Upper Limb Orthotics/Brachial Plexus Birth Palsy
Describe your case study
[edit | edit source]The patient is a 2 month old female who had a forceps delivery. The patient has Erb-Ducheene palsy affecting the right upperlimb. The patient’s right upper limb had a typical “waiter tip position” on initial presentation at the age of 2 weeks, the shoulder adducted and internaly rotatedelbow extended and pronated and flexed wrist and fingers. At the age of 2 months the patient can achieve 90° of active shoulder flexion however the elbow remains extended and pronated with a flexed wrist. The patient is continuing to receive daily physical therapy and was receiving kineseo taping treatment but has had an adverse skin reaction to the adhesive. Parent is concerned about possible wrist contractures.
Orthotic Treatment of Erb’s Palsy in the Upper Limb
[edit | edit source]Introduction
[edit | edit source]Erb-Duchenne palsy (Erb’s palsy) is the most common obstetric brachial plexus palsy, and can be managed both conservatively and surgically (O’Brien, Park, Noetzel, and Weatherly, 2006). This paper will explore the orthotic treatment of Erb’s palsy in the upper limb. Firstly a basic, anatomical understanding of Erb’s palsy will be established. Then, a number of orthotic devices that can be used as part of a conservative treatment plan, as well as post surgically will be presented and finally compared.
Cause
[edit | edit source]Erb’s palsy is a nerve injury to the upper roots of the brachial plexus: C5 and or C6 (Chater, Camfield, and Camfield, 2004; Srilakshmi, and Chaganti, 2013). The most common mechanism of injury is birth trauma caused by excessive bending or stretching of the infants’ neck during childbirth (O’Brien, et al., 2006), often as a result of a forceps delivery (Srilakshmi, and Chaganti, 2013 ). There are four types of nerve injury that may occur, varying in severity from stetching to complete detachment of the nerve. Neuropraxia is the most minor injury, caused by stretching; the injury typically heals on its own. Rupture is where the nerve has been torn but not completely severed, often requiring surgery to regain full function. Surgery is also required in the case of a neuroma, where scar tissue is preventing transmission along the nerve. Where as the most serious injury, avulsion, results in a complete detachment of the nerve, which cannot be surgically repaired and usually results in a permanent loss of function (Ruchelsman, Pettrone, Price, and Grossman, 2008). It is common for a combination of these injury types of varying severities to be present in a single case (Gherman, Chauhan, Oh, and Goodwin, 2005). As a result the severity of nerve injury in each case of Erb’s palsy varies greatly.
Anatomy
[edit | edit source]Nerve damage to the upper roots can cause muscle weakness or paralysis, as well as sensory loss (O’Brien, et al., 2006). The upper roots of the brachial plexus innervate the deltoids, supraspinatus, infraspinatus, biceps, brachioradialis, supinators, wrist extensors and finger extensors (Chater, et al., 2004; Gherman, et al., 2005). Resultantly, an infant with Erb’s palsy typically presents with an adducted and internally rotated shoulder, an extended elbow, pronated forearm and flexed wrist and fingers (Ruchelsman, et al., 2008). Sensory loss may also be evident on the lateral upper arm and lateral forearm, corresponding to injury affecting the axillary and musculocutaneous nerves respectively (Chater, et al., 2004).
Orthotic treatment options
[edit | edit source]The treatment pathway for Erb’s palsy commonly begins conservatively. Conservative treatment consists of occupational therapy, comprising largely of passive and active range of motion exercises (Ramos, and Zell 2000). Occupational therapy is complemented with orthotic treatment, as required throughout the rehabilitation process. The main purpose of orthotic use, in this instance is to prevent contractures in the wrist and fingers and to assist in movement where muscle weakness is present (Ruchelsman, et al., 2008). Both static and dynamic orthoses may be used and in some cases concurrently (Ruchelsman, et al., 2008). It is likely that the patient will use more than one type of orthoses during the rehabilitation process, as functional goals for the orthotic device will evolve as the patient grows and improves upper limb function.
