Upper Limb Orthotics/Colles' Wrist Fracture
Describe your case study
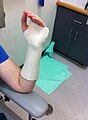
[edit | edit source]The patient, Nancy, is a 65 year old retired female who suffered a colles’ fracture on her right arm following a slip on a wet floor, onto her outstretched hands. She has had no previous wrist fractures. However has recently been diagnosed with osteoporosis. The injury was classified as a 23-A2 fracture according to the Muller AO Classification system, a closed transverse fracture with a minimally displaced distal fragment. No surgery was required and it was deemed appropriate for conservative treatment. It was placed in a POP backslab initially, to let the swelling reduce before a volar wrist splint was applied.
She enjoys gardening and regularly plays lawn bowls. She volunteers with the country women’s association and would like her wrist to be able to cope with the demands for an event in 10 weeks.
Written information
[edit | edit source]Evidence
[edit | edit source]A true Colles’ fracture as defined by Abraham Colles' is a fracture of the distal radius within 2.5 cm of the wrist joint with the distal fragment dorsally displaced. However this term can also be applied to similar fractures that are outside this original definition (Summers, 2005). In elderly patients, it is usually a product of low energy trauma, such as a fall onto outstretched hands and is the most common fracture type in people over the age of 40 (Apley & Solomon, 1993). Nguyen et al (1993) report that it is an instinctive response to put a hand out when falling as this saves injury to the face. Complications can arise from both the fracture and treatment and most commonly include median nerve compression, ligament damage, loss of motion or malunion (Turner, Faber & Athwal, 2007).Turner et al (2010) reported that skin injury was also quite common, especially in elderly patients as overlying skin can be quite thin and could be traumatized during the fracture manipulation. Once the wrist has been fractured, it increases the risk of another wrist fracture threefold and doubles the risk of another osteoporotic fracture occurring. The distal radius is commonly injured as it has the thinnest area of compact bone (Lindsay 1990 & Russell et al. 1990).
Sànchez-Riera et al (2010) state that osteoporosis, the systematic skeletal disease which causes low bone mass and deterioration of bone tissue is often responsible for fragility fractures in the hip, distal radius and ankle regions. The prevalence of osteoporosis increases with age and occurs when bone resorption exceeds bone formation (Nieves, Mosner & Silverstein, 2012). The most useful methods for estimating fracture risk are bone mineral density testing using dual energy x ray absorptiometry and consideration of clinical factors such as gender, age or previous fractures (Sànchez-Riera et al, 2010). If an individual aged 50 or older scores −2.5 T-score or less than the mean BMD value in young females, which is measured at the lumbar spine, hip or femoral neck, osteoporosis may be diagnosed. Age is the most important clinical risk factor and it has been shown that the risk of fracture increases with age and it rises dramatically from 50 to 80 years of age (Sànchez-Riera et al, 2010).
Orthotic treatment options
[edit | edit source]The primary goal of orthotic management is to immobilize the fracture so that healing can occur in the correct alignment and so that the patient can return to normal function as soon as possible (Blakeney, 2010). For this type of fracture, there are many differing opinions and reviews on what position the wrist should be placed in when casting. As a result there is no one definitive treatment. Gupta (1991) has shown that casting the wrist in dorsiflexion has the lowest incidence of the fracture displacing compared to neutral or palmar flexion. However the wrist position can be dependent on the mechanism of injury.
Typically, a below elbow plaster cast is applied as the primary immobilization as it allows some room for swelling after an acute injury. In this case, less layers of plaster would be used for elderly patients to ensure the cast is lightweight (Drozd, Miles, & Davies, 2009). In this case, the initial position of the wrist is slightly extended, between 10 and 20 degrees and in slight ulnar deviation. Upon re-alignment of the distal fragment using a closed reduction technique in this case, some form of padding is layered on the wrist to act as barrier between the skin and the cast (Salvi, 2011). During a 10-day follow-up the original plaster cast may be removed and replaced with a secondary cast such as a thermoplastic volar brace. In a study conducted by Khudairy, Hirpara, Kelly &Quinlan (2012), thermoplastic splints were used to immobilize Colles’ fractures. Patient satisfaction was high and there was no deterioration in radiological outcomes. Fibreglass is also an option, although in this case the use of thermoplastic will be much lighter in weight.
