Motivation and emotion/Book/2013/Blood donation
What motivates and what discourages blood donations?
Overview
[edit | edit source]
Blood is a priceless life sustaining fluid that no human could survive without. Blood is crucial to survival yet is quite often taken for granted until a tragic accident or illness occurs and it is desperately needed (Whittemore,2009). In March 2013 the population of Australia was estimated to be over 23 million people (ABS, 2013). Despite this large population it is estimated that only 3% of Australians actually donate (Australian Red Cross Blood Service, 2012) and less than 60% of new Australian blood donors return within the succeeding 2 years to make a further donation (Masser, White, Hyde, Terry, & Robinson, 2009). Even when donors are given rewards for donating Linden, Gregorio and Klaish (1988) found that of the 67% of men and 55% of women who were eligible to donate blood in the United States, only 8% actually did (Armitage, & Conner, 2001). Even though one donation can be used to save three lives, 27,000 blood donations are needed every week for routine, life-saving operations and for emergency medical care (Australian Red Cross Blood Service, 2013; Masser, et al., 2009). Moreover, is it forecast that the amount of blood needed will increase by 100% in the next 10 years (Australian Red Cross Blood Service, 2013). It is for these reasons and others that blood donation, retention and recruitment is such an important issue in Australia and around the world (Masser, et al., 2009). In order to increase the number of donors and to retain as many donors as possible, understanding blood donor motivation is crucial (Masser, et al., 2009). This chapter focuses on what motivates and discourages blood donations and how the theory of planned behaviour can be applied to encourage more people to donate.
Donating process
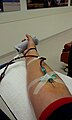
[edit | edit source]For those unfamiliar with the donating process here's a quick overview. The donor needs to prepare beforehand by drinking plenty of water and eating a substantial meal. To ensure the safety of the blood and the donor, they are given a short questionnaire about their health history then privately interviewed before every donation. The donation generally takes about 10 minutes for a whole blood donation, and about 45 minutes for either a plasma or platelet donation. After every donation the blood is tested for HIV 1 & 2, hepatitis B & C, HTLV I & II and syphilis. All equipment used is sterile and needles are only ever used once before being discarded. The Australian Red Cross Blood service ensures every donation is a very safe process. Below are photos depicting a typical donation and three different types of donations as well as the machine use during an apheresis collection (for plasma and platelet donations).
-
Just before the donation.
-
During the donation.
-
After the donation.
-
A whole blood donation.
-
The machine used during an apheresis collection.
-
A plasma donation.
-
A platelet donation.

Are you eligible? Take the quiz and find out.
What discourages blood donations?
[edit | edit source]There are many excuses

Oswalt’s comprehensive literature review from 1977 found that the most commonly recorded motivations not to donate were mainly; fear (of needles, blood, weakness, etc...), medical excuses, deferrals, reactions and inconvenience (Oswalt, 1977). Piliavin (1990) suggests that in addition to this, fear of AIDS and other blood transmitted viruses are also strong inhibitors despite the fact that contracting AIDS from donating is unsubstantiated (new sterilized needles are only ever used once before being properly disposed of after every donation).
The relationship between fear and avoidance of donations is well documented (Piliavin, 1990). Piliavin’s (1990) literature review found that 17% of non-donors stated that fear was the main motivation behind non-donations. Fear is also a concern among donors; out of 1144 Polish donors 47% acknowledged that fear was an initial worry, as well as feelings of weakness or queasiness (Pawliszyn, 1979). A survey administered to two college populations consisting of 187 females and 152 males, reported that before donations 77% were nervous, 37% were afraid of the needle and 28% worried about fainting or feeling weak or dizzy (Oswalt & Napoliello, 1974). Vavić and colleagues (2012) found that “First time donors (FTDs) were more frightened, showed anticipatory anxiety, were less sure they would donate again.” To counter this Vavić et al., (2012) suggest that if the FTDs who are more scared are acknowledged and attention is focused on diminishing their anxiety before they donate, this could influence them to return and donate again (Vavić et al., 2012)
Apheresis (plasma/platelet) donors reported that fear wasn't the main deterrent, but reactions were (Piliavin, 1990). This is seen as a more realistic fear as citrate toxicity, cold chills and other types of reactions have been reported to have occurred in roughly 25% of inactive donors (Piliavin, 1990). Although, a more recent study found that from a 5 year survey a total of 686 adverse reactions were recorded which amounted to 0.28% of all donations, and out of these reactions only 0.38% reported citrate toxicity (Crocco et al., 2009). Overall the results from the survey (of 240,596 donations) show there was low occurrence of reactions (0.28%). Also the researchers stated that of the reactions observed they were mild and resolved quickly lending to the conclusion that apheresis and blood donations are safe procedures (Crocco et al., 2009). Conversely, the groundless fear of contracting AIDS through donating is problematic as this is completely unsubstantiated and irrational but still contributing to collection difficulties (Piliavin, 1990). The interesting thing about these fears is that when rewards were introduced for donations in America, these fears were very easily overcome (Hagen, 1982).
