Motivation and emotion/Book/2010/Stress and health
| This page is part of the Motivation and emotion textbook. See also: Guidelines. |
What is stress?
[edit | edit source]
Imagine yourself in the following situation: It is the morning of an important exam, and you are feeling worried because you think that you aren’t quite prepared. You get into your car, but have trouble starting the engine. You crank the motor again and again without any luck. Finally, the motor roars into life and you are on your way to university. You are already running a little late, but think that you can still make it to your exam on time if you drive a little faster than you probably should – until you turn onto the main road to the university to find that traffic is at a standstill. Now, think of the different physical sensations and emotions you would be feeling in the aforementioned situation. You would probably feeling anxious and worried, your heart would be racing, you would be sweating, your stomach would be turning and you would suddenly feel highly alert. These are all symptoms of the stress response. Life is inherently stressful and almost every person experiences stress at some stage in their life.
Stress is a non-specific emotional and physiological response to demands in the environment, both positive and negative (Baum & Posluszny, 1999). In an evolutionary context, stress is an extremely important defensive reaction, activating the ‘fight or flight’ response – a process by which the body prepares to either face or run away from danger. The stress response is a multifaceted process that occurs when individuals are faced with stressors (stimuli that elicit stress) and involves both psychological and physiological elements.
The stress response
[edit | edit source]The stress response is an automatic physical and emotional response to stimuli that is perceived to be a threat to safety. Unconsciously, the cerebral cortex alerts the hypothalamus and the pituitary gland,which send signals to the adrenal cortex via the peripheral nervous system to release epinephrine and norepinephrine into the blood stream. Simultaneously, the pituitary gland sends signals to the adrenal cortex via adrenocorticotropic hormone (ACTH) that is released into the blood. ACTH stimulates the adrenal glands to secrete mineralocorticoids and glucocorticoids (Marieb & Hoehn, 2007; Myers, 2007). These hormones affect a number of organs and systems in the body to produce the following symptoms:
- Increased heart rate
- Increased blood pressure
- Increase blood-sugar concentration
- Widening of the arteries
- Diversion of blood away from stomach
- Increased blood flow to skeletal muscles
- Increased muscle tension and strength
(Myers; Marieb & Hoehn)
The stress response also induces an emotional and cognitive reaction from the individual. Many emotions are elicited during the stress response such as anger, fear, anxiety or depressed mood (Baum & Posluszny, 1999). Cognitive function is also enhanced during the stress response, as mental alertness is heightened (Myers, 2007). All of these elements prepare the organism to either confront or run from the perceived danger.
Theories of Stress
[edit | edit source]General Adaptation Syndrome (Selye)
[edit | edit source]
In 1950, Hans Selye published his theory explaining the mechanisms of stress – General Adaptation Syndrome (GAS) - in the British Medical Journal. This theory is still highly influential today in medical research. According to GAS, the response that every organism shows to stress is the same, regardless of the organism or the stressor that induces the reaction (Selye, 1950). In the GAS model, there are three stages to the stress response: the alarm reaction, resistance and exhaustion (see Figure 1).
- The Alarm Reaction – In this stage, the stressor is identified by the organism and the stress response rapidly occurs. Initially, the ability to resist the stressor is diminished, due to the physiological effects caused by the activation of the sympathetic nervous system (such as increased heart rate and diversion of blood away from organs such as the stomach to the skeletal muscles) (Myers, 2007). However, the body quickly adjusts and moves into stage two, resistance (Selye, 1950).
- Resistance – During this stage, the body deals with the stressor by increasing heart rate and blood pressure, increasing energy available to the skeletal muscles and heightening alertness temporarily (Marieb & Hoehn, 2007). This response is only designed to be sustained for a short period of time, after which stage 3 occurs (Selye, 1950).
- Exhaustion – In stage 3 of GAS, if the presence of the stressor is sustained, the body’s resources become depleted and the body can no longer sustain an appropriate level of resistance to the stressor. The ability of the body to deal with the stressor becomes lower than it was prior to the stress response, which can leave the organism vulnerable to injury or disease (Myers, 2007; Selye, 1950).