Closed reduction and cast immobilization is the most used form of treatment for minimally displaced, stable fractures, such as this case. Conservative management is also acceptable for unstable fractures in the elderly or those considered too frail to undergo surgery (Blakeney, 2010). Multiple studies have examined the different methods of casting and materials used and anatomical outcomes such as return to function, malunion rates and decreases in angulation. A prospective randomized trial compared the use of plaster casts and prefabricated fibroelastic splints. It concluded that there was no significant difference between casts in terms of anatomical outcome or pain levels, however the splint group scored better in cast satisfaction and had lower complication rates. The lightweight splint also provided a more economic efficient option and allowed faster restoration of function and mobility (O’ Connor et al, 2003). Another study looked at the differences in using a dorsal splint or a complete cast in the first 10 days after the fracture. It was concluded that there was decrease in dorsal angulation in the dorsal cast and the complete cast increased the radial length. However these results were considered to be too small to influence clinical results (Wik, Aurstad & Finsen, 2009).
In addition to conservative management of the wrist fracture, osteoporosis also needs to be treated. One option, vitamin D supplementation with calcium has been shown to reduce the risk of a fracture in patients aged over 65 years and increase bone mineral density (Blakeney, 2010).
Comparison of orthotic treatment options
[edit | edit source]There are many options involved with the stabilization of the distal radius, which include internal surgical techniques such as volar locking plating and percutaneous Kirschner wiring External fixation techniques, wrist bridging or nonbridging are also available, however the age, bone density and fracture classification of each patient are important factors when considering these techniques (Blakeney,2010) . Functional and anatomical outcomes such as radial length, angulation of the distal fragment, mobility and complications are important factors when assessing the success of each treatment (Atroshi et al, 2006). Colles’ fractures in osteoporotic bone have greatly reduced stability which means that surgical fixation is more difficult. The fixation technique used, either pins, wires or plates cannot gain a reliable hold in the bone and this tends to lead to the fracture becoming displaced (Blakeney, 2010).
Fractures of the distal radius have been treated with external fixation techniques since the 1940s and are now more commonly used with unstable fractures. There are two main techniques of external fixation; wrist bridging, where the distal pins are inserted across the wrist joint and into the second metacarpal to immobilize the joint and nonbridging, where distal pins are only inserted into the radius and allows for wrist movement (Blakeney, 2010). The external fixation techniques were compared and it was found that the range of motion at the wrist and forearm 4 weeks after fixation removal was nearly identical, although radial shortening was significantly less with the nonbridging technique. The main weakness of using external fixation are the complications involved, such as pin track infection (Atroshi et al, 2006).
It was thought that internal fixation devices have a much weaker hold in osteoporotic bone and were more likely to loosen and lose fracture alignment. However with the introduction of the fixed-angle locking plate, this has changed the treatment of distal radius fractures in the elderly. The fixed-angle locking screws lock into the plate and don’t rely on any connection with the screw thread in the bone, which reduces the bone instability factor.(Blakeney, 2010). The biggest inconveniences with this technique are the cost involved and the need for a second operation to remove the plates (Maire et al, 2013).In a study conducted by Lee, Wei, Cheng, Hsu, & Huang, (2012) comparing the use of volar plates and percutaneous wiring, it was found that the use of plating increased stability of the fracture and that the reduction of the fracture was maintained better. The cohort of participants were between the ages of 50 and 70 years of age and in both groups of fixation techniques, low complication rates and high union rates.
Surgical treatment of Colles’ fractures remains controversial. Few authors recommend orthopaedic treatment as the first option(Maire et al, 2013 & Chung, Shauver & Birkmeyer, 2009), not only because it is badly tolerated by the patient, but also due to the increased costs involved. Few authors recommend external fixation techniques which is also badly tolerated and can involve secondary infection complications. Many surgeons recommend surgical pinning, which is quick and inexpensive, however this technique may not work well with elderly patients (Maire et al, 2013).
In a patient such as this one, with multiple comorbidities, conservative management is a safer option and is likely to provide similar clinical outcomes as other surgical techniques. Even if malunion occurs, functional outcomes in elderly patients are still acceptable. In between these two options, treatment decisions need to take into account more than the type of fracture and include patient goals, patient preference medical comorbidities and surgeon familiarity with techniques (Blakeney, 2010). Minimally displaced Colles’ fractures such as this case, are common in elderly individuals and have substantial implications on health resources. Results suggest that a lightweight splint offers an acceptable, comfortable and cheaper alternative to a plaster of Paris cast and also allows faster restoration of function without an increased risk of malunion (O’ Connor et al, 2003)
Search Strategy
[edit | edit source]The following databases were used for the collection of these articles: Cinahl, Cochrane, Proquest, Medline and Google Scholar. Search terms such as “colles’ fracture management”, osteoporosis, osteoporosis and women, distal radius fracture, elderly, aged etc.