Oswalt’s review found that most non-donors are discouraged from donating due to legitimate medical excuses such as weighing less than 45kg, low blood pressure, medication, and more (Oswalt & Napoliello, 1974). Other non-legitimate medical excuses are assumed to be rationalizations for not donating, in this case the best suggestion is that by Piliavin (1990, p. 449) “effective dissemination of information pertaining to these often invalid assumptions and the means by which they can be alleviated may aid in dispelling naïve preconceptions about medical exclusion from donation”.
Deferrals have been found to be psychologically distressing and are becoming more common due to the development of more rigorous exclusions criteria in response to emerging diseases such as from from overseas travels (e.g. the Mad Cow - Variant Creutzfeldt-Jakob disease (vCJD) in the UK) and testing limitations (e.g. during the undetectable ‘window’ period) (Piliavin, 1990; Godin, Conner, Sheeran, Bélanger‐Gravel, & Germain, 2007). This is more prominent among early donors where motivation to donate is vulnerable and temporary deferral decreases the probability that they will ever return (Piliavin, 1990). Overall, due to the permanent loss of these early donors and the loss due to permanent deferrals the need to increase retention and recruitment of eligible donors is becoming more critical (Piliavin, 1990).
Lastly, another discouragement to donations is time constraints (donation time, or perceptions of delay) and inconvenience of opportunity (appointment hours, or location of sites) (Piliavin, 1990). However the literature on this issue varies quite a bit. The Australian red cross states that "Time taken to donate is of high importance to donors and is a common inhibitor." (Australian Red Cross Blood Service, 2012 pg. 10). Pilivian (1990) found that regular donors complained about delays and the length of history-taking, apheresis donors were more discouraged by the time taken to donate, but FTDs aren't as concerned about time as they are about discomfort. One study found that perceptions of convenience increase the more the person gives blood, of their sample 54% of non-donors, 60% of FTDs, and 72% of regular donors thought the process was convenient (Gillespie & Hillyer, 2002). Some studies found convenience to be the second most significant deterrent, such as the convenience of the site where the donation takes place, and to mitigate this more mobile or fixed sites need to be based close to heavily populated areas (Drake, Finkelstein, & Sapolsky, 1982; Piliavin, 1990; Gillespie & Hillyer, 2002). Another study by the American Red Cross found that the actual waiting time had no relationship to whether a donor would return (Pilivian, 1990). Pilivian, (1990) suggests that since this is perceived not actual waiting time that is a problem a simple solution would be to help fill in the time by offering magazines, TV, and snacks/drinks.
In conclusion, most of these discouragements against donating is partly controllable through scheduling, collection personnel, dissemination of information and site location,(Piliavin, 1990) the other part will be covered in the Theory of Planned Behaviour section.
What motivates blood donations?
[edit | edit source]There are numerous motivations for why some people give blood, mainly these are altruism/humanitarianism, extrinsic rewards, awareness of community/personal need, emotional benefit, and social pressure (Moore, 2008; Piliavin, 1990) To better understand the strength these motivations have on people they will be categorized into two groups intrinsic, and extrinsic motivation. Intrinsic motivations are stronger influences they're internal, natural, and spontaneous, they engage one's interest due to the enjoyment of the task or for the challenge the task provides not due to any external regulations, whereas extrinsic motivations are less influential, external, and occur due to environmental influences (Reeves, 2009).