Whilst this model is widely accepted by the medical community as an appropriate conceptualisation of the stress response, Selye did not make any firm distinction between the different type of stressors and did not take into account individual differences in the way people perceive stressors (Lazarus, 1993). In this model, both psychological and physiological stressors are treated in the same way; that is, a stressor is defined as anything that is potentially damaging to tissue (Lazarus, 1993). However, in reality, individual perceptions on what is a threat and what is harmful vary largely between different people (McCraty & Tomasino, 2006). In reaction to this, research moved in the direction of explaining the psychological (particularly, the emotional and cognitive) component of the stress response.
Cognitive Appraisal Theory (Lazarus)
[edit | edit source]
The cognitive appraisal theory looks to address some of the deficits of the GAS theory and centres around the concept that it is the organism's perception and appraisal of the stressor that is the most important factor in the intensity of the stress response. This theory suggests that the stress response can be mediated by the individuals appraisal of the stressor as either a threat or a challenge (Larazus, 1990). Depending on whether the stressor is considered a threat to safety or positive challenge, the body’s reaction will differ. If the stressor is appraised to be a challenge, the stress response will be diminished and the experience will be more positive than if the stressor is perceived as a threat (which would induce the ‘typical’ stress response, defined by GAS) (Lazarus, 1993). Lazarus (1990) argues that the stress response is just one part of a larger process that is driven by cognition. This theory has been received favourably given that it takes into account the large psychological component of stress and how individual experience plays a role in the perception of stressors (Ursin & Eriksen, 2001). This theory also have implications for the management of stress, which is discussed later in this chapter.
Relationship between Stress and Health
[edit | edit source]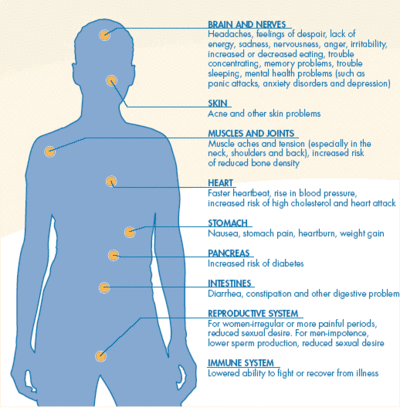
Stress is one of the most important factors that mediates the relationship between health and behaviour (Baum & Posluszny, 1999). It is widely regarded as one of the most important factors in illness (Hanson & Chen, 2010) and is fast becoming a major public health problem (Gehling, Aubert, Padlina, Martin-Diener & Somaini, 2001). Acute stress can be beneficial for an organism, triggering the ‘fight or flight’ response and thereby increasing strength, stamina and attention for a short period of time (Ekman & Arnetz, 2006). However, chronic stress is disruptive to a multitude of psychological and physiological processes.
Over time, if the stress response system is activated continuously, the allostatic load caused by this can put strain on the body (Hanson & Chen, 2010). The ‘exhaustion’ stage of Selye’s GAS theory states that prolonging and sustaining the physiological and psychological reactions of stress long-term has the potential to weaken the body’s immune responses through exhaustion, thereby predisposing the body to disease (Baum & Posluszny, 1999; Selye, 1950). In the long-term, the constant presence of stress hormones within the body results in a range of effects on the organs that create homeostatic imbalance. Mineralocorticoids cause the retention of water and sodium in the body by the kidneys, which increases blood volume and blood pressure. Glucocorticoids increase the amount of glucose in the blood by suppressing insulin and increasing the conversion of fat to glucose (Marieb & Hoehn, 2007). Both of these processes put strain on the cardiovascular and immune systems, as both of these systems use the blood to transport oxygen, antibodies, immune cells and nutrients to cells as well as transporting waste and infection away from cells.
The psychological impacts of stress also play a role in health outcomes. Research has shown that individuals who are under chronic stress are more likely to engage in unhealthy behaviours such as excessive drinking, drug misuse, smoking, overeating and sedentary behaviour in order to manage and relieve the psychological discomfort of stress (Krueger & Chang, 2008). Increased alcohol and drug misuse has been strongly linked to stress in the research literature. The affect regulation model suggests that when stress increases, individuals 'self-medicate' with alcohol and drugs in order to reduce the feelings of distress and discomfort that come with stress (Grzywacz & Almeida, 2008). In their study into alcohol use, negative mood and stress, Grzywacz and Almeida found that the probability that a person would engage in binge drinking behaviours was largely increased on days when individuals experienced stress. Smokers also tend to report increasing their number of cigarettes they smoke during periods of high stress (Söderpalm & Söderpalm, 2006). Engaging in unhealthy behaviours long-term can result in a number of poor health outcomes such as cancer, obesity, health complications related to drug dependence or misuse and death (Krueger & Chang, 2008).