Low temperature wrist hand orthosis
[edit | edit source]Low temperature wrist hand orthoses (WHO) are one type of orthotic intervention that may be utilised. WHO are often used to prevent wrist and finger contractures by maintaining the wrist and fingers in an extended position (Chater, et al., 2004; Zafeiriou, and Psychogiou, 2008). WHO used for Erb’s palsy patients are typically static devices, as a result they can reduce functionality of the hand and are commonly prescribed as night splints (Ruchelsman, et al., 2008), although more functional designs do exist. The largest issue with WHO is as the infant gets older they learn how to remove the device, and the tolerance of the device decreases. WHO can be custom made or bought prefabricated and it is also important consideration the construction of the device to prevent injury.
Supinator orthoses and taping
[edit | edit source]Supinator straps made of soft fabric used in conjunction with fabric WHO are dynamic devices that can be used to correct forearm pronation and encourage supination. While in some infants the device is not well tolerated for similar reasons to the WHO, the device has been shown to encourage muscle movement, unlike a static WHO (Chater, et al., 2004). Alternatively Kinesio arm taping can be used in a similar fashion, to increase forearm supination as well as wrist and finger extension (ElKhatib, ElNegmy, Salem, & Sherief, 2013). Research has shown that infants who receive Kinesio taping as part of a conservative treatment plan, recover faster than those who did not receive the Kinesio treatment (ElKhatib, et al., 2013).
Elbow flexion orthoses
[edit | edit source]Elbow flexion orthoses are sometimes used to treat elbow flexion contractures. Elbow flexion contractures are common in older children with Erb’s paly who still suffer from minor functional limitations (Sheffler, Lattanza, Sison-Williamson, and James, 2012). The elbow flexion orthoses operates in a similar was to serial casting, with the angle of elbow flection increasing every few days. Elbow flexion orthoses can be purchased prefabricated or be custom made. Wrist and hand aspects can also be added to the device to counteract wrist and hand contractures as well.
Evidence for orthotic treatment
[edit | edit source]Despite the wide acceptance as best practice and resultant implementation of orthotic use as part of a conservative treatment plan for Erb’s palsy, there is insufficient evidence in the literature to suggest orthotic intervention is effective (Bialocerkowski, Kurlowicz, Vladusic, and Grimmer, 2005; Chater, et al., 2004). Currently no randomised trials have been undertaken on the effectiveness of orthotic treatment in obstetric brachial plexus palsies, and of the minimal literature that is available it is inconclusive and of low validity (Bialocerkowski, et al., 2005). Despite the gap in the literature, the current conservative treatments are supported by more general literature on treating contractures in children (Teplicky, Law, and Russell, 2002). However it is evident that a significant amount of research needs to be undertaken in this area.
Surgery
[edit | edit source]The treatment pathway for Erb’s palsy commonly begins conservatively, if no or limited improvement in function is seen at 3 months of age, surgical options are then explored (Miller, Allgier, and Louden, 2013). Surgical options include microsurgical reconstruction, nerve graphs and nerve transfers. Surgery often begins with an exploration of the brachial plexus to determine the types and locations of nerve injuries. X-rays and magnetic resonance imaging are also used pre-surgery to identify any underlying fractures and avulsion injuries. If a neuroma is identified nerve reconstruction in the form of a nerve grafts is typically undertaken, where as an avulsion injury may require a nerve transfer as well as nerve grafts (Miller, et al., 2013). More complex nerve injuries typically require further surgical procedures as well as achieve a lower overall function than those with simpler injuries (Ruchelsman, et al., 2008).
Post surgery orthoses
[edit | edit source]The type of orthotic intervention prescribed post surgery, if any, is largely dependent on the severity of the case, age of the child and the type of surgery being undertaken. The general purpose of a post surgery orthoses is to promote healing in the optimal position and to improve movement functionality (Parent-Weiss, Weiss, and Jebson, 2005). One of the most common used devices post surgery, is a shoulder abduction-rotation orthoses (SARO). When using a SARO the child’s shoulder is held in abduction with the elbow in flexion, secured in place by an attachment to the torso (Parent-Weiss, et al., 2005). The angles of shoulder abduction and elbow flexion are altered to accommodate the child’s functional limitations. Historically this device has been custom made prior to surgery, however prefabricated versions are now available. Plaster casts are also an alternative used on occasion, but do not provide the adjustability of a custom or prefabricated device.