Intrinsic motivations
[edit | edit source]Altruism or altruistic behaviour is the act of doing something that benefits others at some personal cost without a reward (Piliavin, Callero, & Evans, 1982). Altruism has been considered one of the main motivations for donating as shown in many studies (Oborne, Bradley, & Lloyd‐Griffiths, 1978; Piliavin et al., 1982; Piliavin, Evans, & Callero, 1984; Steele et al., 2008; Tyano, Munitz, & Wijsenbeek, 1975). In Steele and colleagues’ work they found frequent donors displayed higher altruistic, and social responsibility scores (Steele, et al., 2008). Although the effect this study found was significant, practically it was not very large; the study showed an increase of 10% of the mean of altruistic behaviour would only result in an increase of 0.17 donations over 5 years (Steele, et al., 2008). Furthermore, studies show there is a slow decline in the expression of altruism within today’s society compared to the past; older donors are seen to have higher altruistic behaviour, which is suggested to be due to older donors being brought up in a society that put more value on helping strangers however nowadays helping a stranger is seen as risky behaviour (Steele, et al., 2008). Thus in a society such as this there is dwindling hope that using appeals based on altruism will improve motivations towards blood donations.
Conversely, many studies say pure altruism doesn't exist as donors benefit emotionally from donating such as receiving an emotional "warm glow" feeling (Ferguson, Farrell, & Lawrence, 2008). Ferguson and colleagues (2008) found that people are more likely to help when they find it personally rewarding. Their study examined whether egoistic beliefs would be a better predictor of donation behaviour compared to altruistic beliefs. (Ferguson, et al., 2008). They found that blood donor motivation was partly selfish and suggested that blood donation appeals should focus on benevolent (self-serving) rather than altruistic motivations, such as reminding people that one day they may need blood (Ferguson et al., 2008).
Another intrinsic motivation is blood donor self-identity. Self-identity reflects the extent to which individuals perceive themselves as performing a particular societal role. The more an individual perceives they fit a particular societal role, the more influence self-identity will exert on behaviour. Development of a blood donor identity is suggested to occur after the third to fifth donations, thus more a donor donates the more they develop an intrinsically motivated, role identity and the more resistant they become to potential negative disturbances such as inconvenience, mild reactions or temporary deferrals (Ringwald, Zimmermann, & Eckstein, 2010). In summary, intrinsic motivations are stronger motivators but they are much harder to influence.
Extrinsic Motivations
[edit | edit source]
The debate regarding whether or not extrinsic incentives should be used has been going on quite a while. Titmuss’ (1970) who essentially started the debate in his book “The gift relationship”, hypothesised that incentives (especially monetary types) would be economically inefficient and would have a negative motivational crowding-out effects. That is when high incentives are introduced, a lower supply will be produced (Niza, Tung, & Marteau, 2013). Titmuss (1970) stated that altruism improves social unity and social affluence and is therefore essential to a healthy society which is why a voluntary blood-giving system works and is a better motivator than a monetary reward system (Oakley & Ashton, 1997). Although none of Titmuss’ hypotheses were backup with empirical evidence (Niza et al., 2013). Despite this some studies found Titmuss to be correct that introducing monetary rewards would not increase the likelihood of donating among non-donors, and often people who prefer monetary rewards for donating are less likely to have ever donated. Yet those who have donated do accept non-monetary rewards (Drake, 1978; Costa-i-Font, Jofre-Bonet, & Yen, 2013) which would indicate that extrinsic monetary rewards are ineffective yet other extrinsic incentives may be effective.
Non-financial incentives, such as t-shirts, mugs, and medical tests is considered a commonly acceptable way to incentivize blood donation (Niza et al., 2013). For instance the American Red Cross runs over 7000 blood drives per year where roughly 40% of these blood drives offer an extrinsic incentive such as T-shirts, coupons, coolers and many other forms of merchandise (Lacetera et al., 2011). Non-financial extrinsic incentives are commonly used in Australia as well, such as snacks, cold drinks, stickers, key chains and more. Lacetera and Macis (2010) study which involved administering surveys to 467 blood donors Italy, that financial incentives such as 10 Euros in cash would discourage people to donate but a voucher of the same amount would not. However as the researchers noted, when using a self-report questionnaire type of research no one can be completely certain that actual behaviour won't differ from the answers recorded to a hypothetical scenario (Lacetera & Macis, 2010).