Chronic stress also leads to more instances of self-reported poor health and has been shown to be a large contributor to psychosomatic illness or pain (Ursin & Eriksen, 2007). Numerous studies have found that individuals who suffer from chronic stress report significantly poorer health than individuals who do not suffer chronic stress (Holmgren, Dahlin-Ivanoff, Björnlund & Hensing, 2009; Yu, Chiu, Lin, Wang & Chen, 2007). A study of Swiss participants found that not only did those who reported suffering chronic stress report more health complaints, the severity of the symptoms that they reported was significantly more likely to fall within a clinical range (Gehling, Aubert, Padlina, Martin-Diener & Somaini, 2001). Stress also appears to play a large role in the onset of psychosomatic illness, pain and medically unexplained health conditions. Sufferers of medically unexplained syndromes (such as chronic fatigue syndrome) often report that a stressful event preceded the onset of their condition (Rubin & Wessely, 2006).
Physiological Impacts of Stress
[edit | edit source]Cardiovascular
[edit | edit source]According to figures released by the Australian Bureau of Statistics, cardiovascular disease was the number one cause of death for both males and females in Australia during 2008 (ABS, 2010). Cardiovascular disease (CVD) is a blanket term used to describe a range of disorders that affect different components of the cardiovascular system including conditions such as myocardial infarction (heart attack), stroke, hypertension (high blood pressure), arrhythmia, aneurysm, thrombosis and oedema (Marieb & Hoehn, 2007). The associations between emotional states (such as stress) and cardiovascular disease have been well established over the last 20 years and have been shown to influence the development of cardiovascular pathology independent of other risk factors like smoking, weight and diet (Grippo & Johnson, 2009). So unsurprisingly, understanding the effects of stress on cardiovascular disease is becoming an important priority for medical science.

The relationship between stress (both acute and chronic) and CVD is well established, particularly in relation to myocardial infarction. Schnenck-Gustatsson (2009) found that stress was one of the most important risk factors in the development of CVD in women. In fact, stress is the primary cause of one type of myocardial infarction, called takotsubo cardiomyopathy, which only affects post-menopausal women (Ueyama, Kasamatsu, Hano, Tsuruo & Ishikura, 2008). This particular type of myocardial infarction was identified after an earthquake occurred in Japan, and the number of women suffering heart attacks increases dramatically (Ueyama, Kasamatsu, Hano, Tsuruo & Ishikura, 2008). As well as major life events, such natural disasters or periods of change and uncertainty, personality can influence stress, and it has been investigated in relation to CVD. During the 1980’s, type A personality was linked with CVD. Individuals with type A personalities tend to experience more stress due their propensity to be hostile and aggressive (Friedman & Booth-Kewley, 1987). However, research into type A personality and CVD was mixed and inconclusive, and the focus in recent years has shifted to other personality types that may be related to stress, such as type D 'depressive' personality (Pozuelo, Zhang, Franco, Tesar, Penn & Jiang, 2009; Denollot, 1998).
Given that a large portion of the changes that occur during the stress response are targeted at the components of the cardiovascular system such as the veins and arteries, it is unsurprising that over time, damage can also occur to these components of the cardiovascular system. High blood pressure (which is one of the primary symptoms of stress) when experienced over the long term, can weaken the walls of blood vessels and cause aneurysms to develop and rupture (Torii, Oshima, Kobayashi, Takagi & Tezduyar, 2007). Links have also been found between the presence of severe, acute stressors and the development of heart arrhythmias (Grippo & Johnson, 2009).
One theme that appears from the research literature into CVD and stress is that stress is an independent risk factor (given the pressure that the stress response directly puts on the cardiovascular system), but it also exacerbates other risk factors such as diet, smoking, levels of physical activity and weight. As mentioned previously, stress impacts the likelihood of a person engaging in unhealthy behaviours (Krueger & Chang, 2008). Learning to manage stress is one of the treatment strategies taught to CVD patients to help them manage their condition and reduce the likelihood of future illness (Grippo & Johnson, 2009).