Comparison of conservative and surgical orthotic treatments
[edit | edit source]Orthoses, in both the conservative and surgical treatment plans are primarily used to treat secondary conditions: preventing contracture and immobilisation after surgery. All orthotic types discussed each have different functional goals. Therefore it is important to ensure that the correct orthosis is utilised in the correct situation. While there are anecdotally different methods of taping and different designs for WHO and SARO, literature does not discuss the most effective strategy in producing customised orthoses or selecting the most appropriate prefabricated device. As a result clinicians may make decisions based on personal experience or preference rather than what is the most effective. Further research into orthotic design to determine the most effective design strategy for each functional out come would be desirable
Conclusion
[edit | edit source]Regardless if a conservative intervention was used exclusively or in conjunction with surgical treatment, 80%-96% of Erb’s palsy cases are resolved after the first 12 months of life (Chater, et al., 2004). While there is currently no definitive clinical evidence to suggest that the use of orthoses in conjunction with occupational therapy is beneficial in preventing contracture and improving movement function, the treatment option is producing satisfactory results. Therefore until further research can be undertaken this method should be considered as best practice. While there is also no literature that specifically looks at the effectiveness of post surgery orthoses, the current practice is again anecdotally effective and should be continued until further research is completed. In conclusion, provided the chosen orthosis’ functions match the desired outcome of device use, all orthotic interventions outlined would be a satisfactory options. No one orthotic intervention has been clinically proven to be more effective or beneficial than any other.
Search strategy
[edit | edit source]The following databases were used: Medline, CINHAL, Cochrane The following key words were used in varying combination of AND an OR: erb’s palsy, brachial plexus birth pas*, obstetric* brachial plexus injury, splint*, orthos*, surgery, intervention.
References
[edit | edit source]Bialocerkowski, A., Kurlowicz, K., Vladusic, S., & Grimmer, K. (2005). Effectiveness of primary conservative management for infants with obstetric brachial plexus palsy. International Journal of Evidence‐Based Healthcare, 3(2), 27-44. doi: 10.1111/j.1479-6988.2005.00020.x
Chater, M., Camfield, P., & Camfield, C. (2004). Erb’s palsy–Who is to blame and what will happen?. Paediatrics & child health, 9(8), 556. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2724163/pdf/pch09556.pdf
ElKhatib, R. S., ElNegmy, E. H., Salem, A. H., & Sherief, A. A. (2013). Kinesio arm taping as prophylaxis against the development of Erb’s Engram. Journal of Advanced Research, 4(6), 485-491. Retrieved from http://www.sciencedirect.com/science/article/pii/S2090123212000641
Gherman, R. B., Chauhan, S., Oh, C., & Goodwin, T. M. (2005). Brachial plexus palsy. Fetal and Maternal Medicine Review, 16(03), 221-243. doi:10.1017/S096553950500152X
Miller, M., Allgier, A., & Louden, E. (2013). Restoring function for children with brachial plexus birth palsy. OR Nurse, 7(2) , 18-35. retrieved from: http://www.nursingcenter.com/lnc/cearticle?tid=1524955#sthash.rzLY2lE7.dpuf
O’Brien, D. F., Park, T. S., Noetzel, M. J., & Weatherly, T. (2006). Management of birth brachial plexus palsy. Child's Nervous System, 22(2), 103-112. doi: 10.1007/s00381-005-1261-y Ramos, L. E., & Zell, J. P. (2000). Rehabilitation program for children with brachial plexus and peripheral nerve injury. In Seminars in pediatric neurology (Vol. 7, No. 1, pp. 52-57). WB Saunders. Retrieved from http://0-www.sciencedirect.com.alpha2.latrobe.edu.au/science/article/pii/S1071909100800108?via=ihub# Ruchelsman, D. E., Pettrone, S., Price, A. E., & Grossman, J. A. (2008). Brachial plexus birth palsy: an overview of early treatment considerations. Bulletin of the NYU hospital for joint diseases, 67(1), 83-89. http://0-web.b.ebscohost.com.alpha2.latrobe.edu.au/ehost/pdfviewer/pdfviewer?sid=37d6c644-d5a0-4d31-b021-aa7795d182f0%40sessionmgr114&vid=2&hid=125