A longitudinal field experiment that tested whether economic incentives really did have an effect on blood donations was performed by Lacetera and Macis (2011). However due to the explicit rules set by the U.S. Department of Health and Human Services no cash incentives were allowed to be given in exchange for “voluntary” blood donations (Lacetera et al., 2011). Therefore experimenters were required to use gift cards as the economic incentives. The study involved around one hundred thousand individuals and they found that informing participants of a reward dramatically increased donations, which the researchers suggested that this could be an effective way of gaining more donations during period of increased shortage. On the other hand individuals given surprise rewards (uninformed of rewards before donating) decrease the likelihood that they would return (Lacetera et al., 2011). This result highlights the main problem with extrinsic rewards; if the person is motivated intrinsically to perform an activity and an extrinsic reward is introduced, this undermines future intrinsic motivations (Reeve, 2009, pp. 121-122). Also another problem is the economic inefficacy of constant extrinsic rewards; it is very expensive and once the reward stops so does the behaviour (Skinner, 1958).
Then again extrinsic motivations don't have to be tangible, social pressure is also useful as mentioned in Pilivian’s (1990) review; pressure to conform to the expectations of others is very motivating. He suggests that in order to recruit more donors appeals need to use face-to-face solicitation, a personal reminder the day before planned donation, personally calling eligible donors to organise appointments, and have an opt-out system where donors are automatically given their next appointment after each donation and have to consciously decide not to give (Piliavin, 1990). Also another non-tangible motivator is the awareness of the need for blood, as Drake and colleagues (1982) found many people weren't donating because they weren't unaware of the need. The red cross in New Mexico successfully changed their paid donor system to voluntary by appealing to the public stating that blood is needed to save many lives and that everybody's contribution is important (Piliavin, 1990).
Theory of Planned Behaviour
[edit | edit source]
The most common theoretical approach to donor motivation is The theory of Planned Behaviour (TPB; Giles, McClenahan, Cairns, & Mallet, 2004; Armitage & Connor, 2001; Ringwald, Zimmermann, & Eckstein, 2010). TPB emphasizes that human behaviour is directed by personal attitudes, social pressures and a sense of control, that behaviour is determined by the intentions of individuals (see figure 1) aka their explicit plans or motivations to commit a specific act (Ajzen, 1991). For example, individuals are more likely to execute rather than neglect their intentions, such as if an individual sets up a plan to donate blood they're more likely to actually do it. Therefore, (as mentioned above) applying non-tangible (social pressure) extrinsic motivations to motivate donations would be very effective in recruiting and retaining donors. Additionally Armitage and Connor (2001) suggest that in order to improve intentions to donate blood, we need to emphasize the moral issues surrounding blood donation, influence personal attitudes in the importance of donations by creating awareness of the need.
However in relation to planned behaviour self-efficacy was more influential in predicting intentions than perceived sense of control (Giles, et al., 2004). Armitage and Connor (2001) found self-efficacy was the dominant determinant of intention and therefore represents the variable with the most potential for intention and behaviour change. Specifically, lowered self-efficacy is associated with fear of needles, lack of previous experience, perceived inadequate health status, and the perception that donating blood takes a long time (Giles et al., 2004). To increase self-efficacy especially for FTDs Giles and colleagues (2004) suggest making the donation process as positive as possible by complimenting donors, thanking them and reminding them of the contribution they've made, providing positive feedback, and modelling successful donation. Also through successful donations donors can increase their self-esteem by personal mastery of fear (Bandura, 1997).It is very important that self-efficacy is supported throughout a donor's career to maintain their positive attitudes towards donating and encourage donors to donate as often as they can as this builds up a blood donor self-identity and blood donations become habit and intrinsically motivated (Ringwald, et al., 2010).
From this theory the practical implications to increase both intrinsic and extrinsic motivations are to recruit more donors by using social pressure, creating awareness of the need, and using techniques to increase self-efficacy (e.g. modelling), then retain more donors by increasing self-efficacy, appeal to blood donor self-identity, emphasize the moral issues surrounding blood donation, and apply social pressure (e.g.use face-to-face solicitation). Example
Putting it all together
[edit | edit source]The key elements to encourage more blood donations are:
- Acknowledge FTDs reduce/prevent adverse events and the blood donor's anxiety.