References
[edit | edit source]Apley GA, Soloman L. Apley’s system of orthopaedics and fractures, 7th edn. Butterworth Heinemann,Oxford, 1993:150. (Apley & Solomon, 1993.)
Atroshi, I., Brogren, E., Larsson, G. U., Kloow, J., Hofer, M., & Berggren, A. M. (2006). Wrist-bridging versus non-bridging external fixation for displaced distal radius fractures: a randomized assessor-blind clinical trial of 38 patients followed for 1 year. Acta orthopaedica, 77(3), 445-453. Retrieved from: http://informahealthcare.com/doi/pdf/10.1080/17453670610046389 Blakeney, W. G. (2010). Stabilization and treatment of Colles’ fractures in elderly patients. Clinical interventions in aging, 5, 337. Retrieved from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3010169/
Dionyssiotis, Y., Dontas, I. A., Economopoulos, D., & Lyritis, G. P. (2008). Rehabilitation after falls and fractures. J Musculoskelet Neuronal Interact, 8(3), 244-250. Retrieved from: http://www.ismni.org/jmni/pdf/33/05DIONYSSIOTIS.pdf
Drozd, M., Miles, S., & Davies, J. (2009). Casting: Below-elbow back slabs. Emergency Nurse, 17(5), 20-2. Retrieved from http://0-search.proquest.com.alpha2.latrobe.edu.au/docview/218300051?accountid=12001
Gupta, A. (1991). The treatment of Colles' fracture. Immobilisation with the wrist dorsiflexed. Journal of Bone & Joint Surgery, British Volume, 73(2), 312-315. Retrieved from:http://www.bjj.boneandjoint.org.uk/content/73-B/2/312.short
Khudairy ,A.A., Hirpara,K.M., Kelly,I.P. & Quinlan,J.K.(2013). Conservative treatment of the distal radius fracture using thermoplastic splint: pilot study results. Eur J Orthop Surg Traumatol (2013) 23:647–650. DOI 10.1007/s00590-012-1042-8
Lee, Y. S., Wei, T. Y., Cheng, Y. C., Hsu, T. L., & Huang, C. R. (2012). A comparative study of Colles’ fractures in patients between fifty and seventy years of age: percutaneous K-wiring versus volar locking plating. International orthopaedics, 36(4), 789-794. Doi: 10.1007/s00264-011-1424-2
Maire, N., Lebailly, F., Zemirline, A., Hariri, A., Facca, S., & Liverneaux, P. (2013). Prospective continuous study comparing intrafocal cross-pinning HK2® with a locking plate in distal radius fracture fixation. Chirurgie de la main, 32(1), 17-24. Retrieved from: http://0-www.sciencedirect.com.alpha2.latrobe.edu.au/science/article/pii/S1297320312003253?via=ihub
Nieves, J. W., PhD., Mosner, M., R.D., & Silverstein, S., M.S.N. (2012). Osteoporosis. New York State Dental Journal, 78(4), 30-5. Retrieved from http://0-search.proquest.com.alpha2.latrobe.edu.au/docview/1112539521?accountid=12001
Nguyen T, Sambrook P, Kelley P, Jones G, Lord S, Freund J, Eisman J 1993 Prediction of osteoporosis fractures by postural instability and bone density. British Medical Journal 307:1111-1115. Retrieved from: http://www.jstor.org/stable/29721550
O’connor, D., Mullett, H., Doyle, M., Mofidi, A., Kutty, S., & O’SULLIVAN, M. (2003). Minimally displaced Colles’ fractures: a prospective randomized trial of treatment with a wrist splint or a plaster cast. Journal of Hand Surgery (British and European Volume), 28(1), 50-53. doi: 10.1054/JHSB.2002.0864
Salvi, A. E. (2011). The handshake technique: proposal of a closed manual reduction technique for Colles’ wrist fracture. The American journal of emergency medicine, 29(1), 115-117. Retreieved from: http://0-search.proquest.com.alpha2.latrobe.edu.au/nursing/docview/1030934863/C8FC546DF4214530PQ/7?accountid=12001
Sànchez-Riera, L., Wilson, N., Kamalaraj, N., Nolla, J. M., Kok, C., Li, Y., ... & March, L. (2010). Osteoporosis and fragility fractures. Best practice & research Clinical rheumatology, 24(6), 793-810. Retrieved from: http://www.sciencedirect.com/science/article/pii/S1521694210000896
Summers, A. (2005). Recognising and treating colles' type fractures in emergency care settings. Emergency Nurse, 13(6), 26-33; quiz 34. Retrieved from http://0-search.proquest.com.alpha2.latrobe.edu.au/docview/218283455?accountid=12001
Turner, R. G., Faber, K. J., & Athwal, G. S. (2007). Complications of distal radius fractures. Orthopedic Clinics of North America, 38(2), 217-228.Retrieved from: http://www.sciencedirect.com/science/article/pii/S0030589807000053 Wik, T. S., Aurstad, Å. T., & Finsen, V. (2009). Colles’ fracture: Dorsal splint or complete cast during the first 10 days?. Injury, 40(4), 400-404.Retrieved from: http://0-www.sciencedirect.com.alpha2.latrobe.edu.au/science/article/pii/S0020138308003628?via=ihub