Infectious Diseases
[edit | edit source]The situation experienced by the young woman in the case study, Jayne, is not uncommon for people who suffer chronic stress. Stress has a clear impact on the immune system and the wear-and-tear caused by stress can leave the body unable to mount a defense against incoming pathogens (Godbout & Glaser, 2006; Baum & Posluszny, 1999). Infectious diseases such as upper-respiratory infections, the 'flu, strains of herpes virus and hepatitis C have all been shown to spread faster in individuals experiencing chronic stress (Cohen, Janicki-Deverts & Miller, 2007).
The presence of chronic stress can increase the duration and severity of infectious diseases (Cohen, Janicki-Deverts & Miller, 2007). It has also been shown to help provide an environment within the body that promotes the activation and duplication of viruses and bacteria and is also being investigated as a potential cofactor in tumour growth and development (Godbout & Glaser, 2006). One of the hormones that is released during the stress response, glucocorticoid, has been implicated as the potential primary cause of immuno-suppression (Godbout & Glaser,). Once the immune system has been suppressed, viruses and bacteria that cause infectious diseases are more easily able to multiple and create infection within the body (Baum & Posluszny, 1999).
The emotional state that stress induces is also implicated in the increased propensity for those suffering chronic stress to also develop infectious diseases more rapidly (Clougherty & Kubzansky, 2009). The emotions associated with stress, such as depression and anxiety, has been shown to reduce the activity of key immune system cells such as natural killer cells and T- and B-cells (Godbout & Glaser, 2006).
The suppressed state of the immune system that chronic stress induces has large implications for the management and prevention of infectious diseases. Wound healing and surgical recovery has been shown to be greatly impacted if patients are in stressful environments. Godbout and Glaser (2006) found that wound healing was far slower under stressful conditions and the potential for the wound becoming infected was largely increased. The prevention of infectious diseases can be impaired by presence of chronic stress. When reading the case study, you may have asked yourself 'how it is that Jayne could have caught the flu and whooping cough, given that she had received vaccinations against those two viruses?'. Research shows that if Jayne received these inoculations whilst she was suffering chronic stress, they may not have worked. The antibody development process that occurs after being vaccinated can be impaired if the vaccine is administered whilst the recipient is under stress (Godbout & Glaser, 2006). B-cells play an essential role in the development of antibodies, and when the body is under psychological stress, the function of these cells is greatly reduced (Clougherty & Kubzansky, 2009).
Psychological Impacts of Stress
[edit | edit source]Depression
[edit | edit source]The stress response elicits a wide range of emotions, however, it is mainly responsible for producing a state of negative affect (Krueger & Chang, 2008). Stress is considered to be one of the primary risk factors for the ontset of major depressive disorder and episodes of sub-clinical depression (Husky, Mazure, Maciejewski & Swendsen, 2008). Husky et al. found that stress has a large influence on the development of an initial episode of depression, however tends to play a lesser role in every subsequent episode of depression. This finding is consistent with much of the research literature on the role of stress in depression. One study found that in the three to six months preceding the onset of depressive symptoms, 50 to 80% of depressed individuals reported experiencing at least one stressful life event (Cohen, Janicki-Deverts & Miller, 2007). The genetic predisposition to develop depression also appears to play a role in how individuals react to stressors. A recent study found that those with a family history of depression tended to report heightened negative affect in reaction to life stressors (Wichers et al., 2007). There appears to be an interplay between genetics, cognitive and environmental factors in the relationship between stress and depression.
No one type of stressor appears to have a greater influence on the development of depression than any other. In a study into the effects of work-place stress on mental health, Siegrist (2008) found that work-related stress was associated with a significantly increased risk of developing depression. Childbirth is also a highly stressful life event, and post-natal depression can develop during this period of high stress and rapid change. Interestingly, the stress of having a new baby appears to influence the development of depressive symptoms equally in both mothers and fathers (Gao, Chan & Mao, 2009).
However, Gao et al. (2009) found that mothers tended to be able to cope with the stress better, due to greater social support. The ability to cope with the stress appeared to mediate the level of depression that the mothers in Gao’s study suffered. Research, like the Gao et al. study, suggest that one of the factors that may contribute to the high prevalence of depressive disorders amongst adolescents and young adults may be their inability to cope with stress effectively. Sun, Tao, Hao and Wan (2010) found in a study of Chinese adolescents that the ability to cope with stressful life events reduced the likelihood of developing depression.