- Use appropriate incentives.
- Use personal aspects to motivate blood donors.
- Make blood donations convenient.
- Distribute information aimed at dispelling misconceptions
- Fill in waiting times.
- Support the role of the blood donor's identity.
- Use social pressure.
- Create awareness of the need.
- Compliment donors (they're saving lives after all).

Quiz
[edit | edit source]
Conclusion
[edit | edit source]Blood is an important life saving resource and in order to effectively motivate more people to donate we first need to understand the motivations behind why people do and don't donate (see table 1).
Table 1 Summary of the motivations behind blood donations.
| Motivations not to donate | Motivations to donate |
|---|---|
| Fear | Altruism |
| Inconvenience | Extrinsic rewards |
| Medical excuses | Emotional benefit |
| Deferrals | Social Pressure |
| Reactions | Need |
Most of the discouragements against donating are controllable as through scheduling, collection personnel, dissemination of information and site location. Balancing the effect of extrinsic rewards on current and potential donors is difficult; if the reward is too high intrinsically motivated donors may be insulted, but if it’s too low then incentive seekers will not be motivated. Also there is the problem that rewards aren't economical, and they will disrupt the development of intrinsic motivation (Pilivan, 1990). The best approach is to motivate people both intrinsically and extrinsically and this can be done using the theory of planned behaviour through influencing personal attitudes, social pressures and self-efficacy.
References
[edit | edit source]Armitage, C. J., & Conner, M. (2001). Social cognitive determinants of blood donation. Journal of Applied Social Psychology, 31 (7), 1431-1457.
Australian Bureau of Statistics, [ABS] (2013). Australian Demographic Statistics, Mar 2013 , viewed 27 October 2013, http://www.abs.gov.au/ausstats/abs@.nsf/mf/3101.0
Australian Red Cross Blood Service. (2013). Blood Service Statistics . Retrieved from www.donateblood.com.au/files/2013BloodServiceStatisics_S.pdf
Australian Red Cross Blood Service. (2012). Annual report 2011 -2012 . Retrieved from http://www.donateblood.com.au/files/pdfs/2012_Blood_Service_Annual_Report.pdf
Bandura. (1997) Self-efficacy: The Exercise of Control . Freeman, New York.
Costa-i-Font, J., Jofre-Bonet, M., & Yen, S. T. (2013). Not all incentives wash out the warm glow: the case of blood donation revisited. Kyklos, 66 (4), 521-543.
Crocco, I., Franchini, M., Garozzo, G., Gandini, A. R., Gandini, G., Bonomo, P., & Aprili, G. (2009). Adverse reactions in blood and apheresis donors: experience from two Italian transfusion centres. Blood transfusion, 7 (1), 35.
Drake, A. W. (1978). Public attitudes and decision processes with regard to blood donation . Cambridge, Massachusetts: Operations Research Center, Massachusetts Institute of Technology. 1-139
Drake A.W., Finkelstein S.N., Sapolsky H.M. (1982) The American Blood Supply . Cambridge, MA, MIT Press.
Ferguson, E., Farrell, K., & Lawrence, C. (2008). Blood donation is an act of benevolence rather than altruism. Health Psychology, 27 (3), 327.
Giles, M., McClenahan, C., Cairns, E., & Mallet, J. (2004). An application of the theory of planned behaviour to blood donation: the importance of self-efficacy. Health education research, 19 (4), 380-391.
Gillespie, T. W., & Hillyer, C. D. (2002). Blood donors and factors impacting the blood donation decision. Transfusion medicine reviews, 16 (2), 115-130.
Godin, G., Conner, M., Sheeran, P., Bélanger‐Gravel, A., & Germain, M. (2007). Determinants of repeated blood donation among new and experienced blood donors. Transfusion, 47 (9), 1607-1615.
Hagen, P. J. (1982). Blood: Gift or Merchandise: towards an international blood policy: AR Liss New York.
Lacetera, N., & Macis, M. (2010). Do all material incentives for pro-social activities backfire? The response to cash and non-cash incentives for blood donations. Journal of Economic Psychology, 31 (4), 738-748.
