsiveness, Journal of Hand Therapy, 19(3), 328-348. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/16861132
Gruenberg, A. B., & Reagan, D. S. (1985). Pathological anatomy of the forearm: intersection syndrome. The journal of Hand Surgery, 10(2), p. 299-302. Retrieved from http://0-www.sciencedirect.com.alpha2.latrobe.edu.au/science/article/pii/S0363502385801295?via=ihub
Hanlon, D. P., & Luellen, J. R. (1999). Intersection syndrome: a case report and review of literature. The Journal of Emergency Medicine, 17(6), pp. 939-971. Retrieved from http://www.sciencedirect.com/science/article/pii/S0736467999001250?via=ihub#
Jaworski, C. A., Krause, M., & Brown, J. (2010). Rehabilitation of the wrist and hand following sports injury. Clinics in Sports Medicine, 29(1), pp. 61-80. Retrieved from http://www.sciencedirect.com/science/article/pii/S0278591909000726?via=ihub#
Kaneko, S., & Takasaki, H. (2011). Forearm pain, diagnosed as intersection syndrome managed by taping: a case series. Journal of Orthopaedic & Sports Physical Therapy, 41(7), 514-519. doi 10.2519/jospt.2011.3569
Pantukosi, S., Petchkrua, W., & Stiens, S. A. (2001). Interseciton syndrome in buriram hospital: a 4-year prospective study. American Journal of Physical Medicine and Rehabilitation, 80(9), pp. 656-661. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/11523968
Parellada, A. j., Gopez, A. G., Morrison, W. B., Sweet, S., Leinberry, C. F., Reiter, S. B., & Kohn, M. (2007). Distal intersection tenosynovitis of the wrist: a lesser-known extensor tendinopathy with characteristic MR imaging features. Skeletal Radiology, 36(3), 203-208. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/17177022
Rettig, A. C. (2004). Athletic injuries of the wrist and hand: part II: overuse injuries of the wrist and traumatic injuries to the hand. The American Journal of Sports Medicine, 32(1), pp. 262-273. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/14754754
Shiraj, S., Winalski, C. S., Delzell, P., & Sundaram, M. (2013). Radiologic case study: intersection syndrome of the wrist. Orthopedics, 36(3), pp. 225-227. doi 10.3928/01477447-20130222-01
Tagliafico, A. S., Ameri, P., Michaud, J., Derchi, L. E., Sormani, M. P., & Martinoli, C. (2009). Writs injuries in nonprofessional tennic players: relationships with different grips. The American Journal of Sports Medicine, 37(4), pp. 760-767. doi 10.1177/0363546508328112
Transport Accident Commision (2014). The upper extremity functional index. Retrieved from https://www.tac.vic.gov.au/providers/clinical-resources/outcome-measures
William, J. G. (1977). Surgical management of traumatic non-infective tenosynovitis of the wrist extensors. The Journal of Bone and Joint Surgery, 59(4), pp. 408-410. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/925050
Yonnet, G. J. (2013). Intersection syndrome in hand cyclist: a case report and literature review. Topics In Spinal Cord Injury Rehabilitation, 19(3), pp. 236-243. doi 10.1310/sci1903-236