Functional Aims and Goals
[edit | edit source]The functional goals for this brace are to immobilise the movements of flexion/extension and radial/ulnar deviation at the wrist joint, while still allowing full movement of flexion and extension at the interphalangeal and metacarpophanlangeal joints. The keyhole wrist and hand brace that was prescribed should also provide comfort, decrease the pain, protect the injured structure from further damage and reduce the risk of the aligned distal radius displacing (Uustal& Baerga, 2004). In this case, a lightweight thermoplastic device is preferential over a heavier plaster of paris cast as it allows for optimal healing to occur, can be removed for hygiene practices and is tolerated more by clients (O’Connor et al, 2003). The 3 point force system applied using straps, will help to keep the wrist in the correct position, around 20 degrees of wrist extension with slight ulnar deviation and will also provide more stabilization.
The POP cast that had been made previously included the same positioning and would use the same suspension type if it had been applied. This cast is heavier though, due to the large amount of layers needed to provide support and shouldn’t be used for longer than the initial period of 1-2 weeks after the fracture. This will allow swelling to reduce before the long term LTT device is applied.
Design
[edit | edit source]The use of this orthosis is designed to immobilize and promote tissue healing in the correct alignment at the fracture, in this case at the distal end of the radius (Blakeney, 2010). For this type of fracture, there are many differing opinions and reviews on what position the wrist should be placed in when casting. As a result there is no one definitive treatment, so a slightly extended wrist position was chosen. The medial and lateral trim lines of the device should have a circumference covering half the side of the forearm. The length should be 2/3 the length of the forearm and the distal palmar crease becomes the distal trim line of the device. the proximal end should be flared out so as not pinch the skin underneath. The force diagram can be seen below.

3 straps are attached onto the device; these provide the suspension for the brace. One strap should be at the on the dorsal surface of the forearm at the proximal end of the device, one strap should cover the ulnar styloid process and the other is placed on the dorsal surface of the hand, just below the MCP joints of the 4 digits.
Manufacturing process
[edit | edit source]Materials needed: kitchen chux, permanent marker, paper towel, a sheet of low temperature thermoplastic, table, chair, goniometer, scissors, sheers electric frypan, water, towel, stick back Velcro hooks and Velcro loops.
Step1: The patients hand and arm was placed on to a piece of paper towel, marking the anatomical landmarks of the distal palmar crease, the wrist joint and the MCP joint of the thumb. A line was drawn vertically from the second digit to meet with a line coming across from the MCP joint of the thumb. This was then drawn into a circle, for the thumb hole of the device.
Step 2: The initial design is then cut out and placed on the client’s wrist with the wrist in position (about 10⁰ of extension and slight ulnar deviation) to check if any changes need to be made. Step 3: The design is then traced onto a piece of kitchen chux and then onto a sheet of low temperature thermoplastic (LTT) and cut out.
Step 4: The LTT should be placed in the electric frypan with the water around 60⁰c to begin softening. While this is happening, the patient’s wrist should be put into position and the angle of the wrist double checked using the goniometer.
Step 5: Once the LTT has softened enough, it’s taken out and the edges on the distal transverse crease and around the thumb should be rolled back
Step 6: The LTT is then placed back into the water to soften once more and when taken out it is draped over the patient’s wrist and aligned into the correct position. Once the LTT is aligned, it needs to be secured by folding it over the arm and pinching the edges together. The orthosis was then moulded to the patients forearm.