Post-traumatic Stress Disorder
[edit | edit source]
Post-traumatic stress disorder (PTSD) is arguably the one of the worst health outcomes that comes from exposure to stress. PTSD is a debilitating psychiatric condition that is triggered by a period of highly traumatic and stressful experiences that involved actual or threatened serious injury or death or the actual or threatened danger to personal integrity, either of the individual or others (Bisson, 2007). PTSD is most prevalent among males, and there is a high prevalence amongst veterans of war (Bisson, 2007; Stein, 2002). Following the stressful event, sufferers of PTSD experience severe and debilitating stress reactions whether or not they are in the presence of a stimuli that may remind them of the traumatic event (Yule, 1999). The stress reactions that sufferers experience when they experience flashbacks are linked with the development of depression and suicide attempts are common amongst those with PTSD who are of adolescent age and over (Yule, 1999). The neurological damage that is associated with long-term chronic stress (such as decreased hippocampus size, due to neuron atrophy) can be found in sufferers of PTSD (Stein, 2002).
Even though greater than 50% of adults have experienced at least one traumatic event during their life time, only approximately 10% of these individuals suffer from PTSD (Bisson, 2007). Exactly what makes one individual more susceptible to PTSD than another is still an area of debate in psychology. One model suggests that suffering a psychological disorder earlier in life increases the chance of developing PTSD after being exposed to a traumatising stressor (Cohen, Matar, Richter-Levin & Zohar, 2006). Debate about what biological mechanisms drive PTSD is also still up for debate, although dysfunction of the same hypothalamic-pituitary-adrenal axis that is activated in the normal stress response is returning promising results in an animal model (Cohen et al., 2006).
Preventative measures
[edit | edit source]Given the wide variety of health problems that are associated with stress, understanding how to manage stress in order to improve health is a high priority, particularly in developed nations (Gehring, Aubert, Padlina, Martin-Diener & Somaini, 2001). Thankfully, research is beginning to reveal that the effect of stress on health can be mediated by an individual's ability to cope with the stressor (Wang, Keown, Patten, Williams, Currie, Beck, Maxwell and El-Guebaly, 2009). According to the cognitive appraisal theory, it is the perception of the stressor that has the greatest impact on the level of stress produced (Lazarus, 1990), so learning strategies to help change the way an individual perceives everyday stressors (like the traffic jam from the start of the chapter) has a large impact on the levels of stress an individual experiences (Yu, Chiu, Lin, Wang & Chen, 2007). Like Jayne, many individuals use physical exercise as an effective method of reducing stress, although it can be difficult to get people who are stressed to engage in physical activity as sedentary behaviour can be highly rewarding over the short-term (Siegrist, 2008; Baum & Posluszny, 1999). Mediation has also been shown to be another effective method of stress reduction. In their study into CVD in an African-American population, Schneider and his colleagues found the use of transcendental mediation not only reduced stress, but in doing so, it significantly reduced the risk of CVD (Schneider, Alexander, Salerno, Rainforth & Nidich, 2005). Reducing stress can help improve self-reported health, as in the case of Jayne. Given the fact that the body is not designed to deal with chronic stress (Grippo & Johnson, 2009), making sure stress levels are managed is fast become an accepted method of controlling one of today's the largest public health issues.
Summary
[edit | edit source]Stress is an often unwelcome but common part of our lives and is widely recognised as one of the primary risk factors in health and illness (Hanson & Chen, 2010). This chapter has discussed the relationship between stress and health, looked in depth at four health conditions in which stress is a primary risk factor and discussed some of the preventative methods that can be used to reduce stress and thereby improve health. The two most prominent theories of stress - GAS and the Cognitive Appraisal theory - focus on different aspects of the stress response (the physiological and the psychological), but have both been shown to be quite useful in understanding the multifaceted nature of stress. The physiological features of the stress response impact heavily on the cardiovascular and immune systems, and the links between diseases of these systems and stress have been well established. Stress also has an impact of psychological well-being, with depression and post-traumatic stress disorder being the two psychiatric conditions which stress seems to exacerbate the worst. Thankfully, research has shown that the impact of stress on health can be moderated, in some cases, reversed, by learning coping strategies to effectively deal with stressors.