Sheffler, L. C., Lattanza, L., Sison-Williamson, M., & James, M. A. (2012). Biceps Brachii Long Head Overactivity Associated with Elbow Flexion Contracture in Brachial Plexus Birth Palsy. The Journal of Bone & Joint Surgery, 94(4), 289-297. doi: 10.2106/JBJS.J.01348
Srilakshmi, D., & Chaganti, S. (2013). A holistic approach to the management of Erb's palsy. Journal of Ayurveda and integrative medicine, 4(4), 237. doi 10.4103/0975-9476.123713
Teplicky, R., Law, M., & Russell, D. (2002). The effectiveness of casts, orthoses, and splints for children with neurological disorders. Infants & Young Children, 15(1), 42-50. Retrieved from http://0-ovidsp.tx.ovid.com.alpha2.latrobe.edu.au/sp-3.11.0a/ovidweb.cgi?WebLinkFrameset=1&S=MFLEFPKMJMDDMMIONCMKAAIBHAILAA00&returnUrl=ovidweb.cgi%3f%26Full%2bText%3dL%257cS.sh.30.31%257c0%257c00001163-200207000-00007%26S%3dMFLEFPKMJMDDMMIONCMKAAIBHAILAA00&directlink=http%3a%2f%2fgraphics.tx.ovid.com%2fovftpdfs%2fFPDDNCIBAAIOJM00%2ffs025%2fovft%2flive%2fgv015%2f00001163%2f00001163-200207000-00007.pdf&filename=The+Effectiveness+of+Casts%2c+Orthoses%2c+and+Splints+for+Children+with+Neurological+Disorders.&pdf_key=FPDDNCIBAAIOJM00&pdf_index=/fs025/ovft/live/gv015/00001163/00001163-200207000-00007
Parent-Weiss, N. M., Weiss, D. B., & Jebson, P. J. (2005). Custom Shoulder Abduction/Rotation Orthosis in Postoperative Management of Brachial Plexus Injury After Modified L’Episcopo Procedure. JPO: Journal of Prosthetics and Orthotics, 17(3), 68-73. Retrieved from http://www.oandp.org/jpo/library/2005_03_068.asp
Zafeiriou, D. I., & Psychogiou, K. (2008). Obstetrical brachial plexus palsy. Pediatric neurology, 38(4), 235-242. doi 10.1016/j.pediatrneurol.2007.09.013
Functional Aims and Goals
[edit | edit source]The functional aim for this device is to prevent wrist and hand contractures. This is achieved through the fabrication of a night splint that immobilizes the wrist and fingers in an extended position. As the device is to be worn as a night splint and also considering the age of the client, functional movement of the wrist and hand is not required. As the elbow is predominately in an extended position, it is important that the proximal trimlines allow for full range of motion at the elbow, as not to discourage elbow flexion. The device is also able to correct the position of forearm pronation by molding the device with the forearm in a supinated position; ensuring the radiocarpal joint is completely immobilised.
Design
[edit | edit source]Correction:
- 3 point force system is used correct forearms pronation and wrist flexion, see figure 1
- resting orthosis design drawing see figure 2
Materials:
- low tempaerature thermoplastic
- piece of chucks for template
- 2cm and 4 cm Velcro hook and loop
- soft foam to be used as padding
Attachment Methods:
- Velcro hook to be adhered to LTT using dry heat
-
Caption1
-
Caption2
Manufacturing process
[edit | edit source]- draw, cut out and refine template on piece of chucks
- use template to cut out required piece of LTT
- heat LTT in hot water until it becomes pliable
- meanwhile position client in a seated position, with elbow resting on a table or arm rest, get client to extend fingers and have thumb pointing towards the clients nose
- remove LTT from hot water and dry on towel
- align LTT with clients forearm and wrist
- mold LTT to client achieving desired correction described in orthotic goals
- allow LTT to cool while in position
- check trimlines, remove device from client and remove any excess material
- check for sharp surfaces and remove by heating the surface and flatting out
- flare proximal end with heat gun
- measure and confirm strap position on client
- attach Velcro hook pieces to the device using a heat gun
- attach soft made over finger strap by cutting strips on either end of the pad and feed the strap through
- clean any markings
- attach straps
-
Caption1
-
Caption2
-
Caption1
-
Caption2
Critique of fit
[edit | edit source]Client: The client is a 2 month old female who presented with Erb’s palsy in her right upper limb with susceptibility to wrist and hand contracture at St Margret’s Hospital.