Step 7: Before removing the device, trim lines should be drawn on so that correct changes can be mad. Once the LTT has cooled down in the correct position, it can be removed from the patients arm
Step 8: Before the orthosis fully cools down, trim lines can be cut along the lines previously made and excess material removed. The proximal end of the device can then be flared out. Step 9: Stick back Velcro hooks and loops are measured and cut. The adhesive Velcro is trimmed down and the corners are rounded for an aesthetically pleasing look.
Step 10: The stick back Velcro hooks are placed on to the device and a heat gun is used to heat the device and permanent straps so that they stay in place.
Step 11: The device can then be fitted to the patient and the straps can be checked for the right positioning. Last minute changes can be made if necessary.
-
step 1
-
step 3
-
step 4
-
step 5
-
step 6
-
step 8
-
step 10
-
step 11
-
step 12
Critique of fit
[edit | edit source]The client is a 65 year old retired female who suffered a colles’ fracture on her right arm following a fall onto outstretched hands. She has recently been diagnosed with osteoporosis. On presentation, the client reported a high level of pain and swelling and slight bruising around the site of the injury were observed. The injury was classified as a 23-A2 fracture according to the Muller AO Classification system, a closed transverse fracture with a minimally displaced distal fragment. No surgery was required and it was deemed appropriate for conservative treatment. It was placed in a POP cast initially, to let the swelling reduce before a volar wrist splint was applied. The referring doctor requested an immobilization device be worn for 6 weeks. The client’s main goal consisted of having the functionality of her wrist back, in time for a CWA function in 10 weeks’ time. The main goal of orthotic management was to immobilize the fracture and allow healing to occur in the proper alignment. The device should also provide comfort, decrease the pain level and protect the distal radius from any further damage. In order to achieve these goals, a custom made, low temperature thermoplastic (LTT) keyhole wrist orthosis was provided. The choice of LTT is lighter than a plaster of paris cast and can be removed to help with hygiene practices. The problem with that is that it could cause a problem with compliance (O’Connor et al, 2003). The device met the prescription design and fit the client well. The 3 point force system is applied in the sagittal plane through the use of 3 straps. The client reports that the device is comfortable and practical and states that she feels no pressure areas under the device and doesn’t experience any chaffing under the straps. Overall, the device is manufactured at an acceptable level, however there were some areas that could have been improved.
- The distal trim line comes down slightly too low. They should be just underneath the distal transverse creases, however there is a slightly bigger gap. This could have been a result of rolling down the edges of the device too much.

- Some marks where the trim lines were drawn are still visible on the device

- Slight ulnar deviation isn’t achieved. Next time I would ensure that the client stayed in the correct position and would keep monitoring the angles until the thermoplastic was fully cooled.
- There is a small gap between the palmar surface of the hand and the device, however this doesn’t affect any of the goals of the device, no movement is available

- There is a slight wave in the thermoplastic on the medial trim line. This could have occurred during the moulding stage, by not conforming the thermoplastic completely to the medial side of the arm

Following 6 weeks in the cast, 2 outcome measures; the DASH questionnaire and level of pain (on a numerical scale) could be completed. The Dash questionnaire includes questions about symptoms and the ability to perform certain activities. It would be expected that the level of pain in the client now is much less or non-existent than when compared to her level of pain when she first presented to the clinic.
Outcome measures
[edit | edit source]Outcome measures are tools used to assess different aspects of injuries, including symptoms, pain, ability to perform daily living activities and function of the limb. They enable health professionals to engage more in the recovery, rehabilitation and return to work of a person injured.
For this client, 3 outcome measures were assessed; DASH, range of motion testing and pain using a visual analogue scale. The DASH questionnaire asks patients about their symptoms and their ability to perform certain activities. The patient scored 15 on this assessment. The results to the survey are measured by considering the score as a number out of 100, the higher the number, the greater the impact of the disability. The optional modules were not undertaken for this client and Nancy’s score of 15, indicated that after her injury was allowed to heal, there was only a mild interference in her daily life. Alternatively, the “QuickDash” survey can be used, however it doesn’t provide as much feedback.
Prior to her fracture, Nancy reported no limitations in range of motion at the wrist joint. After 6 weeks of wearing her LTT brace, ROM was tested. Normal values for active flexion extension are 80˚ and 70˚ respectively. It was expected that Nancy would have some limitations with these movements and this was seen with the values achieved; 62˚ for flexion and 50˚ for extension. The level of pain that Nancy experienced was noted down on her arrival to the emergency department and also after the duration of her time in the LTT brace. Pain was measured using a numerical rating scale, like the one below. Originally Nancy noted her pain as a 7 on the scale, after treatment this went down to a 0.