Quiz
References
[edit | edit source]Australian Bureau of Statistics. (2008). Causes of Death (cat.no. 3303.0). Retrieved from http://www.abs.gov.au/ausstats/abs@.nsf/Latestproducts/3303.0Main%20Features12008?opendocument&tabname=Summary&prodno=3303.0&issue=2008&num=&view=
Baum, A., & Posluszny, D. M. (1999). Health psychology: Mapping biobehavioral contributions to health and illness. Annual Review of Psychology, 50, 137-163. doi:10.1146/annurev.psych.50.1.137
Bisson, J. I. (2007). Post-traumatic stress disorder. Occupational Medicine, 57, 399-403. doi:doi:10.1093/occmed/kqm069
Clougherty, J. E., & Kubzansky, L. D. (2009). A Framework for Examining Social Stress and Susceptibility to Air Pollution in Respiratory Health. Environmental Health Perspectives, 117(9), 1351-1358. doi:10.1289/ehp.0900612
Cohen, S., Janicki-Deverts, D., & Miller, G. E. (2007). Psychological stress and disease. JAMA, 298(14), 1685-1687. doi:10.1001/jama.298.14.1685
Denollet, J. (1998). Personality and coronary heart disease: The type-D scale 16 (DS16). Ann Beh Med, 20(3), 209-215.
Ekman, R., & Arnetz, B.B. (2006). The brain in stress – Influence of environment and lifestyle on stress-related disease. In B. B. Arnetz, & R. Ekman (Eds.), Stress in Health and Disease (pp. 280-290). Weinheim: Wiley-VCH.
Friedman, H. S., & Booth-Kewley, S. (1987). Personality, type A behaviour and coronary heart disease: The role of emotional expression. Journal of Personality and Social Psychology, 53(4), 783-792.
Gao, L., Chan, S. W., & Mao, Q. (2009). Depression, perceived stress and social support among first-time Chinese mothers and fathers in the postpartum period. Research in Nursing and Health, 32, 50-58.
Gehring, T. M., Aubert, L., Padlina, O., Martin-Diener, E., & Somaini, B. (2001). Perceived stress and health-related outcomes in a Swiss population sample. Swiss Journal of Psychology/Schweizerische Zeitschrift Für Psychologie/Revue Suisse De Psychologie, 60(1), 27-34. doi:10.1024//1421-0185.60.1.27
Godbout, J. P., & Glaser, R. (2006). Stress-induced immune dysregulation: Implications for wound healing, infectious disease and cancer. J Neuroimmune Pharm, 1, 421-427. doi: 10.1007/s11481-006-9036-0
Grippo, A. J., & Johnson, A. K. (2009). Stress, depression and cardiovascular dysregulation: a review of neurobiological mechanisms and the integration of research from preclinical disease models. Stress (Amsterdam, Netherlands), 12(1), 1-21. Retrieved from http://ezproxy.canberra.edu.au/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=19116888&site=ehost-live
Grzywacz, J. G., & Almeida, D. M. (2008). Stress and binge drinking: A daily process examination of stressor pile-up and socioeconomic status in affect regulation. International Journal of Stress Management, 15(4), 364-380. doi:10.1037/a0013368
Hanson, M. D., & Chen, E. (2010). Daily stress, cortisol, and sleep: The moderating role of childhood psychosocial environments. Health Psychology, 29(4), 394-402. doi:10.1037/a0019879
Holmgren, K., Dahlin-Ivanoff, S., Björkelund, C., & Hensing, G. (2009). The prevalence of work-related stress and its association with self-perceived health and sick-leave, in a population of Swedish women. BMC Public Health, 9(73) doi:10.1186/1471-2458-9-73
Husky, M. M., Mazure, C. M., Maciejewski, P. K., & Swendsen, J. D. (2009). Past depression and gender interact to influence emotional reactivity to daily life stress. Cognitive Therapy and Research, 33(3), 264-271. doi:10.1007/s10608-008-9212-z
Krueger, P. M., & Chang, V. W. (2008). Being poor and coping with stress: Health behaviours and the risk of death. Am J Public Health, 98, 889-896. doi:doi:10.2105/AJPH.2007.114454
Lazarus, R. S. (1990). Theory-based stress management. Psychological Inquiry, 1(1), 3-13.
Lazarus, R. S. (1993). From psychological stress to the emotions: A history of changing outlooks. Annu. Rev. Psychol., 44, 1-21.
McCraty, R., & Tomasino, D. (2006). Emotional stress, positive emotions and psychophysiological coherence. In B. B. Arnetz, & R. Ekman (Eds.), Stress in Health and Disease (pp. 342-364). Weinheim: Wiley-VCH.
Myers, D. G. (2007). Psychology (8th ed.). New York, NY: Worth Publishers.