Subjective On presentation her parents reported the she hardly moved her right upper limb at all and has a very weak grip with her right hand.
Objective: A physical assessment was conducted and revealed:
- - right arm in “waiters tip” position with adducted and internally rotated shoulder, an extended elbow, pronated forearm and flexed wrist and fingers
- right arm lay limb by child’s side
- all joint could be manually manipulated to achieve normal range of motion
- no voluntary movement of shoulder , elbow or wrist
- absent moro reflex
Diagnosis: Considering the results, the child’s diagnosis of Erb’s palsy was confirmed.
Orthotic goals: The goal of orthotic management is to prevent wrist and finger contractures
Prescription: In order to achieve this goal a low temperature thermoplastic resting wrist hand orthosis has been prescribed. The orthosis is to contact the palmer surface of the hand and maintain wrist and finger extension.
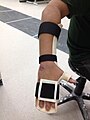
Device finish: Overall the finish of the device is good. There are some pen marks that couldn’t be removed. There are also some rougher edges due to stretching of the thermoplastic, the edges don’t pose a risk to the client but could be prevent by taking more care when moulding and stretching the plastic next time.
Device fit: Overall the device fits well . The distal trim line extends to fully support the fingers, the proximal trim line sits at two fingers width below the elbow crease, not to prevent elbow flexion. Straps are well positioned. Lateral and medial trimlines encompass the radial styloid and sit posterior to the ulna styloid respectively. There is a small amount of gaping along the proximal trimlines when the forearm slightly pronates, however fits well in forearm is supinated. Fore system to opposed wrist and finger flexion has been obtained. As the client is indeed a 26 year old male not an infant the thumb hole used to resist flexion may not be applicable for a 2 month old, due to the small size of the hand, perhaps an open thumb section with a strap would be more suitable.
Demonstrated use: The device meets the prescription goals, the fingers and wrist are held in a neutral position that resists their position of flexion. Elbow flexion can be obtained. As the device is worn as a night splint no other functionality is requires. Client is satisfied with device and finds in comfortable considering the devices goals.
-
Proximal Gap
-
Anterior Coronal View
-
Medial View
-
Posterior Coronal View
-
Thumb ROM
-
Medial Saggital View
Outcome measures
[edit | edit source]Outcome measures: Outcome measures in infants can be very difficult to undertake, as the child is not able to follow direction. The device is prescribed as a night split, that acts to immobilize and prevent contracture, and resultantly no functional movement is required. Therefore the most applicable outcome measure is to assess the general improvement of the upper limb as nerve function slowly restores. One of the best methods for testing and comparing upper limb movement in infants, is using the Active Movement Scale (AMS) (Curtis, Stephens, Clarke, and Andrews, 2002). The AMS grades the function of the joints in the upper limb using a grading system from 0-7. The method assesses the child’s movement based on observation in three different positions and under the influence of gravity and without (Curtis etal., 2002). As my actual client is an adult with normal range of motion conducting these outcome measure is not possible. However in a real clinical situation, as the nerve supply is slowly restored you would expect to see an increase in function and a higher grading score of all joints in the upper limb. At the very least you would expect the grades for wrist and hand to not to decline provided the device has been worn as prescribed, preventing contracture.
Reference: Curtis, C., Stephens, D., Clarke, H. M., & Andrews, D. (2002). The active movement scale: an evaluative tool for infants with obstetrical brachial plexus palsy. The Journal of hand surgery, 27(3), 470-478.