Lacetera, N., Macis, M., & Slonim, R. (2011). Rewarding altruism? A natural field experiment (No. w17636). National Bureau of Economic Research.
Linden, J. V., Gregorio, D. I., & Kalish, R. I. (1988). An estimate of blood donor eligibility in the general population. Vox Sanguinis, 54 (2), 96-100.
Masser, B. M., White, K. M., Hyde, M. K., Terry, D. J., & Robinson, N. G. (2009). Predicting blood donation intentions and behaviour among Australian blood donors: Testing an extended theory of planned behaviour. Transfusion 49, 320 – 329.
Moore, R. J. (1991), Promoting blood donation: a study of the social profile, attitudes, motivation and experience of donors. Transfusion Medicine, 1 (4), 201–207.
Niza, C., Tung, B., & Marteau, T. M. (2013). Incentivizing blood donation: Systematic review and meta-analysis to test Titmuss’ hypotheses. Health Psychology, 32 (9), 941.
Oakley, A., & Ashton, J. (1997). The gift relationship: from human blood to social policy. London School of Economics and Political Science,(LSE).
Oborne, D., Bradley, S., & Lloyd‐Griffiths, M. (1978). The anatomy of a volunteer blood donation system. Transfusion, 18 (4), 458-465.
Oswalt, R. M. (1977). A review of blood donor motivation and recruitment. Transfusion, 17 (2), 123-135.
Oswalt, R. M., & Napoliello, M. (1974). Motivations of blood donors and nondonors. Journal of Applied Psychology, 59 (1), 122.
Pawliszyn, W. (1979). [Efficiency of the propaganda for volunteer blood donation in the opinion of blood donors]. Polski tygodnik lekarski (Warsaw, Poland: 1960), 34 (45), 1771.
Piliavin, J. A. (1990). Why do they give the gift of life? A review of research on blood donors since 1977. Transfusion, 30 (5), 444-459.
Piliavin, J. A., Callero, P. L., & Evans, D. E. (1982). Addiction to altruism? Opponent-process theory and habitual blood donation. Journal of Personality and Social Psychology, 43 (6), 1200.
Piliavin, J. A., Evans, D. E., & Callero, P. (1984). Learning to "give to unnamed strangers": The process of commitment to regular blood donation. Development and Maintenance of Prosocial Behavior: International Perspectives on Positive Morality, Plenum Press, New York.
Reeve, J. (2009). Understanding motivation and emotion (5th ed.): Wiley New York.
Ringwald, J., Zimmermann, R., & Eckstein, R. (2010). Keys to open the door for blood donors to return. Transfusion medicine reviews, 24 (4), 295-304.
Skinner, B. F. (1958). Reinforcement today. American Psychologist, 13 (3), 94.
Staallekker, L., Stammeijer, R., & Wit, C. (1980). A Dutch blood bank and its donors. Transfusion, 20 (1), 66-70.
Steele, W. R., Schreiber, G. B., Guiltinan, A., Nass, C., Glynn, S. A., Wright, D. J., . . . Smith, J. W. (2008). The role of altruistic behavior, empathetic concern, and social responsibility motivation in blood donation behavior. Transfusion, 48 (1), 43-54.
Titmuss, R. M. (1970). The gift relationship: From human blood to social policy. London, UK: George Allen and Unwin.
Tyano, S., Munitz, H., & Wijsenbeek, H. (1975). Psychological and sociological aspects of blood donation in Israel]. Revue française de transfusion et immuno-hématologie, 18 (3), 326.
Vavić, N., Pagliariccio, A., Bulajić, M., Marinozzi, M., Miletić, G., & Vlatković, A. (2012). Blood donor satisfaction and the weak link in the chain of donation process. Transfusion and Apheresis Science.
Weiner, B. (1985). An attributional theory of achievement motivation and emotion. Psychological Review, 92 (4), 548-573.
Whittemore, S. (2009). The circulatory system. New York, NY: Infobase Publishing.
World Health Organization. (2009). Availability, safety and quality of blood products. Retrieved from http://apps.who.int/gb/ebwha/pdf_files/WHA63/A63_20-en.pdf