Pozuelo, L., Zhang, J., Franco, K., Tesar, G., Penn, M., & Jiang, W. (2009). Depression and heart disease: What do we know and where are we headed? Cleveland Clinical Journal of Medicine, 76(1), 59-70. doi: 10.3949/ccjm.75a.08011
Rubin, J., & Wessely, S. (2006). The role of stress in the etiology of medically unexplained syndromes. In B. B. Arnetz, & R. Ekman (Eds.), Stress in Health and Disease (pp. 292-305). Weinheim: Wiley-VCH.
Schneider, R. H., Alexander, C. N., Salerno, J., Rainforth, M., & Nidich, S. (2005). Stress Reduction in the Prevention and Treatment of Cardiovascular Disease in African Americans: A Review of Controlled Research on the Transcendental Meditation Program. Journal of Social Behavior & Personality, 17(1), 159-180. Retrieved from http://ezproxy.canberra.edu.au/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=aph&AN=17123964&site=ehost-live
Schnenck-Gustatsson, K. (2009). Risk factors for cardiovascular disease in women. Maturitas, 63(3), 186-190. doi: 10.1016/j.maturitas.2009.02.014
Selye, H. (1950). Stress and the general adaptation syndrome. The British Medical Journal, 1(4667), 1383-1392.
Siegrist, J. (2008). Chronic psychosocial stress at work and risk of depression: evidence from prospective studies. European Archives of Psychiatry & Clinical Neuroscience, 258, 115-119. doi:10.1007/s00406-008-5024-0
Söderpalm, B., & Söderpalm, A. (2006). The role of stress in the etiology of medically unexplained syndromes. In B. B. Arnetz, & R. Ekman (Eds.), Stress in Health and Disease (pp. 384-400). Weinheim: Wiley-VCH.
Stein, M. B. (2002). Taking aim at posttraumatic stress disorder: Understanding its nature and shooting down myths. The Canadian Journal of Psychiatry, 47(10), 921-922.
Sun, Y., Tao, F., Hao, J., & Wan, Y. (2010). The mediating effects of stress and coping on depression among adolescents in China. Journal of Child and Adolescent Psychiatric Nursing, 23(3), 173-180. doi: 10.1111/j.1744-6171.2010.00238.x
Torii, R., Oshima, M., Kobayashi, T., Takagi, K., & Tezduyar, T. E. (2007). Numerical investigation of the effect of hypertensive blood pressure on cerebral aneurysm - dependence of the effect on the aneurysm shape. Int. J. Numer. Meth. Fluids, 54, 995-1009. doi: 10.1002/fld.1497
Ueyama, T., Kasamatsu, K., Hano, T., Tsuruo, Y., & Ishikura, F. (2008). Catecholamines and estrogen are involved in the pathogenesis of emotional stress-induced acute heart attack. Stress, Neurotransmitters and Hormones: Ann. N.Y. Acad. Sci, 1148, 479-485. doi: 10.1196/annals.1410.079
Ursin, H., & Eriksen, H. (2007). Cognitive activation theory of stress, sensitization and common health problems. Ann. N.Y. Acad. Sci., 1113, 304-310. doi: 10.1196/annals.1391.024
Wang, J., Keown, L., Patten, S. B., Williams, J. A., Currie, S. R., Beck, C. A., Maxwell, C. J., & El-Guebaly, N. (2009). A population-based study on ways of dealing with daily stress: comparisons among individuals with mental disorders, with long-term general medical conditions and healthy people. Social Psychiatry and Psychiatric Epidemiology, 44(8), 666-674. Retrieved from http://ezproxy.canberra.edu.au/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=19039509&site=ehost-live
Wicher, M., Myin-Germeys, I., Jacobs, N., Peeters, F., Kenis, G., Derom, C., Vlientinck, P. D., & Vas Os, J. (2007). Genetic risk of depression and stress-induced negative affect in daily life. British Journal of Psychiatry, 191, 218-223. doi: 10.1192/bjp.bp.106.032201
Yu, L., Chiu, C., Lin, Y., Wang, H., & Chen, J. (2007). Testing a model of stress and health using meta-analytic path analysis. The Journal of Nursing Research: JNR, 15(3), 202-214. Retrieved from http://ezproxy.canberra.edu.au/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=17806037&site=ehost-live
Yule, W. (1999). Post-traumatic stress disorder. Arch Dis Child, 80(2), 107-109.

